Understanding Hidradenitis Suppurativa Subtypes
Ginette A. Okoye, MD, FAAD, provides several clinical pearls to help physicians find the best therapy for their individual hidradenitis suppurativa patients in her presentation at the Skin of Color Update 2021.
Physicians should be asking themselves 3 questions to determine how to best treat their individual hidradenitis suppurativa (HS) patients, according to Ginette A. Okoye, MD, FAAD, professor and chair of the department of dermatology at Howard University College of Medicine, Washington, D.C., and co-chair of the scientific committee of the Skin of Color Society, who presented at the Skin of Color Update 2021, held virtually September 10-12.
These 3 essential questions include:
- Why type of HS does the patient have?
- Has the patient identified any triggers for development of new lesions or flares?
- Which comorbidities does the patient have or is at risk for?
According to Okoye’s observations and knowledge of available research, she suggested several clinical pearls based on these questions to help physicians navigate which therapy is best for their HS patients.
In her presentation, Okoye emphasized the importance of knowing the specific type of HS that patients have to better understand the pathogenesis of the disease and its subsequent treatment.
She identified 4 clinical subtypes of HS including axillary-mammary-inguinal, follicular, gluteal, and syndromic.
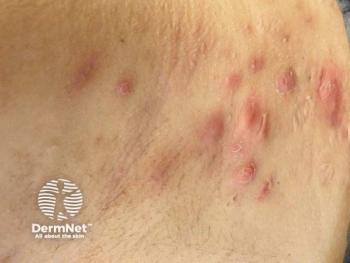
Axillary-mammary-inguinal HS
For the subtype axillary-mammary-inguinal HS, Okoye has observed that lesions appear most commonly on the breasts, in the underarms, and the in inguinal fold. Also, this subtype of HS patients tends to be predominately female.
“These patients tend to report hormonal fluctuations with the severity of their HS, and these are the patients might respond to weight loss. Certainly, obesity is not the cause of HS, so you have to be careful when you approach this topic with your patients,” Okoye said.
The pathogenesis for this subtype, according to Okoye, includes diet, obesity, and hormonal influences. Because of these factors, her recommended treatments in addition to anti-inflammatory therapy involves spironolactone 50-200 mg daily, metformin 2000 mg daily, laser hair removal, as well as in some circumstances the use of oral contraceptive pills that are FDA-approved for acne. Okoye also suggests discouraging the use of progesterone-only hormone contraceptives and talk with your HS patient about nutrition support and dietary modifications.
“What I tell [patients] is based on the little bit of data we have and based on what patients have told me over the years, I believe, a low carbohydrate diet, or a lower glycemic index diet might be helpful. Even if it's not helpful for their HS, it may be helpful for their comorbidities,” Okoye said.
Follicular HS
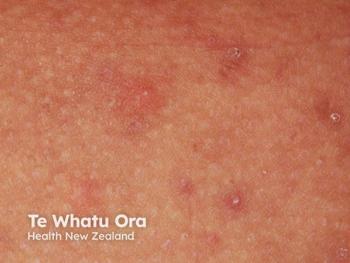
For the follicular subtype of HS, Okoye said these patients have HS in the typical locations, but the lesions tend to be smaller and less severe. However, they also have other types of lesions such as open comedones, epidermal cysts, pilonidal cysts, and severe acne.
“The other thing about these patients is they can get HS in what we would call atypical areas like the lateral thigh, the chest, the back, but those lesions are smaller and very follicular centric compared to your typical HS lesion,” Okoye said.
This subtype consists of a mostly males, and can affect current and former smokers, according to Okoye’s observations. She added that the follicular subtype has moderate disease severity, but also includes earlier disease onset, as well as a longer disease duration.
For the pathogenesis of this subtype, Okoye believes impaired notch signaling caused by gamma secretase mutation or smoking. “I think the people with the more severe phenotype have both that mutation and they're smokers,” Okoye said.
When it comes to treatment, Okoye’s preferred therapies include oral and topical retinoids such as isotretinoin and acitretin in lieu of anti-inflammatory therapy. Also, early surgical excision of epidermal inclusion cysts (EICs) can be removed in cosmetically sensitive areas, but Okoye says to leave the other EICs alone unless they are symptomatic. Most importantly, she recommends these types of HS patients to quit smoking.
Syndromic HS
This HS subtype, according to Okoye, consists of patients with follicular occlusion tetrad and auto-inflammatory syndromes such as:
- PAPASH (pyogenic arthritis, pyoderma gangrenosum, acne, HS)
- PASH (pyogenic arthritis, HS)
- HS and inflammatory arthritis
- SAPHO syndrome (synovitis, acne, pustulosis, hyperostosis, osteitis)
Okoye believes neutrophil, interleukin (IL)-17, IL-1, and tumor necrosis factor (TNF)-α are associated with the pathogenesis of syndromic HS patients.
“Now these patients, I think, are squarely in the inflammatory camp. And so, for them, biologics are my go-to,” Okoye said.
Her preferred biologics include adalimumab, ustekinumab, guselkumab (for ulcerative HS), secukinumab (for HS and inflammatory arthritis), and anakinra. She also mentioned her use of prednisone in a high dose (80 mg daily) with a prolonged slow taper for acute control while starting the biologic, or as maintenance therapy with 20 mg once a week or 20-40 mg once at the beginning of a flare.
“This is very similar to how you would treat a patient with pyoderma gangrenosum (PG), so I kind of justify it to myself that these are people who I am trying to keep out of the hospital,” Okoye said. “They are walking around with 10-cm ulcers. So, I use high-dose prednisone, with a long, slow taper similar to what you would do for PG.”
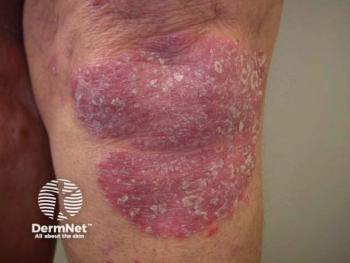
Gluteal HS
In the gluteal subtype, HS lesions primarily appear on the buttocks and consists of follicular papules and folliculitis, according to Okoye. Patients tend to be current or former smokers, males, and have a lower BMI than patients of the axillary-mammary-inguinal HS subtype.
“These patients, I believe, are at increased risk for squamous cell carcinoma (SCC),” Okoye said. “I don't believe this is in the literature per se, but if you look at the literature on SCC and HS you will see that most of the lesions occur in the buttocks, SCC and HS are more common in men, in smokers, and in people who have this disease for 25 years or longer. So that really sounds like these patients to me.”
For treatment of this subtype, Okoye suggests using surgical excision and biologics, as well as monitoring for SCC in the involved area and cessation of smoking.
“So, my preferred therapy for these patients is surgery. I don't find that they respond very well to medical therapy. As a matter of fact, for some of these patients, I think it's a pilonidal cyst that has gone completely rogue and just needs come out. And then for most of them will do some kind of biologic,” Okoye said.
Reference:
1. Okoye G. My Approach to Treating Hidradenitis Suppurativa in Patients with Skin of Color. Presented at the: Skin of Color Update; September 10, 2021; Virtual.
Disclosure: Okoye is a consultant for Janssen and Unilever. She has also received a grant from Pfizer, and is on an advisory board for Lilly, Novartis, UCB, and Pfizer.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.