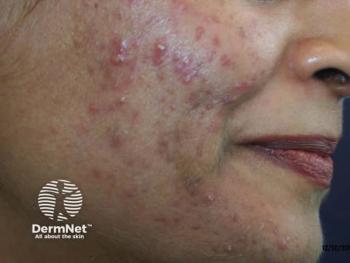
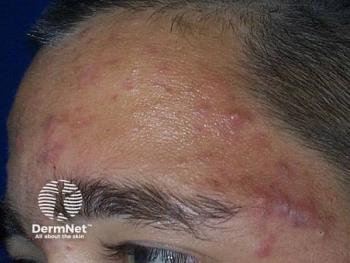
Cost is a barrier to medication adherence
Patient nonadherence to costly acne medications may be overcome by physicians telling patients upfront that preferred medications might be expensive.
This is important because a study in JAMA Dermatology of structured interviews with 26 nonadherent patients from four dermatology practices in the Philadelphia area found that cost was the major barrier to initiating therapy.
“I suspected that cost was increasingly a barrier to patients receiving medications, and acne was a prime example,” says co-author Jules Lipoff, M.D., an assistant professor of dermatology at the University of Pennsylvania. “More and more, insurances are requiring prior authorizations for medications or have high deductibles.”
Dr. Lipoff tells Dermatology Times that he finds out later from patients that they did not fill prescriptions, although he assumed that had. “I also receive too many calls from patients that a medication, even a generic topical medication that I expected to be inexpensive, is $200 out of pocket.”
Dr. Lipoff thought it was important to investigate, in depth, the barriers, the patient experience and what goes through a patient's mind when they do not follow through in filling a prescription.
The patient interviews revealed that 65% of patients had intended to fill prescriptions, but did not because of cost or coverage-related barriers. High out-of-pocket cost was cited by 42% of patients and lack of insurance coverage by 38%.
In addition, 54% of patients were surprised by high medication cost when visiting pharmacies.
Similarly, 19% of patients reported receiving confusing and inconsistent instructions from different sources about prior authorization; fragmented interaction between the physician, pharmacy staff and physician’s office staff; and confusion over their own role in the prior authorization process.
Dr. Lipoff expected that cost would be the major barrier to adherence, “and our findings support that. On the other hand, I was surprised how little patients expected physicians to be aware of cost as an issue. I believe that cost is just as important as safety and efficacy in the process of deciding if a patient should get a medication, and yet we do not talk about it much at all with patients.”
Another surprise to Dr. Lipoff was that even if patients did not fill a prescription, “they usually still considered their office visit as having value. This highlights what a magnificent opportunity we have as dermatologists to make a difference with cost-effective care.”
Dr. Lipoff says that most patients dislike the generic backup plan, which they are asked to call if there is a problem filling a prescription. “Instead, patients want to be provided a clear plan of action; for instance, with a specific back-up prescription or over-the-counter alternative if a medication is not covered or is too expensive,” he explains.
Study patients shared diverse approaches offered by their physicians to secure medications easier: asking patients to call back (7% of interviewees), suggesting patients shop around for medication (7%), proposing alternatives to non-covered, first-line medication (7%) and offering coupons to subsidize medication cost (4%).
Overall, 23% of patients felt positive when physicians provided backup plans if the preferred medication was unavailable and 19% appreciated a frank discussion about cost.
Independent of medication cost, though, 38% of patients reported treatment plan reservations, foremost concerns about adverse effects (15%) and believing that their acne was not serious enough to warrant medication (12%).
Dr. Lipoff says it is frustrating that physicians are unable to accurately predict what the cost will be for a patient when they arrive at a pharmacy. “It is upsetting that prices for medications can vary so much between pharmacies and that patients may not know their options,” he notes. “If there was better connectivity and transparency, things would be much easier.”
Dr. Lipoff would like to develop a toolbox to improve patient adherence, based on the study’s findings. “Though we often can anticipate which medications will likely be problematic, it is a constantly shifting enigma that makes it difficult to predict,” he admits.
Dr. Lipoff’s hope is that in the future, “doctors will be able to choose prescriptions with the out-of-pocket costs immediately available at the time of the decision-making process with patients.”
Disclosures:
The study was funded by a Pfizer Independent Grant for Learning and Change from the American Academy of Dermatology.
References:
Kira L. Ryskina, Erica Goldberg, Briana Lott, Davis Hermann, John S. Barbieri, Jules B. Lipoff. “The Role of the Physician in Patient Perceptions of Barriers to Primary Adherence with Acne Medications.” JAMA Dermatology. Published online February 28, 2018.