- Dermatology Times, September 2020 (Vol. 41, No. 9)
- Volume 41
- Issue 9
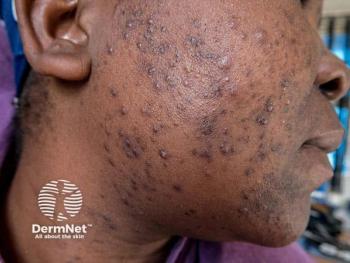
Artificial intelligence algorithm effectively evaluates acne severity
The implementation of artificial intelligence technology in the long-term management and follow-up of acne patients may help to improve patient treatment outcomes.
A novel artificial intelligence algorithm (AIA) appears effective in accurately assessing acne severity and lesion quantification via smartphone application, a recent study found.1
“This is the first validated AI algorithm which, using smartphones, allows the grading of acne severity based on the GEA scale. It provides a fast determination of the severity of acne and identifies the different lesion types, thus supporting the early therapeutic management of acne patients,” says Sophie Seité, Ph.D., La Roche-Posay Dermatological Laboratories, Levallois-Perret, France, and co-author of the study.
RELATED:
Dr. Seité and fellow colleagues developed the novel AIA for acne severity assessment based on the Global Acne Severity (GEA) scale and for acne lesion identification and compared it to clinical diagnosis by trained dermatologists.
In the five-stage development of the AIA, the researchers collected 5,972 images (face, right and left profiles) from 1,072 acne patients from France (32.7%), South Africa (46.5%), China (14.4%), India (5.1%), and Brazil (1.3%) using one or two types of smartphone for each patient [IOS (n=2,933) and Android (n=3,039) systems].
Three dermatologists assessed GEA for each patient on images. The GEA for each patient as assessed by the majority of dermatologists was used to train the algorithm. Using a tagging tool, dermatologists quantified lesions and identified post-inflammatory hyperpigmentation (PIHP) via images.
The model algorithm was then trained using 4,958 images corresponding to 903 patients associated with their GEA grade as well as images with tagged lesions and PIHP (2,939 tagged inflammatory lesions, 7,603 tagged non-inflammatory lesions and 5,702 tagged PIHP). Researchers then tested the algorithm internally using 1,014 new images from 169 acne patients.
For lesions and PIHP identification, results were submitted to the dermatologist for correction, which led to refinements and improvement of the algorithm in further versions. After improving the algorithm, the GEA grading reached 68%, which the researchers found was similar to the grade provided by the majority of dermatologists.
The correct grading and identification of acne lesions is the first step in the successful treatment of acne and, according to Dr. Seité, the promising results achieved with the AIA could prove to be useful in forging future management strategies for acne patients.
“With a decreasing number of dermatologists over the last decades, getting appointments with dermatologists has become more and more difficult for patients, resulting in irregular patient follow‐up, poor treatment outcome and a positive correlation between the duration of the disease prior to treatment and the development of scars,” Dr. Seité says.
On a larger scale going forward, Dr. Seité says that the study results essentially highlight the need for an appropriate and timely management of acne patients to avoid the development of residual hyperpigmentation and scars or a negative impact on the patient's quality of life. As such, the introduction and implementation of AIA technology can have a positive impact on patient outcomes.
“Non‐adherence to acne treatment is a common problem worldwide and this application can help practitioners evaluate their patients’ improvement between consultations. Such an approach can help for early management and serve as an educative tool to help the parents and or adolescents to better follow prescribed acne treatments,” Dr. Seité says.
Disclosure:
Dr. Seite, D Moyal, and G. Le Dantec are employees of La Roche-Posay, France.
Reference:
1 Dreno B, Moyal D, Benzaquen M, Khammari A, Le Dantec G, Seite S. Development and accuracy of an artificial intelligence algorithm for acne evaluation. – AAD poster, Denver 2020
Articles in this issue
over 5 years ago
Will OSHA cite me for requesting employees not wear masks?over 5 years ago
How safe are cosmetics?over 5 years ago
Pretreatment punch technique guides safe injectionover 5 years ago
What we know (and don’t) about dietary effects on skin agingover 5 years ago
Microbiome-based treatments not ready for prime timeover 5 years ago
Emerging options for high-risk melanomaover 5 years ago
Phenotypes inform management optionsover 5 years ago
AI has potential to improve melanoma detectionNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.