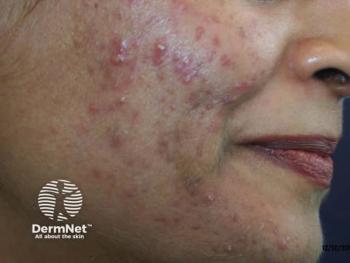
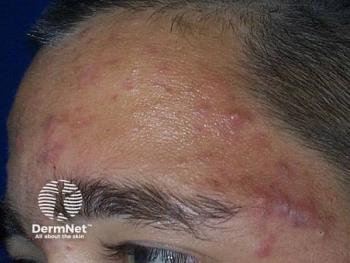
Asynchronous Telemedicine for Isotretinoin Management
A research letter to the editor published in the Journal of the American Academy of Dermatology examines how synchronous telemedicine may be limiting the telemedicine capabilities of the dermatology profession and how asynchronous telemedicine may be the answer.
A research letter1 in the
The researchers write that, “ST requires provider-patient co-availability and fails to address the capacity constraints of our specialty.” In comparison, AT may enhance access4,5 by allowing more routine care to be delivered in a scalable fashion, the researchers continued. The aim is to see if AT can free in-person and AT appointments for more urgent dermatologic care.
The researchers piloted a direct-care AT program for isotretinoin management in established acne patients at their urban, academic dermatology clinic. The patients were instructed to upload photographs then complete an online questionnaire through a non- electronic medical record (EMR)-based web portal accessible on any internet-enabled device. After, the physician used the same access portal to respond asynchronously, and the final AT note is ported into the EMR.
The researchers acknowledged that there are physicians that may hesitate to adjust isotretinoin dosing without a synchronous visit, but they hypothesized that in practice, there would be no difference in dosing outcomes between AT and ST groups. There were 126 patients between March 1, 2020 to May 7, 2020 that completed 182 isotretinoin AT visits that were then retrospectively compared with ST from the same period.
“We developed the AT program pre-pandemic to offset access constraints to our clinic and targeted isotretinoin patients because they require frequent office visits,” the researchers stated. “The pandemic prompted us to rapidly enroll many isotretinoin patients into AT during clinic closures.”
More than three-fourths of isotretinoin AT visits (77.5%) were completed successfully without conversion to ST visits.
The clinician behavior was investigated by using dose adjustments as a proxy for clinician comfort with asynchronous care delivery, the article explained. Isotretinoin AT visits were comprised of the full spectrum of therapy from start to finish, and dosing outcomes were not different between AT and ST groups. Importantly, dosing outcomes were also not different between AT-only and AT-converted-to-ST groups, meaning these conversions were not prompted by dosing adjustments.1
The data when compared to each other may suggest that dermatologists were comfortable remotely adjusting isotretinoin dosing (both escalating for therapeutic effect and decreasing to manage side effects) without a synchronous encounter.
Another benefit of the isotretinoin AT program was alignment of screening pregnancy test with the clinical encounter.
The researchers AT program was funded internally without insurance billing, and which may be the greatest barrier to broader utilization.6 However, the trend in telemedicine reimbursement may eventually allow coverage for AT encounters that replace office visits, the researchers explained.
“Further studies of the asynchronous care model will inform utility of AT for routine follow-up and even triage across a spectrum of conditions,” the authors concluded. “We urge our colleagues to continue practicing teledermatology and consider incorporating AT to improve patient access and clinical productivity. These efforts will keep our specialty poised at the leading edge of health care delivery.”
Reference:
- Das S, Su MY, Kvedar JC, Smith GP. Asynchronous telemedicine for isotretinoin management: A direct care pilot. Journal of the American Academy of Dermatology. 2022;86(1):184-186. doi:10.1016/j.jaad.2021.01.039
- Hollander JE, Carr BG. Virtually perfect? Telemedicine for covid-19. New England Journal of Medicine. 2020;382(18):1679-1681. doi:10.1056/NEJMp2003539
- Lee I, Kovarik C, Tejasvi T, Pizarro M, Lipoff JB. Telehealth: Helping your patients and practice survive and thrive during the COVID-19 crisis with rapid quality implementation. J Am Acad Dermatol. 2020;82(5):1213-1214. doi:10.1016/j.jaad.2020.03.052
- Seiger K, Hawryluk EB, Kroshinsky D, Kvedar JC, Das S. Pediatric dermatology eConsults: Reduced wait times and dermatology office visits. Pediatric Dermatology. 2020;37(5):804-810. doi:10.1111/pde.14187
- Improved patient access and outcomes with the integration of an eConsult program (Teledermatology) within a large academic medical center. Journal of the American Academy of Dermatology. 2020;83(6):1633-1638. doi:10.1016/j.jaad.2019.10.053
- Osman MA, Schick-Makaroff K, Thompson S, et al. Barriers and facilitators for implementation of electronic consultations (Econsult) to enhance access to specialist care: a scoping review. BMJ Global Health. 2019;4(5):e001629. doi:10.1136/bmjgh-2019-001629