Derms, national psoriasis foundation tackle insurance issues
Though it's possible to get biologic drugs covered by many patients' insurance plans, sources agree it's rarely easy.
Though it's possible to get biologic drugs covered by many patients' insurance plans, sources agree it's rarely easy.
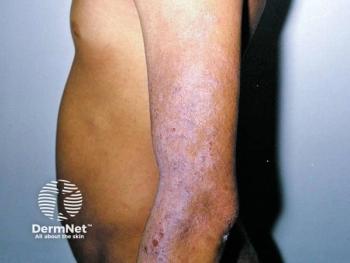
"We know that psoriasis is not simply a cosmetic problem," and that its impact on patients' physical and mental functioning can rival that of cancer, hypertension and heart disease (Rapp SR et al. J Am Acad Dermatol. 1999 Sep;41(3 Pt 1):401-407), says Sheila Rittenberg, National Psoriasis Foundation advocacy director.
Ms. Rittenberg says another problem is that, "The burden of cost is shifting to patients, through increasing co-pays, not only with biologics but also phototherapy and even some topicals."
Jeffrey M. Weinberg, M.D., says that while payors vary, "For the most part, when one does the requisite paperwork, biologic drugs are available to most patients."
However, he adds, "Very often, certain payors will put up barriers such as the need for other systemic treatments or light treatments prior to the use of biologics." He is assistant clinical professor of dermatology at Columbia University and director of the Clinical Research Center at St. Luke's-Roosevelt Hospital Center, New York.
INSURER CHANGES POLICY
One insurer whose policies were inadvertently harming patients was Blue Shield of California, Ms. Rittenberg says.
In early 2006, a National Psoriasis Foundation audit of 80 insurers revealed that this organization fell outside the mainstream of treatment coverage, she says. Specifically, the insurer required that patients meet a body surface area (BSA) requirement of 30 percent and fail two traditional systemic drugs and phototherapy, Ms. Rittenberg reports.
But through dialogue that began more than a year ago, she says, the National Psoriasis Foundation convinced the carrier to reduce its requirements to 13 percent BSA (most insurers require 10 percent) and failure of one systemic.
"They also still require failure of phototherapy," Ms. Rittenberg says, "but if phototherapy is contraindicated" or impractical, this requirement is waived. Blue Shield now also allows biologics for patients with psoriasis in vulnerable areas such as the face, palms, soles and genitals, while women of childbearing age may skip the systemic drug failure requirement, she adds.
The policy is "not perfect," Ms. Rittenberg says, "but it's a big improvement."
Ms. Rittenberg says that although Blue Shield of California initially was concerned about maverick dermatologists whose biologic utilization might outstrip the standard of care, the National Psoriasis Foundation was able to educate managers about how dermatologists treat psoriasis.
"By and large," she explains, "dermatologists don't jump into injectables or infusion regimens, and requiring one systemic medication is enough of a hurdle to ensure that biologics are not prescribed casually."
The National Psoriasis Foundation also learned about healthcare payors' competing priorities and need for education regarding psoriasis, Ms. Rittenberg says.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.