- Dermatology Times, September 2021 (Vol. 42, No. 9)
- Volume 42
- Issue 9
Preventing Keloid Recurrence With SRT

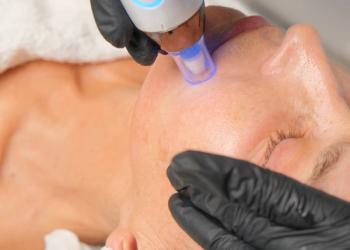
Part 2 of Dermatology Times®’ coverage of a strategic look at superficial radiation therapy (SRT) presented at the recent Music City SCALE Symposium for Cosmetic Advances & Laser Education 16th Annual Meeting details this therapy’s potential for reducing keloid recurrence.
Postsurgical superficial radiation therapy (SRT) could reduce the recurrence of keloids, Brian Berman, MD, PhD, professor emeritus of dermatology and cutaneous surgery at the University of Miami Miller School of Medicine and codirector of the Center for Clinical and Cosmetic Research in Aventura, both in Florida, said in his dermatology updates on this therapy at the Music City SCALE Symposium for Cosmetic Advances & Laser Education 16th Annual Meeting, August 18-22, 2021, in Nashville, Tennessee.1
Keloids commonly occur in high-visibility locations such as the face and earlobes. “When a patient comes to me with a keloid, I try to talk them out of surgery,” said Berman.
Without adjunctive therapy such as SRT, recurrence rates of keloids are high, according to Berman and in unpublished research, he reviewed 13 studies incorporating 343 patients and calculated a weighted average postkeloidectomy recurrence rate of 71.2%.2,3
“Very often, I’ll say, ‘You have a small keloid. If I were able to take away the burning, itching, and tenderness and get it softer and maybe a little flatter, would that be sufficient?’ And I hope they say yes, because there are other modalities to treat an existing keloid without cutting it out,” Berman said. With a referral-based practice, though, in his experience his patients typically want surgery because conservative treatments have failed.
Berman explains to patients that postsurgical SRT offers a noninvasive tool for reducing recurrence risk. Separate studies show that this treatment reduces postsurgical recurrence rates to 3.0% and 10.4%, respectively.4,5
“Dropping the recurrence rate from 7 out of 10 to 1 out of 10, with at least 1 year of follow-up, is very helpful to the clinician to be able to hold out hope to patients,” he said.6
Radiation therapy is believed to prevent keloid recurrence by reducing fibroblast proliferation, arresting the cell cycle, and inducing apoptosis.6 Although these mechanisms delay healing in normal skin, they are tailor-made for preventing keloids with their excessive scarring and for destroying malignant, abnormal cells in nonmelanoma skin tumors arising from fibroblast or keratinocyte hyperproliferation, according to Berman.
“The mechanisms are consistent, but there are different reasons why we’d use it for keloids versus a tumor,” he said. The SRT-100 is FDA 510(k) cleared for treating nonmelanoma skin cancers (NMSC) and keloids. Berman said colleagues have told him that they bought the machine for NMSC but now use it more often for postsurgical keloid recurrences.
Patients may worry about radiation therapy and carcinogenesis, according to Berman.
“I appreciate that. But I explain to them the historical safety of SRT, and the fact that it only goes a few millimeters deep at most into the skin, [meaning] it’s truly superficial radiation therapy,” he said.
Moreover, a 10-year retrospective analysis of 264 excised keloids, of which most received subsequent external-beam radiation or high dose-rate interstitial brachytherapy, showed no development of malignancy.7 Similarly, a search of Medline and PubMed between 1901 and March 2009 uncovered only 5 cases of carcinogenesis associated with, but not likely caused by, postkeloidectomy radiation therapy, Berman said. The cancers included basal cell carcinoma (BCC), thyroid cancer, breast cancer, and fibrosarcoma.
“Intuitively, it doesn’t make sense that radiation therapy induced the development of BCC because we use radiation therapy to treat BCC,” Berman said.
Breast cancers originate at deeper levels than SRT penetrates, and the noted thyroid cancer did not develop in the treated area, he added. The single fibrosarcoma investigators found was probably a fibrosarcoma before surgery, authors explained. These tumors typically take a decade to develop, Berman explained, whereas study follow up periods generally are considerably shorter.
Pacemakers implanted in the treatment area are a contraindication for SRT, in his opinion. Regarding adverse effects, Berman said he warns patients about the potential for post radiation pigmentary changes, most often hyperpigmentation.
In a chart review of 96 excised keloids followed for at least 1 year on which he was lead author, 56% of patients experienced hyperpigmentation.7 It is usually transient because less than 5% of patients experienced persistent hyperpigmentation, he noted.
Reclaiming Radiation Therapy
Regarding the safety and efficacy of SRT, Berman suggested that more dermatologists consider offering this therapy. “It’s part of our armamentarium to treat a patient who has disfiguring keloids that have an impact physically, cosmetically, and psychologically,” he said.
“The use of x-ray therapy was in the purview of dermatologists, historically,” said Berman. “Unfortunately, those machines ultimately broke down.”
According to Berman, around 30 years ago, manufacturers stopped making replacement parts. He continued to explain that the practice had stopped training residents how to use radiation therapy and then lead to radiation oncologists treating the skin with radiation therapy. These specialists typically favor other technologies such as electron-beam radiation, he said.
The SRT-100 platform offers dermatologists a high-tech, straightforward SRT option, according to Berman. Its user interface allows physicians to plug in treatment parameters. For keloids, guidelines suggest a biologically effective dose of 30 Gy delivered in 3 fractions of 6 Gy on 3 consecutive days post-surgery.8 The ultrasound feature is codified and user-friendly, adding only about an hour of training to the usual 1-to-1.5-day training period for the original device, he added.
“What’s nice about this machine is that it can be placed in the dermatologist’s office, and it does not require a radiation oncologist to run it,” Berman said. Along with lead shielding of sensitive body areas such as the eyes, thyroid, and genitals, using the machine requires a shielded room with lead in the drywall, which he says is easily installed.
Postkeloidectomy SRT is covered by insurance, added Berman, who has never been denied prior approval for this procedure. “You probably would have to get approval to do the surgery anyway. It’s not a significant increase in effort on the part of office staff.”
If a keloid recurs after SRT, Berman’s rule of thumb is never to repeat radiation therapy in the same anatomical area. Some excellent dermatologists do this, he said. However, he would rather avoid a therapy that has failed once. “And the skin does not ‘forget’ the original dose, which is concerning because there may be less data on the rate of malignancy development if you double or triple the dose,” Berman concluded.
Disclosures:
Berman is a consultant and investigator for Sensus. Goldberg reports no relevant financial interests.
References:
1. Berman B. Superficial radiation therapy for keloids. Presented at: Music City SCALE Symposium for Cosmetic Advances and Laser Education 16th Annual Meeting; August 18-22, 2021; Nashville, Tennessee.
2. Shaffer JJ, Taylor SC, Cook-Bolden F. Keloidal scars: a review with a critical look at therapeutic options. J Am Acad Dermatol. 2002;46(2 Suppl Understanding):S63-S97. doi:10.1067/mjd.2002.120788
3. Berman B, Nestor MS, Gold MH, Goldberg DJ, Fox J, Schmieder G. Low rate of keloid recurrences following treatment of keloidectomy sites with a biologically effective dose 30 of superficial radiation. SKIN The Journal of Cutaneous Medicine. 2018;2(6):402-403. doi:10.25251/skin.2.6.7
4. Berman B, Nestor MS, Gold MH, Goldberg DJ, Weiss ET, Raymond I. A retrospective registry study evaluating the long-term efficacy and safety of superficial radiation therapy following excision of keloid scars. J Clin Aesthet Dermatol. 2020;13(10):12-16.
5. Liu X, Liu JZ, Zhang E, et al. Impaired wound healing after local soft x-ray irradiation in rat skin: time course study of pathology, proliferation, cell cycle, and apoptosis. J Trauma. 2005;59(3):682-690.
6. Hoang D, Reznik R, Orgel M, Li Q, Mirhadi A, Kulber DA. Surgical excision and adjuvant brachytherapy vs external beam radiation for the effective treatment of keloids: 10-year institutional retrospective analysis. Aesthet Surg J. 2017;37(2):212-225. doi:10.1093/asj/sjw124
7. Ogawa R, Yoshitatsu S, Yoshida K, Miyashita T. Is radiation therapy for keloids acceptable? The risk of radiation-induced carcinogenesis. Plast Reconstr Surg. 2009;124(4):1196-1201. doi:10.1097/PRS.0b013e3181b5a3ae
8. Nestor MS, Berman B, Goldberg D, et al. Consensus guidelines on the use of superficial radiation therapy for treating nonmelanoma skin cancers and keloids [published correction appears in J Clin Aesthet Dermatol. 2019;12(6):14]. J Clin Aesthet Dermatol. 2019;12(2):12-18.
Articles in this issue
over 4 years ago
Nebulous Nail Issuesover 4 years ago
Legal Eagle: Website Slanderover 4 years ago
FDA Warns About Some JAK Inhibitorsover 4 years ago
Acne Care for Transgender Patientsover 4 years ago
Coding Office Visits: The 99211 Checklistover 4 years ago
Full Pipeline, Customized Diagnoses Expand Options for Rosaceaover 4 years ago
SRT Shows Positive Outcomes for NMSCNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.