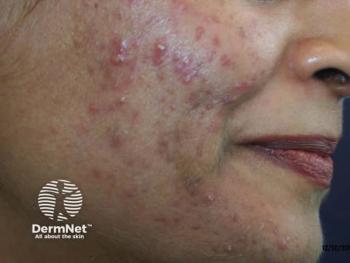
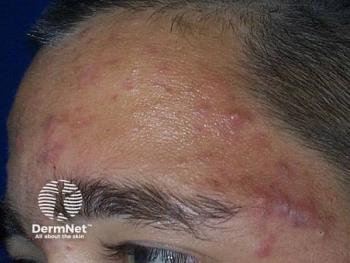
Going beyond clinical guidelines for acne treatment
Conventional acne treatment guidelines focus on acne severity. But there’s much more to effectively treating individual acne patients, according to an expert panel of 13 Canadian dermatologists, who developed a case-centered multifactorial consensus on acne management. Learn more
Conventional acne treatment guidelines focus on
READ:
According to the
Addressing these nuances results in dermatologists’ treating patients; not just acne, according to study author Jerry Tan, M.D., an adjunct professor in the department of medicine, Western University, and in private dermatology practice in Windsor, Ontario, Canada.
“Clinical severity is only a single component of the multifaceted way that patients present with a clinical condition. There are a number of other aspects that are critical to evaluate,” Dr. Tan says. “The panel tried to understand what additional detail can be provided as a guide to articulate what we do in the practice beyond what is available in clinical practice guidelines. So, it gives a more detailed summation of what clinicians often encounter and, then, have to resolve in terms of [an acne] patient’s specific needs.”
READ:
The paper offers eight case-based scenarios to illustrate the factors’ effects on dermatologists’ real-life encounters with acne patients - the skin tolerance differences, gender nuances, quality of life impact and more.
Still other issues, according to Dr. Tan, include treating acne patients who have dry versus normal skin; patients who have atopic dermatitis along with acne; fair versus dark skin patients; and those who have not only have facial acne, but also truncal acne. Dermatologists treat acne patients who are pregnant differently than they would nonpregnant females, who are on birth control pills and are not at risk of pregnancy. There might be different approaches to treating post-pubertal adults with persistent acne versus high school teens.
Acne severity
Of course, there’s always the issue of severity.
READ:
“In a patient with severe acne, what we’re looking for is to attenuate their acne as quickly as possible in order to reduce the inflammation and minimize the risk of scarring,” Dr. Tan says. “The standard therapy in that type of patient might be oral isotretinoin. And, if for some reason they don’t wish to be on that medication or they’ve had problems with it in the past, then we would look at using either oral antibiotics or hormones with medicated gels.”
Skin sensitivity
In reality, the dermatologist’s work is far from over. They also have to look at other factors, such as skin sensitivity.
“The problem in the patient with sensitive skin are retinoids - topical and oral isotretinoin - as they can increase skin sensitivity and irritation,” Dr. Tan says. “In those patients, what we really want to address is gentle cleansers and moisturizers to help repair abnormalities in the skin barrier. Then, as you’re engaged in treatment, to try to minimize any ongoing risk of skin barrier dysfunction.”
READ:
Options for managing acne patients with sensitive skin includes avoiding soaps, which can strip the skin of natural oils and moisture, as well as using moisturizers.
“There are some gels that don’t particularly irritate the skin, such as medications like topical dapsone and topical azelaic acid,” he says.
Quality of life impact
A patient’s assessment of how acne impacts his or her quality of life also comes into play. Dermatologists might make different treatment recommendations to acne patients whose quality of life is highly impacted by acne versus those whose quality of life impact is low - despite actual severity.
“If, for example, the patient quality of life impact is high, then, it’s important to engage in dialogue to try and understand why, particularly if acne severity is low,” he says.
A mismatch of actual severity to reported quality of life impact could indicate an intrinsic or extrinsic psychological component.
“An intrinsic component might be an oppressive, compulsive sense of self and a need to look perfect. And extrinsic component that may trigger psychosocial impact is bullying in high school,” he says.
Identifying the degree of psychosocial impact determines whether a patient might need psychotherapy, as well as helps the dermatologist better educate the patient about potential supportive measures and treatment that would best help the individual.
Gender variables
Gender is another issue that can result in a dermatologist modifying treatment, according to the consensus paper.
“In our society, women are much more focused on their skin than young men are. In women, I generally find they are right on in terms of what I see is what they feel. That is, if we as physicians see mild to moderate acne, that’s what they see, as well. Or it might be upgraded based on what they feel,” he says. “But for some young men (in fact, with quite a few young men), what we see is actually more than what they feel. They feel like they might have less acne than what the people around them see.”
READ:
Young men might go to the doctor for acne treatment only because their parents insist they do.
“In a young man, the counseling is a little different,” he says.
The dermatologist can educate young males who aren’t too worried about their acne now, about the risk of scarring down the road. Upcoming changes in the way they feel about physical attractiveness, socialization, sports and more could also impact the way they feel about acne treatment, he said.
Dermatologists can help boys recognize their feelings about acne by asking them if they’re embarrassed when they’re around people or in sports. It’s then that they might realize that they don’t like taking their shirts off because of their truncal acne or feel embarrassed in specific social situations.
READ:
“Then, it’s a matter of educating them about giving them a chance to treat it to minimize increasing embarrassment over time, increasing impairment problems with socialization and possibly a problem with future scarring, which could be very hard to reverse,” he says.
Skin types
The varying effects of acne on skin photo types is a key consideration for successful long-term outcomes, according to Dr. Tan. More aggressive acne treatment in patients with dark skin types can prevent the hard-to-treat hyperpigmentation that results from acne.
“In patients who have darker skin, I’m a little more aggressive to minimize the risk of secondary lesions, which are the marks that are left,” he says.
Treating the whole patient and not just the skin condition not only impacts patient satisfaction with their outcomes, but also treatment adherence, according to Dr. Tan.
“You might find that patients who have very little impact in their daily lives might be less likely to stick to any therapy, whereas, those that find acne is a bother to their daily lives …they’re much more likely to have a positive outcome,” Dr. Tan says. “That’s why the case-based approach was taken, because it addresses the individual patient considerations, as opposed to acne severity as the sole issue.”
Reference: Lynde C, Tan J, Andriessen A, Barankin B, Dutil M, Gilbert M, Hong CH, Humphrey S, Rochette L, Toole J, Thomas R, Vender R, Wiseman M, Zip C. A consensus on acne management focused on specific patient features. J Cutan Med Surg. 2014 Jul-Aug;18(4):243-55.
Disclosure: Dr. Tan has been an advisor, consultant, trialist and/or speaker and has received grants and/or honoraria from Allergan, Bayer, Cipher, Galderma, Johnson & Johnson, Photocure, Roche, Stiefel/GSK and Valeant.