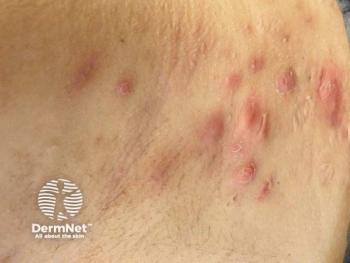
Cumulative dosing of isotretinoin should not follow strict range
Cumulative dosing of isotretinoin has followed a reference range of 120 to 150 mg/kg, but there is an absence of strong evidence supporting this recommendation, pointing to the need for clinicians to treat their patients to achieve clearance of acne rather than adhere to this range.
Clinicians should "ignore the numbers" when treating patients with acne and be guided by the principle to treat to clear, says Jerry Tan M.D., F.R.C.P.C., medical director at Windsor Clinical Research Inc. and an adjunct professor at Western University in London, Ontario, Canada.
Dr. Tan told colleagues during a session at Dermatology Update 2015 (Toronto) that the optimal dosing of oral isotretinoin, a drug that was introduced more than three decades ago, has long been debated in the dermatologic community internationally. Publications in the 1990s and various guidelines subsequently on management of acne put forth that cumulative dosing of isotretinoin should be in the range of 120 to 150 mg/kg to decrease recurrence of acne.
"This range of 120 to 150 mg/kg is probably incorrect," Dr. Tan says. "The issue is that we are over-treating patients with milder forms of severe acne and under-treating patients with severe acne. Slavish adherence to the outdated reference range means that we are treating to a number, not the patient." Dr. Tan and colleagues published results of a systematic literature analysis last year that challenged the dogma around the dosing of isotretinoin for acne.1 They contend that the basis for the recommendation is weak, with most of the studies that support the dosing range not being designed to address the issue.
A total of 20 studies were included in the systematic review. A total of four studies were graded as moderate quality to address remission with oral isotretinoin in acne, and the remainder low quality. Observational studies, for example, were regarded as low quality. Outcomes or endpoints to measure acne improvement varied across the studies. Seven studies, for instance, looked only at acne lesion counts, with some looking at only resolution of nodules and cysts and one looking only at inflammatory lesions.
In addition, the studies did not use standardized definitions of terms like relapse and remission, Dr. Tan stresses. "We would expect from the use of that terminology (remission) to mean absence of disease," he says. "(In these studies), relapse may be defined as severe, nodular acne to milder forms. The point of our paper is that prior studies variably define endpoints that may not reflect conventional medical vernacular - such as remission and relapse."
Patient expectations are such that they anticipate no longer having acne after being treated with oral isotretinoin, Dr. Tan says.
"When people wish to have acne treated, they don't want any acne (after treatment)," he says. "Remission should mean no acne and relapse should mean the recurrence of any acne, but that is not what the studies mean when they use such terms."
In the absence of restrictions on the daily dose of oral isotretinoin therapy, doses should be adjusted according to the patient tolerability, Dr. Tan notes. "It (daily dose) is targeted toward what is the best dose for the patient minimization of avoidable adverse effects and maximization of long-term outcomes," Dr. Tan says, noting daily doses may vary from 0.1 mg/kg to 1.0 mg/kg.
"My preference is for low daily doses - 0.1 to 0.25 mg/kg daily," he says. "They achieve excellent acne clearance and treatment is extremely well-tolerated with minimal dryness of skin and lips."
It is essential that clinicians discuss with their patients that the daily dose can be adjusted, for parents of many of the adolescent patients may have negative associations with oral isotretinoin in terms of its side effect profile. Beyond the usual concerns with use of oral isotretinoin, "parents may associate it (oral isotretinoin) with visible, disturbing side effects such as excessive dryness and chapping of their lips," he says.
Duration of therapy would be affected by the form of oral isotretinoin that is prescribed, Dr. Tan notes. "The more bioavailable the product, the lesser the duration of therapy required to achieve the same outcome," he says.
In terms of duration of therapy, Dr. Tan advises that clinicians treat at least one month after patients are clear of their acne. "We are seeing patients no more frequently than once per month," Dr. Tan says. "I typically treat for one additional month once a patient has achieved acne clearance, meaning absence of primary acne lesions especially inflammatory ones (multiple and/or deep comedones may require adjunctive therapy). There is no current evidence to support prolongation of therapy beyond that time. That trial is waiting to be done to evaluate effect on recurrence."
Disclosure: Dr. Tan has been an advisor, consultant, clinical trialist and/or speaker for Cipher and Roche.
Reference:
1 Tan J, Knezevic S, Boyal S, Waterman B, Janik T. Evaluation of Evidence for Acne Remission With Oral Isotretinoin Cumulative Dosing of 120-150 mg/kg. J Cutan Med Surg. 2015 Jul 17.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.