- Dermatology Times, January 2023 (Vol. 44. No. 01)
- Volume 44
- Issue 01
Psoriatic Arthritis Mutilans
Arthritis mutilans, often called resorptive arthritis, is the most severe and rare form of psoriatic arthritis, affecting only about 5-16% of patients.
Arthritis mutilans (AM), often called resorptive arthritis, is the most severe and rare form of psoriatic arthritis, affecting only about 5-16% of patients.1 The condition is often called opera glass or chronic absorptive arthritis.1
AM is characterized by severe osteolysis of peripheral joints, often resulting in the shortening of digits and opera glass hand deformity. It primarily affects the joints of the hands and feet, causing severe functional impairment.2 It was previously believed that AM only affects hands, feet, toes or fingers. However, data shows that AM can affect any joint generally damaged by arthropathy.1
The Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) in 2012 described the disease's specific features. The features included digital telescoping and shortening, pencil-in-cup deformities, osteolysis, and involvement of distal interphalangeal joints and other small joints of the hands.3
Clinical Presentation:
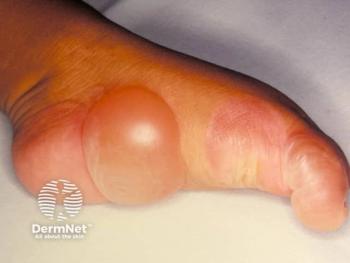
Patients with AM have telescopic fingers with bone edema and erosion severe enough that the hands appear like paws. The condition initially appears at the metacarpophalangeal and interphalangeal joints. The excess skin of the fingers folds tangentially, giving an opera-glass appearance. As the condition progress, it may lead to dislocation and resorption of the phalanges.1
On radiographic examination, patients with AM frequently exhibit deformities, including the pencil-in-cup deformity, where one end of the bone is worn down into the shape of a pencil tip, joint subluxation, and ankyloses. Evidence of comorbid conditions, including hypertension, dyslipidemia, metabolic syndromes, osteoporosis, and fragility fractures, have also been found among patients with AM.4
Causes:
AM mainly occurs in patients with pre-existing psoriatic arthritis or advanced rheumatoid arthritis. However, it can also occur independently.1 The exact cause of the condition is still unknown.
Joints with a high inflammatory burden are more likely to suffer further injury from mechanical stress.5 Studies have reported a link between HLA genes and an increased risk of AM. Moreover, Genetic markers like HLA-B27 and DQB1*02 have also been associated with AM.2
Management:
As soon as the disease is diagnosed, immediate treatment is required to prevent further erosion of the joints and subsequent loss of function. Osteoedema, in the short term, can show dramatic improvement when treated with TNF inhibitors.1 Immunosuppressive medications like methotrexate and leflunomide help reduce inflammation; a once-weekly dose of methotrexate at 10-25 mg has been found to be effective.1 Biologics including IL-17 and IL-23 inhibitors target inflammatory proteins, whereas JAK inhibitors are another class of drugs approved for treating the condition.6 A study published in the Journal of Drugs in Dermatology found significant improvements in the joints and skin of patients with AM after treating them with etanercept (Enbrel), a biologic TNF inhibitor. However, the treatment could not undo any pre-treatment damage or deformities experienced by the patients.7
AM can be successfully treated with iliac bone grafts and arthrodesis of the interphalangeal and metacarpophalangeal joints.1 Physical therapy is another option that may help reduce joint pain and inflammation with several different modalities, including ultraviolet (UV) treatment, ultrasound, cryotherapy, heat, electrical stimulation, and massage. Joints that are impaired by the disease can be supported using splinting.8
References
- Ishak AA, Al-Shamahy HA. Traveling Through Life with Arthritis Mutilans: Humanity Joins All Medical Practitioners in Treating and Supporting the Condition of Chronic Arthritis Mutilans Case. Ann Case Report. 2022;7:729. doi: 10.29011/2574-7754.100729
- Cordeiro RA, de Oliveira JL, Sampaio-Barros PD, Goldenstein-Schainberg C. Psoriatic arthritis mutilans: a descriptive study from a Brazilian tertiary center. Advances in Rheumatology. 2022;62(1). doi:10.1186/s42358-022-00245-4
- Chandran V, Gladman DD, Helliwell PS, Gudbjörnsson B. Arthritis mutilans: a report from the GRAPPA 2012 annual meeting. J Rheumatol. 2013 Aug;40(8):1419-22
- Rida MA, Chandran V. Challenges in the clinical diagnosis of psoriatic arthritis. Clinical Immunology. 2020;214:108390. doi:10.1016/j.clim.2020.108390
- Perrotta FM, Scriffignano S, De Socio A, Lubrano E. Occult axial involvement in patients with psoriatic arthritis mutilans: a case report. Reumatismo. 2019;71(2):88-91. doi:10.4081/reumatismo.2019.1146
- Sigurjonsdottir K, Jonsson H. A New Form of Arthritis Mutilans Related to Successful Gout Treatment. Journal of Arthritis. 2018;07(03). doi:10.4172/2167-7921.1000i107
- Samanta J, Chattopadhyay A, Sharma A. Psoriatic arthritis mutilans. QJM: An International Journal of Medicine. 2020;113(10):765-766. doi:10.1093/qjmed/hcaa029
- Afraz S. Consequences of Neglecting Rheumatoid Arthritis Treatment: A Case of Arthritis Mutilans in an Older Woman. Annals of Long-Term Care: Clinical Care and Aging. 2017;25(6):39-43. doi:10.25270/altc.2017.10.00012
Articles in this issue
about 3 years ago
Management of Generalized Pustular Psoriasisabout 3 years ago
Say No to Nasal Tanning Spraysabout 3 years ago
Nutritional Supplements to Treat Hair Lossabout 3 years ago
Exploring the Connection Between IBD and Psoriasisabout 3 years ago
Vitiligo Treatment and Managementabout 3 years ago
Study Finds JAK Inhibitors Safer Than Other Systemic Agentsabout 3 years ago
Dermatology Drug Pipeline 2023about 3 years ago
5 Simple Financial Tips for Dermatologists and Their Practicesabout 3 years ago
Nail Problems? Easy SolutionsNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.