- Dermatology Times, September 2021 (Vol. 42, No. 9)
- Volume 42
- Issue 9
FDA Warns About Some JAK Inhibitors
Although JAK inhibitors have shown efficacy in treating challenging conditions, federal regulators continue their safety reviews.
Mounting study data and results for off-label use show that Janus kinase (JAK) inhibitors could be highly effective treatments for various skin diseases and conditions. However, a trio of drugs recently received a setback with the FDA’s September 1 announcement that it will now require warnings about increased risk of serious heart-related events, blood clots, cancer, and death for skin disease treating JAK inhibitors.1
Progress in bringing pipeline JAK inhibitors to market for dermatological indications stalled earlier this year after a long-term, postmarketing study on tofacitinib (Xeljanz; Pfizer) in moderate to severe rheumatoid arthritis (RA)—required by the FDA for the first drug in the class to come to market— revealed apparently increased risks of tofacitinib compared to adalimumab in this specific patient population. Several JAK inhibitors have already been FDA approved outside dermatology.
Based on results of a large, randomized safety clinical trial, “...we have concluded there is an increased risk of serious heart-related events such as heart attack or stroke, cancer, blood clots, and death with the arthritis and ulcerative colitis medicines Xeljanz and Xeljanz XR (tofacitinib),” according to the FDA. “We are requiring new and updated warnings for 2 other arthritis medicines in the same drug class as Xeljanz, called Janus kinase (JAK) inhibitors, Olumiant (baricitinib) and Rinvoq (upadacitinib). Olumiant and Rinvoq have not been studied in trials similar to the large safety clinical trial with Xeljanz, so the risks have not been adequately evaluated. However, since they share mechanisms of action... FDA considers that these medicines may have similar risks as seen in the Xeljanz safety trial.”
These and other JAK inhibitors are in development for dermatologic (and other) diseases, said Brett Andrew King, MD, PhD, FAAD, associate professor of dermatology at Yale University School of Medicine, New Haven, Connecticut, in his presentations on JAK inhibitors at the 2021 American Academy of Dermatology Summer Meetings held April 23 to 25 (VMX) and August 5 to 8, 2021, in Tampa, Florida.2
“Despite the enormous steps that we have taken with biologics, most autoimmune and inflammatory skin diseases still do not have reliable, effective treatment. As such, there is a tremendous need for new therapeutics in dermatology and JAK inhibitors could fill the gap," Kind said.
Since the black box warning was issued to certain JAK inhibitors from the FDA, the regulatory agency has now approved JAK1/2 inhibitor ruxolitinib cream (Opzelura; Incyte) for the short-term and non-continuous chronic treatment of mild to moderate atopic dermatitis (AD) in non-immunocompromised patients 12 years of age and older whose disease is not adequately controlled with topical prescription therapies, or when those therapies are not advisable, according to a September 21
With physicians seeking a broader range of treatment options for AD, questions are being raised about whether the FDA is being overly cautious. “Overall, I’d say the FDA is understandably concerned. But the data show that some [JAK inhibitors] are more effective than the biologics that are approved, and they’re certainly much safer than systemic steroids that are approved for AD,” Mark G. Lebwohl, MD, told Dermatology Times® in an exclusive interview. He is dean for clinical therapeutics and a professor of dermatology at Mount Sinai Hospital in New York, New York, and a member of the Dermatology Times® editorial advisory board.
“If you put the black box warnings about the risk of thrombosis, malignancy, and infection in perspective, those risks are a fraction of what they are with cyclosporin, for example,” Lebwohl said. “In terms of systemic steroids, the AEs [adverse effects] dramatically exceed those of JAK inhibitors. So I understand why the FDA put this delay in [on approvals of 3 JAK inhibitors for atopic dermatitis]. My colleagues are concerned about it. It makes them worry more about the AEs. But all in all, there will be a very large number of patients for whom the benefit-risk ratio is worth it.” Another benefit is that the JAK inhibitors tend to be less immunosuppressive than some current treatment options, he said.
The outcome of the FDA’s assessment could have ripple effects across various skin diseases and conditions. “If you look at conditions such as alopecia areata [AA] and vitiligo, we don’t have good treatments for those conditions,” Lebwohl said. “Conditions like these have a high frequency of depression and suicide that dramatically affect the lives of patients in so many ways, and there’s nothing for them. So the JAK inhibitors are the first glimmer of hope for those patients in a very long time.” According to King, the emergence of JAK inhibitors could potentially be a treasure trove in dermatology for the treatment of AA, AD, dermatomyositis, granuloma annulare, sarcoidosis, lichen planus, morphea, pruritus, and vitiligo.
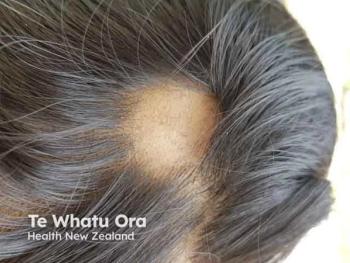
Recent top-line results of randomized clinical trials on use of JAK inhibitors to treat AA “offer hope of reliably effective treatment of this often devastating disease,” King said. In a dose-dependent manner, in 2 phase 2/3 trials (Brave-AA1 and Brave-AA2; NCT03570749 and NCT03899259, respectively), baricitinib demonstrated regrowth of scalp hair in up to 35% of patients treated with baricitinib, King said.3 In AD research, results of recent clinical trials4,5 show that 2 different JAK inhibitors, abrocitinib and upadacitinib, have comparable and, in some respects, increased efficacy to dupilumab (Dupixent; Sanofi and Regeneron Pharmaceuticals) over 12 to 24 weeks of treatment.
Increased selectivity in next-generation drugs’ mechanisms of action could lead to breakthroughs in psoriasis treatment as well, King added. Some, such as deucravacitinib (Bristol Myers Squibb), which inhibits TYK2, may be so selective that their ability to blockade certain cytokines but not others could decrease off-target or unwanted AEs, he said. “In psoriasis, results of deucravacitinib trials show for the first time that biologic-like efficacy in psoriasis is possible with an oral agent,” King said. “This is related to the fact that deucravacitinib modulates IL-23 signaling, which is known to be critically important in psoriasis pathogenesis. As such, deucravacitinib has the potential to be disruptive to the psoriasis treatment pyramid. But that hinges on the safety profile and label for deucravacitinib.”
Lebwohl added that deucravacitinib is so selective for TYK2 that it shows none of the AEs of the other JAK inhibitors. “This molecule is created in such a way that it pretty much only blocks TYK2. So, you’d expect it to be much more targeted, and therefore have fewer [AEs],” Lebwohl said. “I hope that this will gain approval. It is certainly more effective than apremilast. It’s much safer than cyclosporin and methotrexate. So, of the other drugs we have out there, this one would really help a lot of patients. Admittedly, you don’t know the full [AE] profile until the drug is on the market for years and thousands of patients use [it]. But of the oral drugs available, if approved, it would be the second new drug beyond the phosphodiesterase 4 [PDE4] inhibitor apremilast [Otezla; Amgen], which is very safe.”
In Lebwohl’s view, “the other diagnosis we’re not mentioning is psoriatic arthritis. We still have a very big void in the treatment of psoriatic arthritis. Upadacitinib recently published the data on the treatment of psoriatic arthritis, and their ACR [American College of Rheumatology] scores, which is a measure we use to determine severity of arthritis, were dramatically better than the current IL-17 and TNF [tumor necrosis factor] blockers that are the gold standard today for psoriatic arthritis,” he said. “They’re not good enough. Upadacitinib beat them. I think we’ll see similarly good results from other JAK inhibitors as well.”6
Despite the delays, Lebwohl is confident the JAK pipeline will not be shut down for long. “Everyone is anxiously awaiting these drugs,” he said. “We are gearing up for it. We’re getting ready for it. I personally had promised patients, ‘We’re going to have something better for you,’ because patients with psoriatic arthritis, AA, and vitiligo are badly underserved right now. I would be skeptical that we won’t begin to see FDA approvals. The current FDA cares about patients. They’ve shown that in many ways. I think that they are holding up approvals because they’re concerned about AEs. But I think that they have a realistic view and perspective on this. And I don’t think that [JAK inhibitors] won’t get approved. There may be boxed warnings... [about AEs], and those will have to be addressed. But in the end, we can put them in perspective for patients who are suffering with skin diseases and conditions.”
He pointed to similar concerns when biologics came to market. Surveys showed that physicians initially tended to overemphasize the AEs and underappreciate the beneficial effects of biologics. “Here we are years later, and biologics have taken over because they are very safe and effective. I do think the same will happen with JAK inhibitors,” Lebwohl said.
King added, “It is important for clinicians to have fluency in JAK inhibitors, their mechanism of action, their AE profile, and their amazingly broad potential across dermatological diseases, many of which lack reliably effective therapies. JAK inhibitors are going to make possible the treatment of many diseases that have been refractory to treatment.”
Disclosures:
King has served on advisory boards and/or is a consultant and/or is a clinical trial investigator for AbbVie, Aclaris Therapeutics, Almirall, AltruBio, Arena Pharmaceuticals, Bioniz Therapeutics, Bristol Myers Squibb, Concert Pharmaceuticals, Inc, Dermavant Sciences, Inc, Eli Lilly and Company, Incyte, LEO Pharma, Otsuka/Visterra Inc, Pfizer, Regeneron, Sanofi Genzyme, TWi Pharmaceuticals Inc, and Viela Bio, now owned by Horizon Therapeutics. He is on speaker bureaus for Pfizer, Regeneron, and Sanofi Genzyme.
Lebwohl is an employee of Mount Sinai and receives research funds from AbbVie, Amgen, Arcutis Biotherapeutics, Boehringer Ingelheim, Dermavant Sciences, Eli Lilly and Company, Incyte, Janssen, LEO Pharma, Ortho Dermatologics, Pfizer, and UCB, and is a consultant for Aditum Bio, Allergan, Almirall, Arcutis, Avotres, BirchBioMed, BMD skincare, Boehringer Ingelheim, Bristol Myers Squibb, Cara Therapeutics, Castle Biosciences, CorEvitas, Dermavant Sciences, EMD Serono, Evelo Biosciences, Facilitate International Dermatologic Education, Foundation for Research and Education in Dermatology, Inozyme Pharma, Kyowa Kirin, LEO Pharma, Meiji Seika Pharma, VYNE Therapeutics, Mitsubishi, NeuroDerm, Pfizer, Promius Pharma/Dr Reddy’s Laboratories, Theravance Biopharma, and Verrica Pharmaceuticals.
References:
- King BA. Treating alopecia areata and vitiligo with JAK inhibitors, a new frontier in dermatology. Presented at: 2021 American Academy of Dermatology Summer Meeting; August 5-8, 2021; Tampa, FL.
- King B, Ko J, Forman S, et al. Efficacy and safety of the oral Janus kinase inhibitor baricitinib in the treatment of adults with alopecia areata: phase 2 results from a randomized controlled study. J Am Acad Dermatol. Published online June 16, 2021. doi:10.1016/j.jaad.2021.05.050
- Bieber T, Simpson EL, Silverberg JI, et al; JADE COMPARE Investigators. Abrocitinib versus placebo or dupilumab for atopic dermatitis. N Engl J Med. 2021;384(12):1101-1112. doi:10.1056/NEJMoa2019380
- Blauvelt A, Teixeira HD, Simpson EL, et al. Efficacy and safety of upadacitinib vs dupilumab in adults with moderate-to-severe atopic dermatitis: a randomized clinical trial. JAMA Dermatol. Published online August 4, 2021. doi:10.1001/jamadermatol.2021.3023
- McInnes IB, Anderson JK, Magrey M, et al. Trial of upadacitinib and adalimumab for psoriatic arthritis. N Engl J Med. 2021;384(13):1227-1239. doi:10.1056/NEJMoa2022516
- FDA delays impacting inflammatory skin disease community. Dermatology Times. Published August 6, 2021. Accessed September 13, 2021. https://www.dermatologytimes.com/view/fda-delays-impacting-inflammatory-skin-disease-community
Articles in this issue
over 4 years ago
Nebulous Nail Issuesover 4 years ago
Legal Eagle: Website Slanderover 4 years ago
Acne Care for Transgender Patientsover 4 years ago
Coding Office Visits: The 99211 Checklistover 4 years ago
Full Pipeline, Customized Diagnoses Expand Options for Rosaceaover 4 years ago
Preventing Keloid Recurrence With SRTover 4 years ago
SRT Shows Positive Outcomes for NMSCNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.