- Dermatology Times, September 2020 (Vol. 41, No. 9)
- Volume 41
- Issue 9
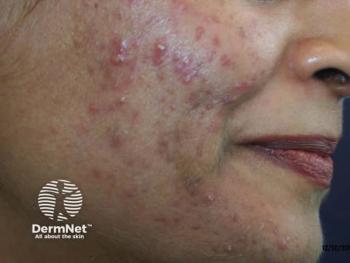
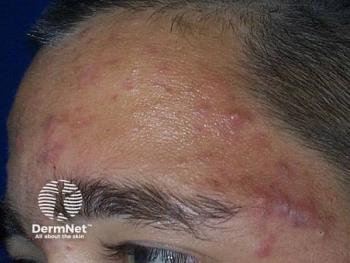
Combination therapies improve keloid treatment
Combination therapies that integrate older therapies have shown great promise in the treatment and management of keloids.
Although there is no wide consensus as to which combination therapies work best for keloid lesions, many specialists around the world are independently using and experimenting with combinations of older and newer treatment modalities, many of which are proving to be very effective, an expert says.
“Keloids are challenging to treat and as such, many clinicians will typically combine a number of different treatments and delivery modalities in order to help achieve optimal clinical outcomes. However, currently, there is no agreement as to which are the most effective combination treatments for keloids and which combination therapy might work better for keloids of a different anatomical location,” says David M. Ozog, M.D., FAAD, chair, department of dermatology, C.S. Livingood Chair in Dermatology, director of cosmetic dermatology, division of Mohs and dermatological surgery, Henry Ford Hospital, Detroit.
The treatment of keloids has always been complex and includes a wide spectrum of therapies ranging from more traditional surgical procedures to intralesional or topical agents, radiation, botulinum toxin and energy-based devices. Though many of these therapies can work well in keloid treatment as stand-alone therapies, it is the clever combinations of these treatment approaches and how they are optimally delivered that has been somewhat revolutionary in keloid therapy of late, Dr. Ozog says.
RELATED:
In his keloid patients, Dr. Ozog usually treats the lesion with either a combination of pulsed dye laser (injection) or fractional ablative laser (topical) prior to the application corticosteroids or 5-fluorouracil (5-FU), allowing the medication to reach much deeper and more consistently into the keloid.
In recalcitrant lesions, Dr. Ozog may perform a traditional surgical excision followed by the application of varying combination therapies including laser, the injection of steroids and/or 5-FU, and/or radiation treatment to the target area.
For painful keloids and particularly those located on the trunk, Dr. Ozog found that pretreating these lesions with pulsed dye or CO2 laser enables a quicker and more efficient delivery of steroid or 5-FU drugs due to the tissue edema created.
Other leading specialists around the world are also currently using similar combination treatments, Dr. Ozog says, and achieving similar positive clinical outcomes. Matteo Clementoni, M.D., Milan, Italy, has achieved remarkable clinical results using a CO2 laser followed by a combination of botulinum toxin, steroids, and 5-FU applied topically on the skin, Dr. Ozog says. The delivery of the topical drugs to the keloid is far more effective and quicker through the micro-channels created by the CO2 laser, he says.
“The positive response to these new and experimental keloid therapies independently performed by specialists around the world is testament to their efficacy and reinforces their place in keloid therapy,” Dr. Ozog says.
Another interesting treatment approach pioneered by Somesh Gupta, M.D., New Delhi, India, combines RF energy with the delivery of steroids and 5-FU at the same time.1 According to Dr. Ozog, the novel treatment using insulated probes protects the outer keloidal skin from the heat produced by the RF device, helping to prevent any unwanted pigmentary changes, and allows the clinician to deliver the RF waves to the core of the lesion while simultaneously incrementally delivering the drugs chosen for treatment.
“For ear keloids, surgery followed by some other treatment such as steroids or 5-FU is still commonly employed. However, for truncal lesions where recurrence rates are high, there is a definite trend towards combination approaches that incorporate energy-based modalities such as laser and RF,” Dr. Ozog says.
One of the newer developments in keloid research revealed in a recent study2 by Ardeshir Bayat, M.D., from the University of Manchester, UK, was that hypertrophic scars and keloidal scars are very different and that there are specific biomarkers that can help clinicians differentiate between them.
According to Dr. Ozog, there are distinct molecular differences between keloids of different anatomical locations and these lesions behave differently in the same patient depending on the location they occur.
“Many specialists from all around the world are currently using combinations of energy-based devices and medications whether they are cytotoxic, steroids, or even botulinum toxin. New and exciting combinations of treatments combined with clever drug delivery modalities is what is making the difference and allowing us to achieve exceptional clinical outcomes,” Dr. Ozog says.
Disclosure:
Dr. Ozog reports no relevant disclosures.
References:
1 Yadav S, Gupta S. A simple device for ablation of keloidal tissue and serial deposition of intralesional drugs. J Am Acad Dermatol. 2018 May;78(5):e107-e109.
2 Bagabir RA, Syed F, Sheniere P, Paus R, Bayat A. Identification of a potential molecular diagnostic biomarker in keloid disease: syndecan-1(CD138) is overexpressed in keloid scar tissue. J Invest Dermatol. 2016 Nov;136(11):2319-2323.
Articles in this issue
almost 6 years ago
Will OSHA cite me for requesting employees not wear masks?almost 6 years ago
How safe are cosmetics?almost 6 years ago
Pretreatment punch technique guides safe injectionalmost 6 years ago
COVID-19 safety guidelines provide protocols to protect staff, patientsalmost 6 years ago
What we know (and don’t) about dietary effects on skin agingalmost 6 years ago
Microbiome-based treatments not ready for prime timealmost 6 years ago
Emerging options for high-risk melanomaalmost 6 years ago
Systemic immunomodulatory therapy may protect patients with COVID-19almost 6 years ago
Phenotypes inform management optionsalmost 6 years ago
AI has potential to improve melanoma detection