- Dermatology Times, November 2022 (Vol. 43. No. 11)
- Volume 43
- Issue 11
Disadvantages of Excision for Melanoma
At the Melanoma Update of the Annual ASDS Meeting, Tyler Hollmig, MD, looked at complex clinical scenarios when treating melanoma and the continued challenges dermatologists face.
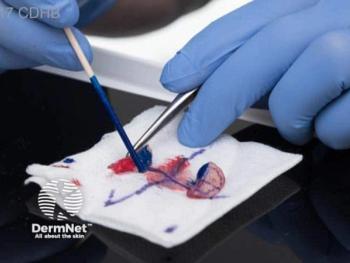
To begin his updates on treatment methods for melanoma, Tyler Hollmig, MD, director of dermatologic surgery in the department of internal medicine at the University of Texas at Austin Dell Medical School in Austin, Texas, reiterated that the incidence of melanoma has risen substantially over the last few decades. According to Hollmig, lifetime risk now is over one in 50. Traditionally, melanoma is treated by excision with a recommended margin of healthy-appearing skin. The specimen is then fixed in formalin and vertically sectioned, like a bread loaf. The sections allow for visualization and staging of the central tumor. But Hollmig also states that excisional surgery is not perfect, it has disadvantages as well.
Hollmig points out 4 major disadvantages of excisional surgery. First, traditional excision does not completely examine the margin, which creates an increased risk of false negative margins. Most pathologists will cut sections about every 3 to 4 millimeters, which studies show allows pathologists to visualize approximately 25% of the margin. To see all of the margin using cut sections, pathologists would have to cut at .01 millimeter increments, which is impossible, according to Hollmig.
Another disadvantage of excision is that historically, margin guidelines, particularly for melanoma in situ, have been inadequate. Hollmig points out that the inadequacy of guidelines has been well documented in melanoma literature. The National Comprehensive Cancer Network (NCCN) guidelines now recommend 0.5-to-one-centimeter margins for melanoma in situ.
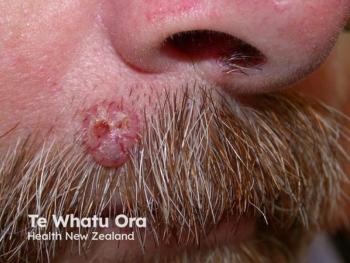
“We know, however, that when excisions with narrower margins than recommended are taken, there's a 5 times increased risk of having positive margins. And we know now that 0-millimeter margins are necessary to clear 97% of melanoma in situ and melanoma on the trunk and extremities. Twelve-millimeter margins are necessary to clear the same proportion of tumors arising on the head and neck,” said Hollmig. “For so-called ‘specialty site’ melanomas defined as melanomas arising on the head, neck, genitalia, and pre-tibial shins, there is a 5 times higher risk of positive margins than other sites. In fact, one out of 4 excisions of head and neck melanomas has positive margins.”
The third disadvantage of excisional surgery is that local recurrence is not uncommon. Anywhere from 9%-15% local recurrence has been reported in the special group of head and neck lesions. Hollmig notes that is a key rate because when melanoma in situs recur, approximately a quarter of the time, there will be an invasive focus. When melanomas recur, approximately 1/3 of the time, there is a deeper Breslow depth, bringing major consequences.
According to Hollmig, the fourth disadvantage of excision is the delay between excision and margin assessment. Some Mohs surgeons see reconstructions done before the margin has been shown as negative, which is not ideal. Trying to find positive margins after a flap repair is extremely difficult. Overall, it can also take a long time to achieve clear margins. Hollmig stressed to colleagues that lengthy reconstruction processes due to excision procedures can negatively impact patients and their quality of life.
Reference:
- Hollmig T. Melanoma Update. Presented at: 2022 American Society of Dermatologic Surgery Annual Meeting, Denver Colorado, October 7-10, 2022.
Articles in this issue
about 3 years ago
New Tech for Skinabout 3 years ago
Update on New Laser Treatments for Acneabout 3 years ago
Are You Prepared for Potential Tax Law Changes?about 3 years ago
Genetic Profiling and the Future of Therapeutics in Dermatologyabout 3 years ago
Low-Dose Oral Minoxidil for Hair Growthabout 3 years ago
The Role of Precision Medicine in the Management of Melanomaabout 3 years ago
The Latest Buzz in Atopic Dermatitisabout 3 years ago
Hand Healthabout 3 years ago
Hidradenitis Suppurativa: Current and Future TreatmentsNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.