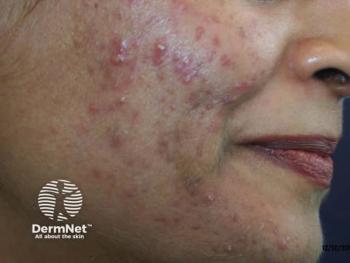
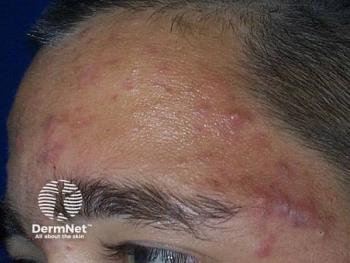
Add-on statins effective in acne
Oral and topical statins can be an effective addition to treatment for acne vulgaris when combined with standard treatment, suggests the results of a study published online in Current Clinical Pharmacology.
Oral and topical statins can be an effective addition to treatment for acne vulgaris when combined with standard treatment, suggests the results of a study published online in Current Clinical Pharmacology.
Inflammatory responses are known to play an important role in the development of inflammatory acne lesions. Many studies have demonstrated that statins have anti-inflammatory effects and some studies have shown the drugs to be effective for the treatment of other dermatological conditions such as dermatitis, vitiligo and psoriasis, researchers wrote in the International Journal of Dermatology.
Researchers at the Hamadan University of Medical Sciences in Iran, undertook a randomized double-blind placebo-controlled trial to look at the effectiveness of oral and topical simvastatin as an adjunct therapy in acne vulgaris.
The study included 76 patients with moderate to very severe acne vulgaris who were all treated with oral azithromycin (250 mg three times a week) and topical benzoyl peroxide gel (5% once daily) for eight weeks and additional treatment according to which of three treatment group they were randomly assigned to.
Patients in the oral group received 20mg/day of oral simvastatin and a blank topical solution. Patients in the topical group received simvastatin 1% topical solution and oral placebo. And, patients in the placebo group received oral placebo and blank topical solution.
Severity of acne was determined at baseline and after eight weeks of treatment using the Global Acne Grading System and compared between groups.
Acne severity scores decreased significantly in all three groups over eight weeks. Topical simvastatin was associated with the greatest decrease in acne severity compared with oral simvastatin and placebo, while oral simvastatin appeared to be superior to placebo.
In the topical group baseline severity was 40.57±9.37 (mean±SD) and fell to 14.15±4.58 over the eight weeks – a fall of 25.62±10.70 (p<0.001). In the oral group baseline severity was 34.11±8.02 and fell by 17.11±11.43 to 13.80±9.95. The smallest fall in acne severity score of 11.50±6.57 occurred in the placebo group taking mean severity from 30.45±8.94 to 17.13±9.23.
Both oral and topical simvastatin were well tolerated and there were no significant differences in adverse treatment effects between the three groups.
“This study demonstrated that topical simvastatin solution 1% and oral simvastatin (20mg/day) effectively reduce acne severity and were effective in ameliorating moderate to very severe acne vulgaris lesions. Although preliminary, the results of this study showed that oral and topical statins, drugs with anti-inflammatory properties, can be considered as effective treatment for acne vulgaris as an adjunct to standard treatment,” the authors wrote.
Limitations of the current studies included its small size and duration and not measuring the blood lipid profiles of patients which meant any association between the effect of simvastatin on blood lipid profiles and its effects on acne lesions could not be determined.
“Designing studies with larger sample size and considering the changes of patients’ blood lipid profile, as well as using improved formulation of topical simvastatin and considering the formulation’s stability are needed to further confirm our results,” the authors wrote.
A previous study evaluating the efficacy of topical atorvastatin solution in the treatment of papulopustular acne vulgaris in a one-month double blind randomised clinical trial found no significant differences between placebo and atorvastatin topical solution.
That study’s small sample size, short duration and type of statin studied might have affected the results. “Some studies (DOI:10.1111/j.2042-7158.2011.01302.x) showed that simvastatin is more effective and more powerful than other statins in the improvement of skin inflammation,” the authors wrote.
REFERENCES
Ahmadvand A, Yazdanfar A, Yasrebifar F, Mohammadi Y, Mahjoub R, Mehrpooya M. Evaluation the effects of oral and topical simvastatin as adjunct therapy in the treatment of acne vulgaris [published online August 21, 2018]. Curr Clin Pharmacol. doi:10.2174/1574884713666180821143545
Jowkar F, Namazi MR. Statins in dermatology. International journal of dermatology 49(11):1235-43
DOI: 10.1111/j.1365-4632.2010.04579.x
Bracht L, Caparroz-Assef SM, Magon TF, Ritter AM, Cuman RK, Bersani-Amado CA.
Topical anti-inflammatory effect of hypocholesterolaemic drugs. J Pharm Pharmacol. 2011 Jul;63(7):971-5. doi: 10.1111/j.2042-7158.2011.01302.x. Epub 2011 May 19.