- Dermatology Times, October 2020 (Vol. 41, No. 10)
- Volume 41
- Issue 10
Case series draws attention to phenotype of acne scarring
A retrospective review of patients seen in an academic dermatology clinic over a one-year period identified 20 individuals with nasal papules in association with acne, which are thought to represent scarring sequelae. The condition is underrecognized, researchers say and requires further research to better understand.
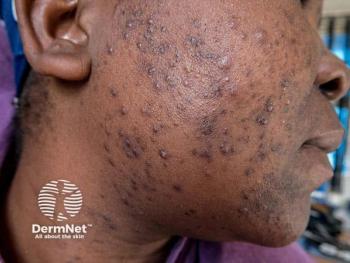
Papules occurring predominantly on the nose is an under-recognized form of acne scarring that seems to disproportionately affect younger males with skin of color, reported dermatology researchers from the New York University Grossman School of Medicine, New York, NY.
In an article published first online1, they reported the findings from a retrospective review that identified a series of 20 patients who presented with multiple papules on the nose in association with acne vulgaris.
Patients with nasal papules were identified through a review of electronic medical records between April 2018 and April 2019 by searching a photograph archives database using the terms “acne” and “nasal papules.” The patients who were identified included 17 males and three females. The median age of presentation was 16 years (range 12 to 30 years) and the mean age of acne onset was 14 years (range 11 to 20 years).
Nasal papules appeared concurrently or shortly after the development of acne. The majority of patients had moderate-to-severe acne and half were noted to have concurrent acne on the nose specifically. Five patients had papules on both the nose and chin. No patients had facial or extrafacial hypertrophic or keloidal scarring. Eight patients were noted to have atrophic acne scars on the cheeks.
Histopathologic examination of biopsies from five patients demonstrated dermal fibrosis and dilated thin-walled blood vessels, findings that the researchers noted were indistinguishable from those of conventional angiofibromas.
“It is not clear whether these lesions are true angiofibromas or a distinct entity with shared characteristics. Although acne has not been implicated in the development of angiofibromas, based on the data available for our patients, we do not believe that their lesions are a manifestation of any of the genetic conditions that are associated with multiple facial angiofibromas,” says Jorge Roman, M.D., lead author and dermatology resident.
Cutaneous stigmata of tuberous sclerosis were absent in all patients. None of the patients had a personal or family history of any genetic disorders.
Dr. Roman told Dermatology Times that he was motivated to undertake the review after seeing a patient with these nasal papules early during his training and finding a lack of information in the literature describing the condition. A literature search identified just two published reports of papular acne scarring.
Dr. Roman says, “Our study reports just a small series of patients that are affected by what we believe to be a much more prevalent problem. This condition is both under-recognized and under-reported. Having been raised in a predominately Latino community in Texas, I can easily recall seeing people with these papules growing up.”
All patients in the study were Fitzpatrick skin type III, IV, or V. In this cohort almost all of the cases were seen in adolescent Hispanic males. The cohort was comprised of 17 Hispanics, two African Americans, and one Asian patient. Information on patient ethnicity was absent in the previous reports of papular acne scars so the proclivity of this condition for this particular patient demographic was a novel finding.
Dr. Roman proposed that the paucity of reports describing the nasal papules might be related to healthcare disparities.
“Previous research has shown that racial minorities are lower utilizers of dermatologic care. It is possible that the patient demographic most afflicted by this condition face significant barriers when seeking care,” he tells Dermatology Times. “Given the dearth of information available on this condition, clinicians may not recognize it as an acne-related scarring process.”
In the published article, the authors stated that the nasal papules persisted despite conventional acne treatments such as topical antibiotics, oral antibiotics, and isotretinoin. Dr. Roman says. “Evaluation of different treatments for these papules is an area of ongoing investigation. Physical treatment modalities such as ablative laser or surgical removal seem to be the most efficacious.”
He and his coauthors hope to raise awareness of this entity in order to encourage further investigation and improve patient care.
“Early recognition and treatment can prevent the development or progression of these potentially disfiguring lesions,” Dr. Roman says.
References
1 Roman J, Krueger LD, Young TK, et al. The "bumpy" adolescent nose: Acne associated angiofibroma-like nasal papules. Pediatr Dermatol. 2020 Aug 7. [Epub ahead of print]. doi: 10.1111/pde.14319
Articles in this issue
over 5 years ago
Stem cell media boosts microneedling benefitsover 5 years ago
Cosmetic procedure complications in darker skinover 5 years ago
My experience with surface radiotherapyover 5 years ago
PDL, botulinumtoxinA improves rosacea symptomsover 5 years ago
Trial compares NMSC destructive techniquesover 5 years ago
Phenotype-based approach advances managementover 5 years ago
The retinoid revolutionover 5 years ago
Managing pandemic patient volumesover 5 years ago
I warned my patient – was it enough?Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.