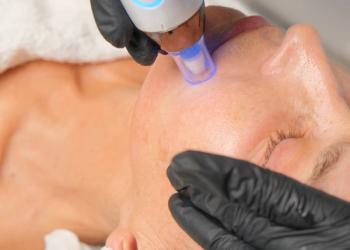
Laser-Assisted Drug Delivery
The use of laser-assisted drug delivery (LADD) is gaining momentum as the novel technique enables a more efficient delivery of drug to the lesion.
Ever since its inception about 20 years ago, laser-assisted drug delivery (LADD) has come a long way, becoming more fine-tuned and finding its use in several different areas and medical specialties. However, along with the expanding indications of the novel treatment approach comes responsibility and attention to safety in its increasingly popular use. In a recent study,1 researchers aimed to develop recommendations for the safe and effective use of LADD with the goal of offering a framework for clinicians to better manage LADD treatment in their patients.
“Unfortunately, there have been some bad players using LADD––some are not professional doctors but instead medi[cal]-spa people who are topically applying cosmeceuticals that are causing granulomas. There are things [regarding which] we do not know what happens if you topically apply them because they were never intended for that use. This underscores the need for us to get on the same page regarding how and when to safely apply the LADD technique,” said study coauthor Jill S. Waibel, MD, medical director and owner of Miami Dermatology and Laser Institute, subsection chief of dermatology at Baptist Hospital, Miami, and medical director of Miami Cancer Institute Multidisciplinary Skin Cancer Clinic in Florida.
LADD augments the distribution and penetration of topically applied treatments, leading to enhanced delivery and bioavailability. Over the years, LADD has been found to be useful in various indications, including nonmelanoma skin cancer (NMSC), vitiligo, melasma, scarring, photodamaged skin, alopecia, and onychomycosis. It has also proved beneficial for vaccination, local anesthesia, analgesia, viral warts, infantile hemangiomas, and cosmetic uses. It can be argued that the ever-increasing and expanding indications for LADD have outpaced the explicit need for a safe and effective clinical guideline to be established, which would clearly be useful for clinicians when implementing this very promising therapeutic approach.
“The exciting thing that our paper really highlights is that LADD is a very effective way to enhance the delivery of therapeutics. Right now, we have pills, IVs, and patches to deliver medicines. This is a new cutaneous delivery system where you will need [fewer] drugs because when you get it directly in the bloodstream, you don’t go through the first pass effect via the stomach, resulting in decreased toxicity, because you are not giving as much medicine. And there is a huge cost reduction,” said Waibel, who is also a clinical voluntary assistant professor at the University of Miami in Florida.
The study, a systematic literature review, looked at publications reporting research on LADD, and a multidisciplinary panel was convened to draft recommendations informed by the systematic review. The guideline’s 15 recommendations address 5 areas of LADD use: (I) indications and contraindications; (II) parameters to report; (III) optimization of drug delivery; (IV) safety considerations; and (V) prophylaxis for bacterial, viral, and fungal infections. The recommendations are as follows.
I. Indications and Contraindications
1. We recommend the use of LADD in adults and adolescents with all Fitzpatrick skin types.
2. We suggest that LADD may be safely used in patients with immunosuppression disorders.
3. We recommend the use of LADD for the treatment of actinic keratoses, actinic cheilitis, and cutaneous squamous cell carcinoma in situ.
4. We suggest the use of LADD for the treatment of hypertrophic scars and keloids.
5. We recommend the use of LADD for epidermal and dermal analgesia if there is sufficient time for application.
6. We recommend LADD be deferred in patients with known allergy to the drug being delivered or active local skin infection, or who have an underlying medical problem or enzyme abnormality if the drug is at risk of worsening the abnormality.
II. Parameters to Report
7. We recommend that the following parameters be reported when performing AF and NAF LADD: fluence/channel depth, density/surface area, spot size, incubation time (time between laser delivery and medicine application), number of passes, and total volume and type of formulation of medication applied.
III. Optimization of Drug Delivery
8. We suggest that drug delivery via LADD may be increased by using heat, pressure, occlusion, and/or low viscosity drug formulations.
9. We suggest that AF laser settings be selected to ensure that the expected channel diameter is greater than the diameter of the particle being delivered.
10. We suggest that cold, nonhollow bore microneedling (without heat/radiofrequency) or radiofrequency microneedling may be alternative modalities to laser for drug delivery.
IV. Safety Considerations
11. We recommend that physicians using LADD appreciate that there is a certain unpredictability of response and tissue levels of drug owing to variable pharmacokinetics.
12. We recommend that physicians using LADD be cautious because systemic adverse effects owing to inadvertent systemic delivery of medications are a possibility.
13. We recommend LADD be performed with appropriate eye protection (appropriate for the laser platform), surgical masks, and gloves, and suggest using a smoke evacuator, particularly with AF devices.
14. We suggest LADD only be used with medication formulations approved by a national regulatory authority for parenteral injection.
V. Prophylaxis for Bacterial, Viral, and Fungal Infections
15. We suggest use of the following prophylaxis regimens for AF and NAF LADD in otherwise healthy adults, pediatric patients, and patients who are immunosuppressed: antibiotic prophylaxis is not recommended when treating areas other than where wound healing might be impaired (eg, genitalia, lower legs); antiviral prophylaxis is recommended when LADD is used on the face or genitalia; and antifungal prophylaxis is not recommended.
“This [is a] technology-driven way to take topical drugs where you can do dosage timing and record keeping. I believe that it is time for this in our technology-driven world. Dermatology has really pioneered this approach because we are the laser people in creating these channels, but it really should touch every branch of medicine,” Waibel said.
Not only is LADD safe, she noted, but it is probably safer than traditionally used treatments. According to Waibel, who specializes in scar therapy, LADD is appropriate for scar treatment and significantly enhances outcomes.
“It’s a win-win because the lasers are treating scars and then you are [using] a medicine like Kenalog [triamcinolone] or 5-FU [5-fluorouracil] or something that will further help the lesion. You end up treating patients with [fewer] treatments and no needles, which can be very helpful in the pediatric population and needle-phobic patients,” Waibel explained.
Perhaps one of the main points emerging from the study concerns the treatment of NMSCs such as actinic keratosis (AK) and squamous cell carcinoma (SCC). Now with imaging techniques such as optical coherence tomography (OCT) and reflectance confocal microscopy (RCM), clinicians can better image margins and more precisely target those lesions amenable to LADD therapy.
“I work at the Miami Cancer Institute, and I literally have surgical and medical oncologists send me patients who have upwards of 50 SCCs on their legs and they ask me to perform LADD and try to get rid of some and shrink some lesions. So there is a real role here for noninvasive and nonsurgical skin treatment of skin cancers,” Waibel said.
Although LADD is not currently viewed as the gold standard treatment approach, Waibel pointed out that it can take time for a new technology to gain speed. Additionally, the current literature is showing that the novel treatment approach is slowly being adopted and explored.
Dermatologists have pioneered and are uniquely suited to perform LADD, said Waibel. The fractional ablative CO2 and erbium lasers allow the clinician to go anywhere from 5 µm to 4000 µm. According to Waibel, LADD is a revolutionary step forward in medicine and now the homework has been done.
“If you have 30 skin cancers on your lower leg, you can’t do 30 surgeries because that doesn’t make sense. But certainly, in 10 minutes, you can laser over each skin cancer. It is an incredible therapeutic approach, as the tunable laser allows you to deliver the drug more efficiently,” Waibel said.
When applying LADD in AKs, BCCs, and SCCs, the key is to get through the 10 to 15 µm of stratum corneum. Waibel will painlessly drill holes with the laser and then apply the aminolevulinic acid, a 30-minute incubation time followed by activation with the light.
“You are significantly cutting the time for the patient in the office and are getting much more increased efficacy of getting rid of the pre–skin cancers.
Now, instead of 3 hours, it’s only a 30-minute procedure. Laser-assisted drug delivery has caught on, but not as widely as it should have to date. If you are not doing this in your practice, you should consider it, safely and within these guidelines,” Waibel said.
A multidisciplinary skin cancer team should help determine whether LADD might be appropriate, taking into consideration other factors including patient fatigue and cost, or perhaps cases where surgery, radiation, and chemotherapy have failed. According to Waibel, when you are not successful with another therapy, LADD may be the way to go.
In dermatology, Waibel pointed out, the data in the literature show that only 1% to 5% of topical drugs get through the stratum corneum.
“…Think of how depressing that is and how many medicines are prescribed daily by dermatologists for topical applications that probably don’t ever get through. In LADD, we make these tiny little channels that are only 120 µm in diameter, and we can put anything we want down these channels, and they heal in 2 days. That’s pretty amazing, and it makes so much more sense,” she said.
The nonablative fractional lasers only disrupt the stratum corneum without causing an actual hole. As such, the ablative lasers do a much better job at delivery than the nonablative lasers.
When Waibel performs LADD in scars, the first laser addresses the color of the scar; this is followed by the ablative fractional erbium or CO2 laser and finally the LADD (the actual medicine application). As a result, improved outcomes are reached in fewer treatments, which is better and cheapter for the patient.
“I believe that LADD should become the gold standard. Without exception, [data from] every study that [have] been published on LADD [show it has] better efficacy over traditional drug delivery methods for the indication. Pioneered by dermatology, LADD can be used in all specialties and really change medicine,” Waibel said.
Disclosures: None relevant
Reference
Labadie JG, Ibrahim SA, Worley B, et al. Evidence-based clinical practice guidelines for laser-assisted drug delivery. JAMA Dermatol. Published online August 17, 2022. doi:10.1001/jamadermatol.2022.3234
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.