Diagnosing and Treating Different Pigmentation Disorders
At the 2022 SDPA Conference, Ted Rosen, MD, discusses mundane and rare diseases that often present as vitiligo.
At the 2022 Society of Dermatology Physician Assistants Conference in Miami, Florida, Ted Rosen, MD, professor, and vice-chair of dermatology at the Baylor College of Medicine in Houston, Texas, reviewed several adult pigmentation disorders that assume a pathologic “white” tone aside from the common cause of vitiligo. In this discussion, called "It's Not Always Vitiligo", Rosen discussed both mundane and rare diseases and disorders that call for medical physicians to construct a broad differential diagnosis for pigmentary disorders and described various therapeutic interventions for various causes.1
Rosen listed several disorders that often present as vitiligo:
- Tinea Versicolor: This is a common fungal skin infection that occurs when the fungus interferes with normal pigmentation of the skin, resulting in small, discolored patches. These patches may be lighter or darker in color than the surrounding skin and most commonly affect the trunk and shoulders. Depigmentation can be intensified by sun exposure. The condition is not painful or contagious and can be treated with antifungal creams, lotions, or shampoos. Antifungal creams, such as ketoconazole, can help treat tinea versicolor, but only in lotions, creams or shampoos. Rosen noted that oral tablets should not be used as a first-line treatment for fungal infections because the US Food and Drug Administration has issued warnings about them; they're associated with an increased risk of adrenal insufficiency, potentially fatal hepatotoxicity, and drug interactions, according to the US Food and Drug Administration.
- Idiopathic guttate hypomelanosis: This is a commonly acquired form of leukoderma that presents as small flat pale or white spots on the sun-exposed limbs. Idiopathic guttate hypomelanosis can affect both sexes, all races, and all skin phototypes but is more prominent in women and patients with skin of color. It presents as a smooth, hypopigmented, or depigmented macule on sun-exposed areas of the forearms, chest, and face. Rosen said there is no definite therapy for this condition; a combination of therapies such as steroids and laser treatment could
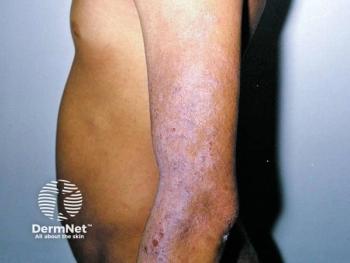
- Morphea (localized scleroderma): This condition causes hardening and discoloration of the skin. It is thought to be isolated to the skin without internal organ involvement as seen in systemic sclerosis. This is a rare disease, but more common in females and often begins in childhood, and the precise cause is still unknown. It can be difficult to treat. "So, we actually treat it with systemic therapy, typically with systemic steroids, that we give intermittently, along with long-term medications like methotrexate, which we use all the time in dermatology for a lot of other diseases", said Rosen.
Rosen concluded his discussion by recommending that clinicians treat patients with pigmentary disorders for 3 years after their condition improves and symptoms disappear to monitor for future outbreaks or recurrences.
Reference
Rosen T. It's not always vitiligo. Presented at the 2022 Society of Dermatology Physician Assistants Conference; November 17-20, 2022; Miami, Florida.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.