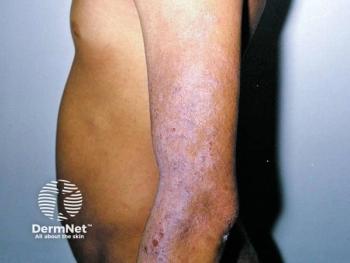
Mohs surgery for Bowen's disease?
I have tried unsuccessfully to find a single reference which describes the natural history of Bowen's disease.
The authors report on 270 cases of histologically diagnosed carcinoma in situ, 93 percent of which were on the head and neck region, and 50 percent of which were recurrent. After treatment with Mohs micrographic surgery, there was a 6 percent, five-year recurrence rate. Based on this data, the authors recommend this form of therapy, not only because of the high cure rate, but also because of the risk of invasive cancer in these lesions if incompletely removed. After reviewing this article in our Journal Club with a group of potentially impressionable dermatology residents, I decided to present another point review by submitting a letter to the editor of the Journal of the American Academy of Dermatology. After review by an outside reviewer and an associate editor of the Journal, my letter was rejected for publication. Somewhat annoyed, but undeterred, I have decided to air my opinion in this forum.
No doubt
What I question is why is this form of therapy necessary? Based on their review of the literature, the main rationale that the authors give for this aggressive form of treatment is that 3 percent to 8 percent of lesions of Bowen's disease progress to invasive carcinoma. They cite three references, two of which are from the same author. None of these references present experimental data supporting the high incidence of invasive carcinoma, but all simply quote a percentage of lesions which eventuate in invasive carcinoma.
I have tried unsuccessfully to find a single reference which describes the natural history of Bowen's disease. It is clear that there are cases of invasive carcinoma arising at sites of carcinoma in situ, but the published literature does not support the notion that this occurs with any great frequency.
The reviewer of my letter to the editor noted that Mohs micrographic surgery may be indicated when there is a major medical import of recurrence after inadequate removal, particularly of lesions in the head and neck area. As far as I am aware, the only import of recurrence of Bowen's disease is the physical presence of the lesion once again. A recurrence should not increase the biologic aggressiveness of the tumor, or make retreatment more problematic or risky.
If one were to agree that Mohs micrographic surgery is indicated in the treatment of Bowen's disease to reduce the likelihood of a recurrence of a potentially malignant lesion, why couldn't that same argument used to justify this form of therapy for actinic keratoses? It has been estimated that as many as 8 percent of these lesions progress to invasive squamous cell carcinoma (I don't believe that the incidence is remotely that high). The answer to this rhetorical question is that the severity of the disease does not fit the aggressiveness of therapy. There are several very good alternatives, including liquid nitrogen cryotherapy, topical fluorouracil and imiquimod. Mohs micrographic surgery would probably be more effective than these agents, but the added efficacy is not worth the medical and financial resources needed to accomplish the task.
BCC
A similar argument could be made for basal cell carcinoma. There is a 5 percent to 20 percent risk of recurrence of small nodular basal cell carcinomas after destruction by electrodesiccation and curettage. Why not reduce the risk to less than 5 percent by performing Mohs micrographic surgery on all basal cell carcinomas, even small ones? Once again, one must answer this with a philosophical and economic argument. We put a medical and financial value on diseases and their treatment. Small nodular basal cell carcinomas are fairly low on most people's scale of seriousness. Thus, less involved therapies are indicated.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.