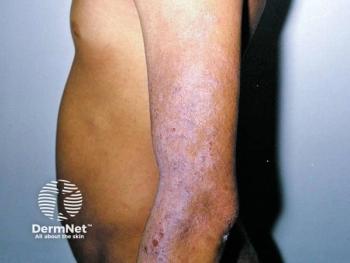
Psoriasis in Intertriginous Areas Has Negative Impact on Well-Being and Sexual Health
At a poster presentation at the 2022 SDPA Conference, patients with psoriasis reported symptoms in intertriginous areas at some point during the duration of their psoriasis.
A poster presentation1 from the 2022 Society of Dermatology Physician Assistants Conference in Miami, Florida, examined the quality of life of patients with psoriasis in intertriginous areas such as the groin, under the breasts, stomach folds, and buttocks. Study investigators determined 2 out of 3 patients with psoriasis in intertriginous areas had a negative impact on their lives, specifically their emotional well-being and their sexual health. Similarly, 2 out of 3 patients with psoriasis reported symptoms in intertriginous areas at some point during the duration of their psoriasis.
To determine the impact of psoriasis in intertriginous areas, Arcutis Biotherapeutics conducted a survey2 through the Harris Poll in the United States to better understand the perspectives and burden of patients with plaque psoriasis who use topical treatments to manage their disease. The survey was conducted online October 21, 2021-November 24, 2021, and included responses from 507 US adults aged 18 years and older, diagnosed with psoriasis by a healthcare provider. Out of the 507 responses, 320 participants had confirmed intertriginous area psoriasis.
To qualify for the study, participants had to use a topical treatment and not just a prescription injectable treatment for their psoriasis. Out of 320 confirmed participants, 44% were female and 55% were men. Regarding symptom severity in intertriginous areas, 20% of participants experienced mild symptoms, 67% experienced moderate symptoms, and 13% experienced severe symptoms. Additionally, 10% of participants reported having genital psoriasis, but genital involvement was not included in the intertriginous assessment.
Concerning the burden of psoriasis in intertriginous areas, 80% of patients reported they feel embarrassed, 79% had anxiety, and 69% were depressed. Reported rates of emotional impact were significantly higher in participants with groin involvement. Additionally, 45% of participants reported that intertriginous area psoriasis had a strong negative impact on sexual distress and anxiety, 39% reported a negative impact on intimate relationships, and 37% reported a negative impact on sexual function.
According to the study, “Nearly all participants (97%) say their intertriginous psoriasis has some effect on their overall quality of life, and most (66%) say this impact is slightly or moderately negative. Patients reporting a ‘very strong negative impact’ on their quality of life was numerically higher in patients with groin involvement (6%) and in females (15%) versus males (6%).”
Symptoms that caused the largest negative effects on the quality of life were:
- Itching
- Scaling
- Redness
- Skin cracking
Although 70% of participants with intertriginous area psoriasis showed their psoriasis to their health care provider, the most common area of intertriginous involvement was least likely to be shown to a health care provider. Between the buttocks was the most commonly reported intertriginous involvement, but only 19% of participants showed this area of their body to their health care provider. Typical protocols for health care provider visits range from some participants disrobing, while others remained fully clothed. Most participants believe the ability to use one treatment would be beneficial and increase their adherence.
Overall, intertriginous area psoriasis has a significant negative impact on patients and their emotional well-being, sexual health and relationships, and treatment adherence.
Reference
- Greiling T, Young M, Highman R. Patient perspectives on the prevalence and burden of intertriginous psoriasis: Results from a national survey of adults with psoriasis in the united states. Presented at the Society of Dermatology Physician Assistants Conference. Miami, Florida. November 17-20. https://www.sdpaconferences.org/hub/events/08d628c0-db6c-4633-8960-74ba986b221a/exhibitors/b8a550c6-ae1b-4e56-8556-0f937a1fcf9c
- Skin insights: Uncovering psoriasis: Arcutis Biotherapeutics. Published March 22, 2022. Accessed November 18, 2022.
https://www.arcutis.com/wp-content/uploads/2022/03/Skin-Insights-Uncovering-PsO-Infographic-Final-Print.pdf
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.