- Dermatology Times, December 2019 (Vol. 40, No. 12)
- Volume 40
- Issue 12
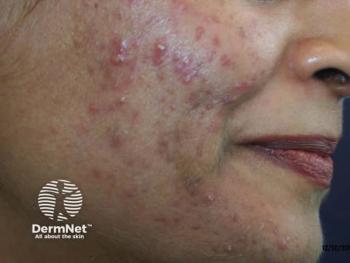
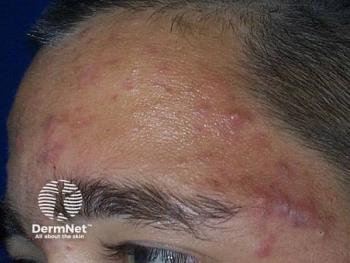
Acne patients open to antibiotic-free treatment
Acne patients are open to using effective antibiotic-free treatments if their prescriber offers them, says a recent study.
Most patients with acne and parents of children with the condition would be willing to try an effective antibiotic-free treatment for the condition, shows a study published in the Journal of Clinical and Aesthetic Dermatology.1
Dermatological conditions, particularly acne, are frequently treated with antibiotics. In fact, around 3–5% of all antibiotics prescribed across specialties in the US are prescribed in dermatology, two-thirds of these for acne vulgaris.
As efforts are made to limit the use of antibiotics to slow the growing threat of antimicrobial resistance, researchers conducted an online survey of patients and parents of children with acne to find out how much they know about antimicrobial resistance stewardship, and how accepting they would be of a non-antibiotic treatment.
The study found that the majority of patients and parents of young patients with acne vulgaris were aware of and concerned about the impact of antibiotic resistance. However, while they had a general understanding of the risks associated with antibiotic resistance and the possible causes, there were some gaps in knowledge, specifically regarding topical treatments.
“They underestimate the role of topical treatments in the development of antibiotic resistance,” says lead author James Del Rosso, M.D., JDR Dermatology Research/Thomas Dermatology in Las Vegas.
“Most of the respondents were not aware of antibiotic-free treatment options, but the vast majority were open to using an effective, antibiotic-free treatment for acne vulgaris on themselves or their children,” he adds.
A total of 809 adult patients aged between 17 to 40 years and 210 parents of children or adolescents aged 9 to 17 years who had received a prescription for an oral or topical treatment in the previous year were surveyed.
Of these, 86% correctly identified the definition of antibiotic resistance as when infectious organisms adapt and become immune to antibiotics and/or antibacterial use over a period of time, resulting in less effective treatment. Most respondents (84%) associated the use of oral antibiotics with developing antibiotic resistance, but fewer (62.1%) were aware of the role of topical antibiotics.
Awareness of antibiotic resistance, and the potential associated risks increased with the age of the responder. “It might be important to focus on increasing awareness among younger patients,” Dr. Del Rosso concludes.
Three quarters of survey respondents (74.2%) said that they would prefer to use or have their children use an effective antibiotic-free prescription treatment instead of a full-dose antibiotic, but few patients were aware of this option and fewer still had been offered it.
Only a third of respondents (35.3%) could recall their healthcare provider recently discussing the possible risks of antibiotic use as part of their acne treatment. In two thirds of cases (65.6%), these discussions had been initiated by their doctor.
Of those who could remember being prescribed an antibiotic in the last year or who were unsure, the figure was even lower; just 27.7% reported having discussed antibiotic-free acne vulgaris treatment options with their prescriber and only 31.7% (35.4% of adult patients, 16.2% of parents) were even aware of their existence.
When asked what role antibiotics played in the treatment of acne, 43.7% of respondents believed it was connected to their ability to treat bacteria or infection, and more than one third thought the condition was infectious or were unsure.
More than 90% of patients with acne and parents of children with acne responding to the survey believed that healthcare providers should do more to educate patients about antibiotics and antibiotic resistance.
“Nearly all respondents surveyed agreed that healthcare professionals should be involved in efforts to educate patients about antibiotic resistance, and respondents ranked actions by healthcare professionals as being the most effective,” Del Rosso says. “This indicates that there is an opportunity to improve the existing dialogue between clinicians, their staff, patients with acne vulgaris and parents of patients that are minors.
“Notably, the results of the survey indicated a need for improved patient knowledge regarding the specific risks of antibiotic resistance, particularly healthcare cost-associated risks, and knowledge of antibiotic-free treatment options.”
He adds, “Because the duration of antibiotic exposure is a critical factor in the propagation of antibiotic resistance, clinicians should be particularly mindful of educating patients with disorders that often require long-term treatment, such as acne vulgaris.”
References:
1. Del Rosso JQ, Rosen T, Palceski D, Rueda MJ. Patient Awareness of Antimicrobial Resistance and Antibiotic Use in Acne Vulgaris. J Clin Aesthet Dermatol. 2019;12(6):30-41.
Articles in this issue
over 6 years ago
Diet may impact squamous cell carcinoma riskover 6 years ago
Genetic expression testing still a work in progress for melanomaover 6 years ago
New resource for teens with atopic dermatitisover 6 years ago
When is the right time to retire?over 6 years ago
40 years of champions in dermatologyover 6 years ago
A novel target for rosacea treatmentover 6 years ago
Should dermatologists embrace AI?over 6 years ago
Spironolactone efficacy may be similar to oral antibiotic Tx