- Dermatology Times, November 2022 (Vol. 43. No. 11)
- Volume 43
- Issue 11
New Tech for Skin
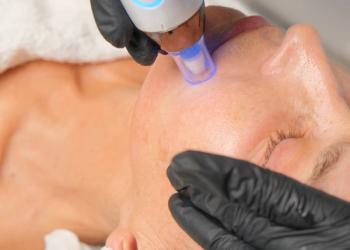
There are many innovative and exciting developments coming to the dermatology space, both energy-based devices and injectables.
There are many innovative and exciting developments coming to the dermatology space, both energy-based devices and injectables. These will expand the armamentarium of the dermatologist to deliver minimally invasive results that can help reduce and smooth wrinkles, add volume, and rejuvenate the skin. Additionally, treatments that can provide long-term improvement of acne are finally on the horizon.
Accure:
Accure is a novel 1726-nm wavelength laser for the selective targeting of sebum. It is pending FDA approval for the treatment of acne. However, it is far more than just a wavelength. To effectively “thread the needle” of effective thermal effect while avoiding complications, the design of a unique temperature monitoring and pulsing gradient strategy has proven equally critical to the device’s clinical performance and safety profile. Using this methodology has allowed Accure to determine an optimal sebaceous gland damage temperature target and corresponding peak epidermal temperature end point (PET). This is a patented and unique dosimetry engine that gives the operating clinician an instant, real-time feedback measurementof the PET during each pulse of the treatment to ensure safety, consistency, and confidence of the energy delivery and corresponding clinical impact. 5
Daxxify:
Daxxify is the first and only neuromodulator stabilized with peptide exchange technology for frown lines, crow’s-feet, and other facial lines. The peptide-powered frown treatment’s main differentiators from current neuromodulators are that it can sustain its effect for 6 months and that it has worked for up to 9 months in some patients. Daxxify’s duration benefits were established in phase 3 trials that included 2,700 patients and 4,200 treatments. 6
Luminera/HArmonyCA:
HArmonyCA is a new generation of dermal filler for the face that is based on a composite matrix of cross-linked hyaluronic acid with embedded calcium hydroxyapatite microspheres. This provides an immediate volumizing effect due to the hyaluronic acid while providing a long-lasting effect whereby the calcium hydroxyapatite microspheres form a scaffold and promote fibroblast stimulation of new collagen production. An added benefit and safety feature is that the entire HArmonyCa product is susceptible to hyaluronidase and thus can be dissolved.7
Avava:
The Avava PL-1 is a Q-switched 1064 laser with microbeam handpiece. Avava’s breakthrough is a new class of focused intradermal laser products powered by Focal Point Technology to deliver energy at any depth with pinpoint accuracy for ideal patient outcomes. This 3D technology combined with Avava’s proprietary Skin AI visualization allows skin aging and pigment to be treated safely and effectively for all Fitzpatrick skin types.
Ellacor
The ellacor System by Cytrellis BioSystems received FDA clearance in July 2022 and is based on the novel concept of tissue micro-coring. Invented at Massachusetts General Hospital and Harvard Medical School by R. Rox Anderson, MD, and Jay Austen, MD, ellacor utilizes hollow needles to penetrate the epidermis and dermis in order to extract thousands of columns or micro-cores of skin, thereby reducing the overall density of the skin. Because the diameter of the needles is less than 0.5 mm, the extracted cores are on the micro-scale, thereby mitigating the possibility of scarring.1
Ellacor is indicated for use in the treatment of moderate to severe wrinkles of the mid and lower face for Fitzpatrick skin types I to IV. It has not been clinically tested for skin types V and VI. The actual mechanism of action is skin removal and skin rejuvenation through neocollagenesis and elastinogenesis prompted by the natural healing of the skin after the controlled, mechanically induced injury.
The system consists of a console, a handpiece, a foot switch, and a vacuum system that includes a pump, a filter, and suction tubing. A single-patient, disposable needle cartridge attaches to the handpiece and is used to perform the procedure.
The user interface on the console is used to input basic patient information such as patient gender and age range, whether they are a new or existing patient, and if they have already had an ellacor procedure. You can also select and adjust the percentage of skin to be removed throughout the procedure, which changes the travel pattern of the needles. User selections are 1%, 3%, 5%, 7%, and 8%. A higher percentage of skin removal corresponds to a greater number of cores being removed for a more aggressive treatment. You can also select and change the penetration depth of the needles in 0.5-mm increments from 0.0 mm to 4.0 mm as you move around the anatomy, thereby customizing the procedure for each patient.
Patient selection based on skin quality, underlying conditions, and other procedures that could adversely impact outcomes, as well as setting the right level of patient expectation, are important during initial patient consultation as patient experiences may vary. The procedure usually takes about 30 minutes and is typically performed under local injectable anesthesia, and in my experience the pain experienced by patients during the procedure is mild.
Clinical trials performed with the ellacor system have typically included up to 3 procedures per patient with an average downtime of 3 to 5 days. There have been a few reports of prolonged redness and healing, but these typically resolve without further sequelae.2
Although the ellacor system is currently indicated for treating rhytides of the mid and lower face, the utility of this technology is just being realized and opens up the potential for many over clinical applications beyond wrinkles and beyond the face. There are several studies currently underway to explore the possible benefits over existing technologies.
Resonic
Resonic received FDA clearance in mid-2021 and relies on the novel proprietary use of sound to treat cellulite3 and remove tattoos4 all over the body. The device is owned by AbbVie, which acquired Soliton, the parent company of Resonic. The proprietary platform technology relies on a rapid acoustic pulse and was licensed from The University of Texas on behalf of MD Anderson Cancer Center. Resonic uses rapid pulses of acoustic shock waves for the treatment of cellulite and as an accessory to lasers for the removal of unwanted tattoos.
Resonic offers a truly noninvasive approach to treating cellulite. Clinical studies showed a roughly 30% improvement in cellulite appearance at 12 weeks with high satisfaction responses (~93%) among study participants with minimal pain experienced during treatments. An important differentiator is that there is no postprocedure recovery with Resonic, in contrast to other new methods of treating cellulite that are minimally invasive and require some postprocedure recovery.
Resonic also offered some potentially exciting advances in treating unwanted tattoos. Despite the development of picosecond lasers, tattoo removal remains challenging and often takes more treatments than patients and physicians would like. The Resonic device is used in combination with traditional laser tattoo removal technology and generates acoustic shock wave pulses that clear epidermal and dermal vacuoles to enable multiple laser passes in a single office laser tattoo removal session. In the clinical study, the combination of a Q-switched laser and Resonic showed a dramatic increase in average fading (44.2%) vs laser only (24.8%). The ability to lighten and clear tattoos faster is a major advance in our abilities to treat unwanted tattoos.
Resonic has currently undertaken a limited commercial launch, placing the device in a small number of dermatology and plastic surgery practices.
References
1. Champlain, A. et al. 2019. What is the Largest Size Full-Thickness Skin Injury That Can Heal Without a Scar? Lasers in Surgery and Medicine, 50(S30), S30-31.
2. Pivotal Study to Evaluate the Effectiveness of a Micro-Coring Device Treating Moderate to Severe Facial Wrinkles; submitted for publication.
3. Tanzi EL, Capelli CC, Robertson DW, et al. Improvement in the appearance of cellulite and skin laxity resulting from a single treatment with acoustic subcision: findings from a multicenter pivotal clinical trial. Lasers Surg Med. 2022;54(1):121-128. doi:10.1002/lsm.23448
4. Kaminer MS, Capelli CC, Sadeghpour M, Ibrahim O, Honda LL, Robertson DW et al. Increased tattoo fading in a single laser tattoo removal session enabled by a rapid acoustic pulse device: a prospective clinical trial. Lasers Surg Med. 2020;52(1):70-76. doi:10.1002/lsm.23163
5. Tanghetti E, Geronemus R, Bloom B, Anderson RR, Ross EV, Sakamoto FW. Safety and efficacy data in a pilot study of the treatment of acne with a fiber laser. Poster presented at: 2020 American Society for Laser Medicine Annual Conference; April 29-May 3, 2020; Phoenix, AZ.
6. Fabi SG, Cohen JL, Green LJ, et al. DaxibotulinumtoxinA for injection for the treatment of glabellar lines: efficacy results from SAKURA 3, a large, open-label, phase 3 safety study. Dermatol Surg. 2021;47(1):48-54. doi:10.1097/DSS.0000000000002531
7. Yag-Howard C, DeNigris J. Novel filler technique: Hyaluronic acid and calcium hydroxylapetite mixture resulting in favorable esthetic and longevity outcomes. Int J Womens Dermatol. 2021;7(5 Pt B):817-819. doi:10.1016/j.ijwd.2021.09.008
Articles in this issue
about 3 years ago
Update on New Laser Treatments for Acneabout 3 years ago
Are You Prepared for Potential Tax Law Changes?about 3 years ago
Genetic Profiling and the Future of Therapeutics in Dermatologyabout 3 years ago
Low-Dose Oral Minoxidil for Hair Growthabout 3 years ago
The Role of Precision Medicine in the Management of Melanomaabout 3 years ago
The Latest Buzz in Atopic Dermatitisabout 3 years ago
Hand Healthabout 3 years ago
Hidradenitis Suppurativa: Current and Future Treatmentsabout 3 years ago
How to Have a Proper Presence on Social MediaNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.