- Dermatology Times, March 2021 (Vol. 42, No. 3)
- Volume 42
- Issue 3
New Research Addresses Rosacea Challenges
Update tracks trending factors changing the treatment landscape.
Recent research on the importance of phenotype classification, comorbidities, triggers, and mechanism of action—including possible implications for metainflammation in coronavirus disease 2019 (COVID-19)—can expand the understanding of rosacea and suggests new directions for diagnosis and prognosis of this widespread skin disease.
Richard Gallo, MD, PhD, chair of the department of dermatology at the University of California San Diego (UCSD), provided an overview of current trends advancing rosacea therapy in his presentation at Maui Derm Live. The in-person dermatology continuing medical education (CME) conference in Hawaii was held concurrently with Maui Derm Connect, a virtual CME conference, from January 25 to January 29, 2021.1
His remarks were featured in the session, “Update 2021: Acne and Rosacea”, which highlighted new drugs, research, and expert insights into the management of rosacea and acne. Guy Webster, MD, PhD, clinical professor of Dermatology at Thomas Jefferson University, Philadelphia, Pennsylvania, moderated the panel which included speakers Lawrence Eichenfield, MD, vice chair of Dermatology and chief of Pediatric and Adolescent Dermatology at UCSD, and James Leyden, MD, emeritus professor CE of Dermatology at University of Pennsylvania School of Medicine, Philadelphia, Pennsylvania.
Gallo outlined 4 key areas driving change in addressing the challenges of rosacea.
PHENOTYPES MATTER
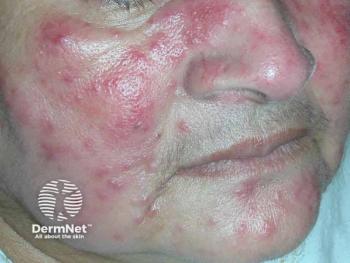
“Rosacea is now understood by phenotypes,” Gallo said. These phenotypes are (1) diagnostic: fixed centrofacial erythema in a characteristic pattern that may intensify periodically or phymatous changes; (2) major: flushing, papules and pustules, telangiectasia, and ocular manifestations; and (3) secondary: burning sensation; stinging sensation; edema; dryness and ocular manifestations.2
Gallo stressed the importance of using the phenotype-based classification system for rosacea rather than the subset-based method. Gallo noted limitations in describing a patient’s rosacea through subsets. Often, patients experience many subtypes simultaneously. Categorizing by phenotype allows health care professionals to track patient progress.
COMORBIDITY RISK EXPANDS
“Studies from 2020 confirmed a growing number of rosacea comorbidities including those related to cardiovascular, neurologic, and gastrointestinal risks,” said Gallo. Two meta-analyses found that patients with rosacea have a higher risk of hypertension, CRP, high LDL, epicardial fat, and insulin resistance, Gallo pointed out. According to 8 recent studies that evaluated a total of 200,000 patients, individuals who have rosacea also have an increased risk of migraine, Parkinson disease, and depression. Several studies pointed to higher risks of inflammatory bowel disease.
That is not all. “Innate immune dysfunction drives rosacea’s comorbidities,” said Gallo.
SUN EXPOSURE TOPS TRIGGER LIST
Ultraviolet (UV) light releases potential trigger molecules such a nucleic acids and other damage-associated molecular patterns. Although these endogenous danger molecules released from damaged or dying cells activate the innate immune system by interacting with pattern recognition receptors, they may also promote pathological inflammatory responses.
The cathelicidin peptide LL-37 is another factor. “LL-37 facilitates DNA recognition but does that explain UV sensitivity in patients with rosacea?” asked Gallo. In a study published last year, Gallo and his fellow authors saw results showing that LL-37 amplifies the response to UV products and predicts vascular cell adhesion molecule response in rosacea.3
MECHANISM OF ACTION
According to Gallo, research on rosacea’s mechanism of action could hold promise for better understanding COVID-19. Mutation scanning identified a possible structure necessary for inflammatory activity relating to COVID-19.”
Disclosure:
Gallo is a co-founder and holds equity interest in MatriSys Bioscience and is a consultant for Sente Inc.
References:
- Webster G. Eichenfield E, Layton J, et al. Update 2021: acne and rosacea. Pre- sented at: Maui Derm For Dermatologists 2021; January 25-29, 2021; Maui, Hawaii.
- Gallo R, Granstein R, Kang et al. Standard classification and pathophysiology of rosacea: The 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2018;1(78):148-155. doi:10.1016/j.jaad.2017.08.037
- Kulkarni NN, Takahashi T, Sanford JA, et al. Innate immune dysfunction in rosa- cea promotes photosensitivity and vascular adhesion molecule expression. J Invest Dermatol. 2020;40(3):645-655.e6. doi:10.1016/j.jid.2019.08.436
Articles in this issue
about 5 years ago
2021’s Top Challenges Facing Physiciansabout 5 years ago
Optimize Risk, Management of Pigmented Lesions in Pediatric Patientsabout 5 years ago
New E-BPO Improves Rosaceaabout 5 years ago
Systemic Therapy Advances for ADabout 5 years ago
Sebaceous Gland is Target for Acne Treatmentsabout 5 years ago
Quantifying is Key to Effective Hair Loss Treatmentabout 5 years ago
The Potential of Precision Medicineover 5 years ago
Novel Therapeutics Usher in a Year of Innovationover 5 years ago
Systemic Therapy Advances for Atopic Dermatitis













