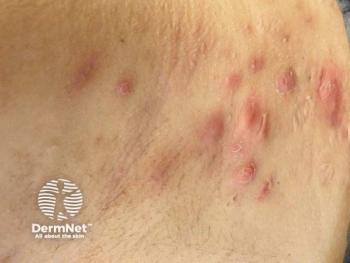
Anticipated FDA Approval of Bimekizumab for HS: Insights From Investigator Christopher Sayed, MD
The phase 3 studies, BE HEARD I and BE HEARD II, showed significant improvements in skin pain over the 48-week period.
UCB has released data a 48-week post-hoc analysis of pooled phase 3 data, showcasing the potential of bimekizumab (Bimzelx) in treating moderate to severe hidradenitis suppurativa (HS). The company presented14 bimekizumab abstracts across a range of disease states including HS, plaque psoriasis, and psoriatic arthritis during the 2024 American Academy of Dermatology (AAD) Annual Meeting in San Diego, California. UCB expects FDA action and potential approvals for all indications by the end of 2024.1
Christopher Sayed, MD, dermatologist at the University of North Carolina Chapel Hill’s HS clinic, served as an investigator for the phase 3 studies, BE HEARD I (
Patients with HS under bimekizumab treatment exhibited improvements in skin pain over the 48-week period, as assessed through various outcomes such as the HS Symptom Questionnaire (HSSQ) skin pain item, Patient Global Impression of Severity of Skin Pain (PGI-S-SP), and Change in Severity of Skin Pain (PGI-C-SP). Furthermore, patients demonstrated more substantial reductions in draining tunnel count compared to those on placebo at week 16, with these positive responses persisting or improving up to week 48.
Hadar Lev-Tov, MD, associate professor at the University of Miami in Miami, Florida, expressed his optimism about the long-term results in a UCB press release. He noted that after 48 weeks of bimekizumab treatment, approximately 6out of 10 patients reported their skin pain as "much better." These results hold particular significance, given the common complaint of pain in individuals with HS that dermatologists confront daily.
It's crucial to acknowledge that while these findings are promising, bimekizumab is not currently approved for the treatment of moderate to severe HS by any regulatory authority worldwide. The efficacy and safety profile for this indication is still under investigation.
The phase 3 studies, BE HEARD I and BE HEARD II, included 1014 adult patients with moderate to severe HS. They were randomized into different treatment groups, receiving bimekizumab at various intervals or a placebo. The baseline characteristics, including a mean HSSQ skin pain score of 5.8, underscored the initial pain levels experienced by the participants.2
Key highlights from the bimekizumab data presented at AAD 2024 include significant impacts on pain:
- At week 48, 64.6–75.7 percent of patients achieved an HSSQ skin pain response.
- HSSQ skin pain score of 0 at week 48 was achieved by 12.7–19.8 percent of patients.
- From weeks 0–48, HSSQ skin pain scores reduced by 36.9–43.7 percent across treatment groups.
- At week 48, 55.9–63.7 percent of patients rated their skin pain as "much better" using PGI-C-SP.
- At week 48, the percentage of patients rating PGI-S-SP as "severe" decreased to 3.9–7.8 percent, compared to 28.5-33.3 percent at baseline.
The impact on draining tunnel count was also noted:
- At week 16, bimekizumab-treated patients demonstrated a higher draining tunnel percent change from baseline compared to placebo (-43.9 to -45.7 vs. -21.5 percent).
- Absolute changes in draining tunnel count were greater in bimekizumab-treated patients compared to placebo.
- The percentage and absolute change from baseline increased through week 48 across all bimekizumab groups.
- At week 16, a greater proportion of bimekizumab-treated patients experienced draining tunnel reductions of 3 or more compared to those on placebo (58.0–70.6 vs. 35.0 percent), with sustained or improved responses to Week 48 across regimens (79.4–88.7 percent).
Sayedacknowledged the exciting advancements in HS therapies over the past decade saying “It is really exciting to see so much data come out for so many different drugs. Adalimumab (Humira) got approved almost 10 years ago at this point. Secukinumab(Cosentyx) was the next to get approved for several years. What I'm most looking forward to is the is the fact that at least some of these drugs, bimekizumab being one of them, is going to be a step up in terms of level of response. I think it'sgoing to be reassuring that more patients respond. And when they do respond, they respond more deeply. And they hopefully maintain those responses over longer periods of time. And it'sgoing to get more and more confusing as more drugs do come to market to figure out which drug is best for each patient. Hopefully, we get better at understanding that and predicting response to treatments, that we're not just cycling patients through a whole bunch of medications back-to-back. I think it's going to be nice to see this next step of an evolution where again, patients can expect a bit more.”3
Speaking on the safety profile of bimekizumab, Sayed reassured that dermatologists are already familiar with IL-17 inhibitors, and the study results were consistent. "Thrush is something that is occasionally seen, but pretty much no patient with HS is ever going to say they're getting a lot better on a drug like that and that thrush matters to them at all. They'd much rather treat that as a very mild inconvenience and very easy for us to treat as physicians. So, patients in the study pretty much always continued, regardless of something like that,” Sayed explained.
The trial investigator concluded that he is optimistic about bimekizumab getting approved by the FDA for the treatment of HS and expressed how it would drastically improve the quality of life for patients. “HS is a disease with lots of ups and downs. Having stable improvement tells you that the drug [bimekizumab] is really working. They didn't just happen to get better on the day they were measured at the week 16 time point.They're clearly moving the right direction very steadily over time for patients,” Sayed concluded.“You know, part of the trouble that comes along with HS is the unpredictability, the fact that it can flare up anytime at all like you have a vacation plan when you have some big family event planned. So the idea that you can be stable over a long period of time and have fewer ups and downs means sort of less dread hanging over that patient all the time.”
References
- BimzelxI® 48-week phase 3 analyses in moderate-to-severe hidradenitis suppurativa showed sustained improvements in skin pain and draining tunnel count. News release. UCB. March 8, 2024. Accessed March 9, 2024.
https://www.ucb-usa.com/stories-media/UCB-U-S-News/detail/article/bimzelx-48-week-phase-3-analyses-in-moderate-to-severe-hidradenitis-suppurativa-showed-sustained-improvements-in-skin-pain-and-draining-tunnel-count - Glatt S, Jemec GBE, Forman S, Sayed C, et al. Efficacy and safety of bimekizumab in moderate to severe hidradenitis suppurativa: a phase 2, double-blind, placebo-controlled randomized clinical trial. JAMA Dermatol. 2021 Nov 1;157(11):1279-1288. doi: 10.1001/jamadermatol.2021.2905. Erratum in: JAMA Dermatol. 2021 Nov 1;157(11):1384. PMID: 34406364; PMCID: PMC8374742.
- Fragoso NM, Masson R, Gillenwater TJ, Shi VY, Hsiao JL. Emerging treatments and the clinical trial landscape for hidradenitis suppurativa part I: topical and systemic medical therapies. Dermatol Ther (Heidelb). 2023;13(8):1661-1697. doi:10.1007/s13555-023-00956-6
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.