- Dermatology Times, October 2021 (Vol. 42. No. 10)
- Volume 42
- Issue 10
Rejuvenating Laser Leads to Acne Agminate-Like Reaction
A recent case report highlights the importance of caution when using fractional laser resurfacing in patients with active or previous acne.
A recent case report highlights the importance of caution when using fractional laser resurfacing in patients with active or previous acne, the report authors said. “We had a patient with mild comedonal acne who developed a severe acne agminate-like granulomatous reaction after rejuvenation laser therapy,”1 principal investigator Ifa Etesami, MD, MPH, told Dermatology Times®. She is an assistant professor in the Department of Dermatology at Razi Hospital, Tehran University of Medical Sciences, Iran. Along with carefully examining for acne in patients requesting laser rejuvenation, the authors recommend using deep bulk-heating rejuvenation lasers cautiously in the presence of acne lesions, or thoroughly treating the acne before laser therapy.
The case report was published online May 4 in the Journal of Cosmetic and Laser Therapy. To the best of the authors’ knowledge, theirs is the first report of such a reaction to minimally invasive fractional laser rejuvenation.
The 41-year-old woman underwent Fotona4D laser rejuvenation with the SP Dynamis dual-wavelength laser system (1064-nm Nd:YAG and 2940-nm Er:YAG; Fotona). At the time of treatment, she had mild inflammatory acne limited to her neck and chin. Her medical history was unremarkable except for adolescent acne, which was treated with isotretinoin for 8 months.
Perioperatively, the patient cleaned her face with a facial cleanser, after which the treatment area was cleaned with 70% ethanol solution. She underwent 1 laser session and began herpes prophylaxis immediately thereafter.
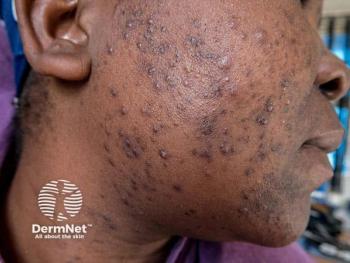
Three days postoperatively, the patient developed severe erythematous papules on her face and neck. One week post treatment, the lesions had evolved into monomorphic pustules. Tzanck smear ruled out the presence of herpes. Further investigation uncovered gram-positive cocci that culture revealed to be Staphylococcus epidermidis. This entity is rarely pathogenic, and authors considered it to be part of the patient’s normal skin flora.
The lesions did not respond to tetracyclines, cephalexin, or ciprofloxacin. After around 2 weeks, the lesions began to scale off and evolve into infiltrated edematous, erythematous papules.
Punch biopsy performed 3 weeks post laser showed ill-defined small granulomas—composed of histiocytes, small lymphocytes, and multinucleated giant cells without necrosis—in the superficial dermis. The infiltrate extended to the deep dermis and congregated around the follicles; the overlying epidermis showed mild acanthosis and spongiosis. Together, authors said, histological findings pointed to acne agminate. This condition usually affects young adults, with lesions occurring predominantly in the central face.
The patient experienced no systemic symptoms during the reaction. Laboratory tests including complete blood count, lipid profile, erythrocyte sedimentation rate, and renal and liver function were normal, as were viral markers, purified protein derivative/tuberculosis testing, and angiotensin-converting enzyme and calcium levels. Over time, the infiltrated papules resolved without therapy. By 2 months post treatment, the patient’s skin had completely recovered.
“Acne agminate is a relatively rare granulomatous condition with unknown etiology,” Etesami says. However, it may represent a form of granulomatous rosacea or a granulomatous reaction to ruptured hair follicles.2 Nishimoto et al showed that cell-mediated granulomatous immune reaction in acne agminate could occur following the entrance of Propionibacterium acnes into the dermis due to follicular rupture.3 Some authors have suggested that acne agminate is a granulomatous reaction to Demodex folliculorum, ruptured epidermal cysts, or aluminum zirconium complexes.4
Etesami said, “We believe that the bulk heating of the skin caused by the laser may have led to the rupture of existing comedones in our patient, leading to the entrance of Propionibacterium acnes and other particles of follicles into the dermis, resulting in a granulomatous reaction and acne agminate-like lesions.” Infections or biofilm may have aggravated the patient’s condition, she added, but the preoperative facial cleansing and negative culture from lesions argue against these possibilities.
The laser settings used were not particularly aggressive, said Etesami. “We believe that the Fotona 4D third step, which uses 1064-nm Nd:YAG with high fluences and high pulse duration (2 seconds), contributed most to the severe reaction in our patient.” The third step is performed to achieve deep and homogenous bulk heating of the skin, she said. However, Etesami added, performing this step in skin with existing comedones could have led to the rupture of the follicles and the subsequent severe granulomatous inflammation.
“Complications of resurfacing fractional lasers are rare, and these lasers are considered safe,” she said. “It’s also important to note that in our laser clinics at Razi Hospital, the Fotona 4D laser has been applied to hundreds of patients during recent years without any significant [adverse] effects [AEs].”
However, Etesami said, many studies report acneiform lesions as one of the most frequent AEs after laser therapy. In a study of 730 patients who underwent fractional rejuvenation with 1927-nm, 1550-nm, or CO2 laser, 13 patients experienced acne eruptions.5 In a retrospective study of 961 patients who underwent 1550-nm Er:YAG laser treatment, 7.6% experienced complications, with acneiform lesions (1.87%) being the most common.6 A review of all reported complications of fractional laser resurfacing occurring between 1998 and 2009 revealed that acneiform lesions occurred in 2% to 10% of patients.7 Conversely, authors uncovered only 1 previously reported case of granulomatous lesions occurring after laser resurfacing.8
Ultimately, authors advised caution in patients considering laser therapy who have active comedonal acne or a history thereof. “I would highly suggest dermatologists first treat comedonal acne lesions in patients seeking minimally invasive rejuvenation lasers before performing laser therapy,” Etesami said. “Even very mild comedonal acne, as in our patient, can lead to severe reactions including acne flare or the development of an acne agminate-like granulomatous reaction.”
References:
1. Balighi K, Abedini R, Ghanadan A, Peymanfar AA, Akhdar M, Etesami I. Self-limited acne agminate-like granulomatous reaction to facial laser rejuvenation in a patient with comedonal acne vulgaris. J Cosmet Laser Ther. 2020;22(6-8):241-243. doi:10.1080/14764172.2021.1921810
2. Ferguson L, Fearfield L. Topical dapsone gel is a new treatment option for acne agminata. Clin Exp Dermatol. 2019;44(4):453-455. doi:10.1111/ced.13742
3. Nishimoto J, Amano M, Setoyama M. The detection of Propionibacterium acnes signatures in granulomas of lupus miliaris disseminatus faciei. J Dermatol. 2015;42(4):418-421. doi:10.1111/1346-8138.12773
4. Ganzetti G, Giuliodori K, Campanati A, Simonetti O, Goteri G, Offidani AM. Doxycycline-isoniazid: a new therapeutic association for recalcitrant acne agminata. Dermatol Ther. 2012;25(2):207-209. doi:10.1111/j.1529-8019.2012.01442.x
5. Cohen SR, Goodacre A, Lim S, et al. Clinical outcomes and complications associated with fractional lasers: a review of 730 patients. Aesthetic Plast Surg. 2017;41(1):171-178. doi:10.1007/s00266-016-0767.x
6. Graber EM, Tanzi EL, Alster TS. Side effects and complications of fractional laser photothermolysis: experience with 961 treatments. Dermatol Surg. 2008;34(3):301-305; discussion 305-307. doi:10.1111/j.1524-4725.2007.34062.x
7. Metelitsa AI, Alster TS. Fractionated laser skin resurfacing treatment complications: a review. Dermatol Surg. 2010;36(3):299-306. doi:10.1111/j.1524-4725.2009.01434.x
8. Rendon-Pellerano MI, Lentini J, Eaglstein WE, Kirsner RS, Hanft K, Pardo RJ. Laser resurfacing: usual and unusual complications. Dermatol Surg. 1999;25(5):360-366; discussion 366-367. doi:10.1046/j.1524-4725.1999.07358.x
Disclosure:
Etesami reports no relevant financial disclosures.
Articles in this issue
over 4 years ago
Tap the Tax, Savings Potential of Cash Balance Plansover 4 years ago
Hair and Skin Diversity Examinedover 4 years ago
Rosacea Update: Facial Erythema’s Importanceover 4 years ago
Connecting Skin Diseases and COVID-19over 4 years ago
FDA Announces Action on Sunscreensover 4 years ago
New Frontiers Open for AD, Eczema Solutionsover 4 years ago
Pipeline Updates in Melanomaover 4 years ago
FDA Requiring Black Box Warning for Certain JAK InhibitorsNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.