- Dermatology Times, November 2022 (Vol. 43. No. 11)
- Volume 43
- Issue 11
Defining a New Era for Patients with PsO and PsA
At the 2022 Fall Clinical Dermatology Conference, Bruce E. Strober, MD, PhD, reviewed the best treatment options for patients with psoriasis and psoriatic arthritis.
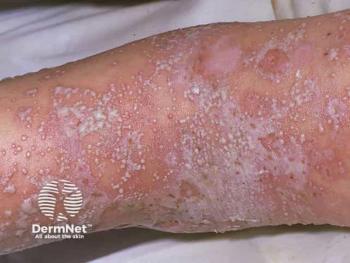
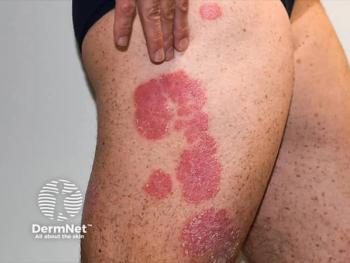
Bruce E. Strober, MD, PhD, clinical professor of dermatology at Yale University and scientific co-director of the CorEvitas Psoriasis Registry, presented his session, “Psoriatic Disease: Defining a New Era for Patients and Physicians,” at the 2022 Fall Clinical Dermatology Conference in Las Vegas, Nevada. The focus of his discussion was psoriasis and psoriatic arthritis, as well as the patient’s journey during treatments. Strober began by giving a quick review of psoriasis as a systemic inflammatory disease that is not just limited to the skin.
“Most patients have a lot of inflammation affecting other tissues, and that’s important because we need to control systemic inflammation for patients with psoriasis,” said Strober.
With psoriatic arthritis, the ligaments and tendons are affected just as much as the joints. Stiffness, pain, and achiness are other common symptoms of psoriatic arthritis. Another layer to consider is whether it’s peripheral or axial psoriatic arthritis. Axial diseases affect up to half of patients with psoriatic arthritis and are associated with neck and lower back pain.
Strober stated that one of the main goals of treating psoriasis or psoriatic arthritis is to achieve skin clearance. If dermatologists 100% clear a patient’s skin, it’s much easier to manage symptoms than if the patient is cleared only 80%-90%. Complete clearance also means that patients are more likely to benefit from no psoriasis symptoms and no impairment of their health-related quality of life.
Over 30% of patients with psoriasis will also develop psoriatic arthritis. Also for psoriasis patients, the time between the onset of psoriatic arthritis is 7-12 years, and the prevalence of psoriatic arthritis increases with psoriasis duration. As skin symptoms often precede psoriatic arthritis, dermatologists are in a unique position to identify and treat psoriatic arthritis earlier.
One of Strober’s most important takeaways from the session was that axial disease is an important consideration for people with psoriasis and psoriatic arthritis. Axial disease is present in 20%-50% of patients with psoriatic arthritis and may involve the spine, and it often goes undiagnosed.
“Axial disease affects the vertebra, specifically the neck, lower back, and the sacroiliac. It’s different than a disease that affects the periphery, such as the ankles. The reason why we know that is because certain therapeutics preferentially treat only a peripheral, but not an axial,” said Strober.
Moving on to therapeutic options, Strober believes that the current targeted therapeutics and targeted immunosuppressants on the market for psoriasis and psoriatic arthritis are safe and tolerable. He mentions that yes, dermatologists do know that some biologics aren’t meant for certain people. Patients would inflammatory bowel disease shouldn’t receive IL-17 inhibitors. Patients with certain forms of cancer should avoid JAK inhibitors. But the majority of patients with psoriatic disease have the ability to go on the different drug classes.
Rheumatologists strongly recommend IL-17 inhibitors and TNF inhibitors for patients with axial disease. IL-23s are not recommended for those with axial disease. Strober strongly emphasizes that if you have a patient with axial psoriatic arthritis, they need to go on an IL-17 or TNF inhibitor to effectively treat their symptoms and prevent severe progression.
Reference
Strober B. Psoriatic disease: Defining a new era for patients and physicians. 2022 Fall Clinical Dermatology Conference. October 21, 2022. Las Vegas, Nevada.
Articles in this issue
about 3 years ago
New Tech for Skinabout 3 years ago
Update on New Laser Treatments for Acneabout 3 years ago
Are You Prepared for Potential Tax Law Changes?about 3 years ago
Genetic Profiling and the Future of Therapeutics in Dermatologyabout 3 years ago
Low-Dose Oral Minoxidil for Hair Growthabout 3 years ago
The Role of Precision Medicine in the Management of Melanomaabout 3 years ago
The Latest Buzz in Atopic Dermatitisabout 3 years ago
Hand Healthabout 3 years ago
Hidradenitis Suppurativa: Current and Future TreatmentsNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.