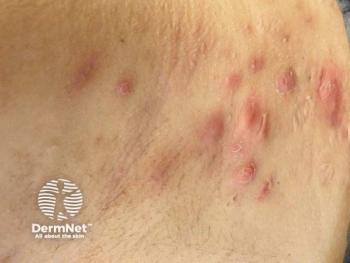
Caffeine can reduce inflammation in patients with eczema and psoriasis
Adding caffeine to topical skin treatments would be a simple way to reduce inflammation in patients with atopic dermatitis and psoriasis, suggests a review presented at the Psoriasis: From Gene to Clinic International Congress, which took place in London this week.
LONDON - Adding caffeine to topical skin treatments would be a simple way to reduce inflammation in patients with atopic dermatitis and psoriasis, suggests a review presented at the Psoriasis: From Gene to Clinic International Congress, which took place in London this week.
The researchers identified past studies which had investigated the effects of topical caffeine in atopic dermatitis or psoriasis, the results of which have all but been forgotten, and looked for potential mechanisms for caffeine’s positive effects.
One of the researchers, Mais Alashqar, M.D., of Alfaisal University in Riyadh, Saudi Arabia, said: “Initial studies in the 1970s first demonstrated this, but 40 years later this knowledge has, in a sense, faded. We still don’t add caffeine to topical steroids that patients use daily. It is a simple step that could significantly benefit the many patients around the world that suffer from inflammatory skin conditions like eczema or psoriasis. We hope that our review will help bring this knowledge back into the consciousness of doctors and patients.”
The review found that in the 1970s a research group conducted several studies on caffeine in patients with atopic dermatitis, culminating in a double-blind study involving 83 patients in which topically applied caffeine 30%-hydrocortisone 0.5% in hydrophilic ointment was compared to betamethasone valerate 0.1% cream and hydrocortisone 0.5% in hydrophilic ointment. After three weeks’ treatment the betamethasone and caffeine-hydrocortisone groups performed significantly better than the hydrocortisone group on three of seven scales assessed - lichenification, excoriation, and global impression – and outcomes in the betamethasone group did not differ significantly from the hydrocortisone group.1
A more recent study of 39 patients with stable plaque psoriasis showed that application of 10% caffeine produced significantly greater improvement in Psoriatic Area and Severity Index (PASI) scores than placebo. The only side effect of caffeine appeared to be mild itching.2
Patients with atopic dermatitis and psoriasis have decreased intracellular cAMP levels in cutaneous leucocytes, and the reviewers propose that caffeine, being a methylxanthine and hence a phosphodiesterase inhibitor, raises intracellular cAMP levels, which suppresses inflammatory pathways.
The researchers added that caffeine also has proapoptotic and anti-necrotic properties so may reduce inflammation by influencing cell death pathways. As an ATR (ataxia-telangiectasia mutated) kinase inhibitor and an ATM (ATM- and Rad3-related) kinase inhibitor, caffeine promotes prompt apoptosis (programmed cell death) of damaged cells. Caffeine also exhibits anti-necrotic effects which prevent cells damaged by oxidative stress from dying prematurely through necrosis, a process which can lead to further inflammation. Several caffeine metabolites also have anti-oxidising effects which may further reduce inflammation.
Primary treatments such as corticosteroids for atopic dermatitis and psoriasis are associated with side effects, Dr. Alashqar said. “Caffeine is a cheaper, safer alternative that could complement the long-term therapy of atopic dermatitis and psoriasis patients,” she said. “More research is needed to fully elucidate its potential.”
REFERENCES
1. Kaplan RJ, Daman L, Rosenberg EW, Feigenbaum S. Topical use of caffeine with hydrocortisone in the treatment of atopic dermatitis. Arch Dermatol. 1978 Jan;114(1):60-2.
2. Vali A1, Asilian A, Khalesi E, Khoddami L, Shahtalebi M, Mohammady M. Evaluation of the efficacy of topical caffeine in the treatment of psoriasis vulgaris. J Dermatolog Treat. 2005;16(4):234-7.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.