- Dermatology Times, July 2022 (Vol. 43. No. 7)
- Volume 43
- Issue 7
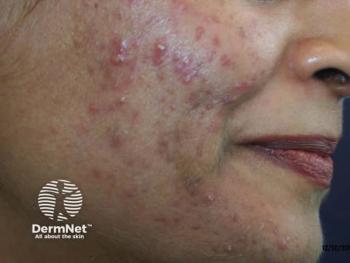
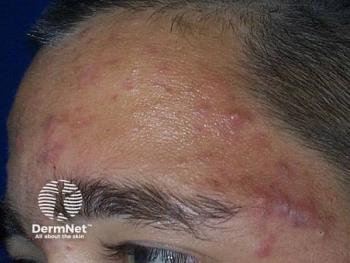
Study: Family History May Factor in Acne Presentation, Severity, and Scarring
Parental acne has “significant” associations with presentation and a predisposition to moderate to severe disease, but acne in siblings is a better indicator of the likelihood of grade 3 to 4 scarring, reported a recent study.
Although numerous epidemiology studies have investigated the risk factors associated with acne presentation and severity, few have examined acne scarring. New findings by a research team from the department of biological sciences at the National University of Singapore, set out to fill that information gap.1
“We initiated a study on the epidemiology of acne as this was a common skin condition afflicting young adults,” said Chew Fook Tim, associate professor in the department of biological services at National University of Singapore and lead author of the paper. “This study would form the baseline for us to understand the pattern of disease in our population and within our tropical environment and allow us to elucidate the underlying risk factors as well the pathogenesis, with the intent to evaluate modifiable factors that could be performed to alleviate the condition.”
This was not the first time that this research group investigated this subject. They undertook a highly detailed meta-analysis and critical review of the literature in this area.2
Their latest study aimed to investigate the prevalence of acne and its presentation, severity, and scarring grades and their associated risk factors among Singapore Chinese. They conducted a large-scale epidemiological study over multiple years, enrolling university students at the National University of Singapore. More than 4,000 individuals were evaluated both by investigator-administered questionnaires as well as physical observations.
“We evaluated the pattern of the disease, severity, as well as scarring due to the disease,” Chew said. “Additionally, we evaluated both lifestyle factors, such as diet and smoking, as well as demographic, socioeconomic, and personal health history.”
A total of 3,888 subjects (2,090 cases/1,798 controls; median age = 21 ± 4.589; range 17–71) completed an investigator-administered questionnaire as part of the cross-sectional study, which included sociodemographics, familial medical history, lifestyle factors, dietary habits, and acne history.
Investigators classified participants into five scarring grades based on the Qualitative Global Scarring Grading System (QGS), where grade 0 indicated no acne scars; grade 1, shallow scars not visable from a distance affecting less than one quarter of the face; grade 2, with slightly deeper scars that are slightly visible from a distance affecting more than one quarter but less than half of the face; grade 3, with even deeper scars visible from a distance affecting at least half of the face; and grade 4, with the deepest scars that are clearly visible from a distance affecting almost the entire face.
“One change made was to exclude erythema and hyperpigmentation marks from the grading system, which is in contrast with grade 1 of the QGS, which considered such marks,” Chew said.
“Further, unlike the QGS, the area of the face affected by scarring was considered in our grading system to ensure that fewer patients fell between 2 scarring grades.”
The research revealed the majority of the acne cases had mild acne/grade 1 scarring, while less than 1 percent had severe acne/grade 4 scarring.
“Parental acne was significantly associated with acne presentation and moderate/severe acne, while sibling acne was significantly associated with grade 3/4 scarring,” Chew added. “Gender and age affected acne severity and scarring but not acne presentation, while tertiary maternal education level and the possession of greater than or equal to 3 siblings were particularly associated with acne scarring.”
“Positive familial history is a strong predisposing factor in determining acne presentation, severity, and scarring,” Chew said. “The tendency to see familial history is not always an indication that genetics is at play. It could also be that families tend to have similar of shared environment(s) or shared lifestyles. Nevertheless, even after discounting for these other factors, genetic disposition still remained the strongest risk factor.”
The investigators found that having a body mass index that classified a patient as underweight was protective against acne presentation, while atopic diseases (asthma, allergic rhinitis, eczema) were its predisposing factors.
Lifestyle factors also play a role. “Of the evaluated lifestyle factors, computer/TV usage had significant association with acne presentation, while alcohol consumption was significantly associated with acne severity,” Chew said.
Diet is an additional consideration, wrote the authors. The paper showed that frequent milk consumption was associated with a protective effect for moderate to severe acne, while frequent butter consumption had a detrimental effect on the acne scarring extent.
Additionally, demographic factors and sedentary lifestyle influence acne presentation, while dietary habits influence acne severity and scarring. "The predisposing factors revealed in this study could help us to gain insights into acne pathophysiology and hence develop interventions especially targeting modifiable risk factors,” Chew said.
He noted that identifying the baseline patterns of disease was important so that the researchers could tease out what to work on first. With that done, they could then tackle the underlying pathogenesis one by one, including the genetics of the disease. That is what led to their next examination into the subject.
“We are currently focused on the modifiable factors such as diet first and are trying to understand the underlying factors that my influence the development of the condition due to these modifiable factors first,” Chew said. “In a follow-up study, we elucidated a potential mechanism linking frequent high glycemic index food intake to the disease and the potential link to what happens in the skin.”3
Chew believes the predisposing factors revealed in the study may help researchers and clinicians better understand the epidemiology of acne, especially in the Singapore population. In addition, the findings should guide future research on risk factors with the hope of better understanding the pathophysiology of acne and developing effective interventions especially targeting modifiable risk factors like lifestyle factors and dietary habits, the authors concluded.
Disclosure
The authors reported no relevant financial disclosures.
References
1. Heng AHS, Say YH, Sio YY, Ng YT, Chew FT. Epidemiological Risk Factors Associated with Acne Vulgaris Presentation, Severity, and Scarring in a Singapore Chinese Population: A Cross-Sectional Study. Dermatology. 2022;238(2):226-235. doi: 10.1159/000516232. Epub 2021 Jun 1. PMID: 34062533.
2. Heng AHS, Chew FT. Systematic review of the epidemiology of acne vulgaris. Sci Rep. 2020 Apr 1;10(1):5754. doi: 10.1038/s41598-020-62715-3. PMID: 32238884; PMCID: PMC7113252.
3. Say YH, Heng AHS, Reginald K, Wong YR, Teh KF, Rawanan Shah SM, Sio YY, Ng YT, Matta SA, Pang SL, Chew FT. Modifiable and non-modifiable epidemiological risk factors for acne, acne severity and acne scarring among Malaysian Chinese: a cross-sectional study. BMC Public Health. 2021 Mar 27;21(1):601. doi: 10.1186/s12889-021-10681-4. PMID: 33773591; PMCID: PMC8005239.
Articles in this issue
almost 4 years ago
Alopecia Areata Gets FDA-Approved Drugalmost 4 years ago
Optimize Acids, Peels in Acne Scar Treatmentalmost 4 years ago
What Practice Owners Need to Know When Considering a Sale or Mergeralmost 4 years ago
How Can I Be Sued for Not Having Access to Newer Mole Mapping Systems?almost 4 years ago
Trends in Clean, Sustainable, and Green Skin Care, Cosmeticsalmost 4 years ago
The Inside Look on the Dupilumab Approvalalmost 4 years ago
Factors Affecting Patients Adherence in Topical Therapiesalmost 4 years ago
Innovation in Psoriasis Therapies