- Dermatology Times, August 2022 (Vol. 43. No. 8)
- Volume 43
- Issue 8
Acne Updates: Pearls on Treating Acne from a Recent Maui Derm Conference
Julie Harper, MD, a board-certified dermatologist in private practice in Birmingham, Alabama, a founding director and past president of the American Acne and Rosacea Society, gave a presentation on acne treatment updates at the Maui Derm NP+PA Summer 2022 conference.
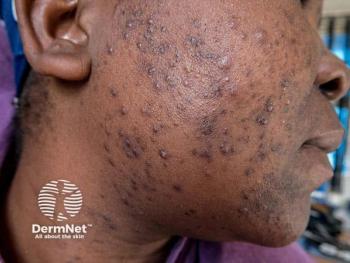
Acne is an extremely common skin disease and while particularly prevalent in adolescents, it can persist into adulthood as well. Most dermatology providers are very familiar with treating acne, as approximately 15% of the US population has suffered from acne and, by some estimates, nearly 9 out of 10 adolescents have also suffered from this condition. Julie Harper, MD, a board-certified dermatologist in private practice in Birmingham, Alabama, a founding director and past president of the American Acne and Rosacea Society, gave a presentation on acne treatment updates at the Maui Derm NP+PA Summer 2022 conference.
Before discussing treatments, Harper took time to highlight the goals of acne treatment and she shared her CLEAR acronym for effective treatment. The 3 most important goals of acne treatment are achieving meaningful improvements in lesion count, preventing sequalae, and improving quality of life. The CLEAR acronym can help accomplish this by reminding providers how to best counsel patients on effective treatment—C: communicate expectations, L: listen to customize treatment, E: treat early, A: treat aggressively, R; don’t resist isotretinoin. This was followed by a brief discussion on the role of topical therapy in acne treatment. Topical therapy is considered first-line treatment in most mild to moderate patients and it can be used as monotherapy or as combination therapy. However, topical antibiotics should rarely be used as monotherapy. There is also some utility for topical therapy in the treatment of acne sequelae.
Harper began her focused update on treatments with topical retinoids, which work by binding to the retinoic acid receptor, which modulates genes associated with acne etiology. Specifically, topical retinoids normalize follicular epithelial hyperkeratinization and are anti-inflammatory in nature. There have been 4 generations of FDA-approved topical retinoids, with the most recent approval for trifarotene 0.005% cream in 2019. This novel topical therapy is the first new retinoid molecule the FDA has approved in over 20 years and was studied on facial and truncal acne. In phase 3 clinical trials, trifarotene achieved a 42% IGA/PGA success rate at week 12 and a 65% absolute reduction in inflammatory lesions for both face and trunk.1 “Topical retinoids remain a cornerstone of acne treatment. I am grateful that we have seen innovation in this space. We have a whole new retinoid molecule, trifarotene, created to specifically and precisely target the retinoic acid receptors (RAR ) receptor,” Harper said.
Harper followed her discussion of trifarotene with another retinoid, tazarotene lotion 0.045%. This medication was FDA approved in 2019 for daily use in patients 9 years and older with moderate-to-severe acne. In a phase 2 study, tazarotene lotion performed better than tazarotene 0.1% cream in percent change in mean inflammatory and non-inflammatory lesions at week 12.2 The novel vehicle, polymeric emulsion technology, allows for a lower percentage of active ingredients, which improves the tolerability of tazarotene, traditionally an irritating agent. Before moving on to oral agents, Harper mentioned 2 other important topical therapies. First was E-tretinoin 0.1%/E-BPO 3% cream, which can be stabilized together through microencapsulation technology. This technology also allows for improved tolerability of the medication. Next, clascoterone was highlighted and the unique mechanism of action was displayed. Clascoterone is a topical anti-androgen that binds to the androgen receptor and has limited systemic activity.3 In 1 clinical trial, IGA treatment success for clascoterone was 16.1% vs 7% for the vehicle. This medication is the first topical antiandrogen for acne and is appropriate for use in both male and female patients. “We all have a tendency to think of our oral antibiotics in the management of acne as being the heavy lifter once they are added to a treatment regimen, but in fact the topicals are the unsung heroes,” Harper said. “While there are no head-to-head studies, clinical trials consistently show more acne patients achieve clear or almost clear with topical agents than with oral antibiotics.”
Harper also discussed oral therapy, which she said is equally as important as topical therapy. Oral therapy is recommended for moderate-to-severe acne that does not respond to other treatments or for inflammatory acne that is nonresponsive to topical antibiotics. Sarecycline, the newest oral antibiotic therapy, offers a narrow spectrum of therapy because it has a minimal effect against gram-negative bacilli. The advantage of this narrow spectrum may be a reduced tendency to disrupt normal gut flora.4 Sarecycline is taken once a day with or without food, and adverse events, while uncommon, include nausea and vaginal yeast infections. Its activity against C acnes is equivalent to that of doxycycline and minocycline.
Harper highlighted spironolactone oral therapy, which is not FDA approved for acne treatment but remains a popular option. She reviewed some high-yield pearls when using spironolactone. There is no need to check potassium in healthy women (between aged 18 and 45 years).5 There is no evidence of an increased risk of breast cancer, despite its FDA black box warning stating that “spironolactone has been shown to be a tumorigen in chronic toxicity study in rats.”6 Spironolactone takes 2 to 3 months to achieve optimal efficacy. An ideal way to use this medication is in combination with other acne treatments (topical therapies or oral antibiotics) and it even can be used in combination with oral contraceptives.7 Practically, dosage should be between 25 and 200 mg, but Harper prefers a maximum dose of 100 mg. A higher dose of spironolactone will lead to a high rate of side effects.
Harper ended her talk with isotretinoin, one of the most commonly used medications for the treatment of acne. She noted that the goal of isotretinoin therapy is complete clearance with 1 course of treatment while minimizing adverse effects and risks. An appropriate end point often varies by provider but a study by Tan et al found that the traditional end point dose of 120 to 150 mg/kg appears to vary with severity.8 Optimal end point dosing of isotretinoin has the goal of preventing relapse. Relapse can be defined in different ways, such as deterioration in acne requiring systemic therapy and those who require retreatment with oral isotretinoin.9,10 Relapses still occur in 20% to 30% of cases and less than 120 mg/kg is considered a cumulative dose that is too low. Patient characteristics that make relapse more common include younger age, male gender, severe presentation, females with polycystic ovary syndrome, and patients who present with a large number of comedones.
Harper reviewed laboratory monitoring with isotretinoin therapy. A study by Zane et al found that the greatest perturbation in laboratory abnormalities on isotretinoin were in triglycerides and total cholesterol.11 As such, the FDA package insert states that “blood lipid determination should be performed before isotretinoin is given and then at intervals until lipid response is established, which is usually about 4 weeks.” A meta-analysis on laboratory evaluation of isotretinoin found that while lab values demonstrated a change from baseline, none of them were considered high risk changes.12 The authors recommended performing lipid and hepatic panels at baseline and 2 months after therapy, with repeat labs dictated by medical history.
Harper wrapped up her presentation with a discussion on the risk of depression and suicide in patients on isotretinoin therapy, a traditionally contentious topic. A systematic review on the topic conducted by Huang et al in The Journal of The American Academy of Dermatology analyzed 31 studies and found that only 1 had evidence to show that isotretinoin significantly increased the risk of depression.12 The authors concluded that although individual susceptibility to depression cannot be ruled out, isotretinoin can be safely used without increasing the risk of depression. Another medical expenditure panel survey study, which utilized questionnaires like the Kessler 6-Item Psychological Distress Scale, found that patients on isotretinoin had fewer depressive symptoms than those on oral antibiotics and had less psychological distress.13
It is exciting to see new innovation in the treatment of acne and review the critical data on traditional therapies. Given the frequency with which this condition is seen in the dermatologist’s office, the management of acne is always an important topic to stay updated on.
Disclosures:
Harper is a consultant and/or speaker for Almirall, Cassiopea Pharmaceuticals, Cutera, EPI Health, Galderma, Journey Medical Corporation, L’Oréal, Ortho Pharmaceutical, Sol-Gel, SUN Dermatology, and VYNE Therapeutics. She is also an investigator for Almirall. For full list of references, see dermatology-times.com
References:
1. Tan J, Thiboutot D, Popp G, et al. Randomized phase 3 evaluation of trifarotene 50 μg/g cream treatment of moderate facial and truncal acne. J Am Acad Dermatol. 2019;80(6):1691-1699. doi:10.1016/j.jaad.2019.02.044
2. Tanghetti EA, Kircik LH, Green LJ, et al. A phase 2, multicenter, double-blind, randomized, vehicle-controlled clinical study to compare the safety and efficacy of a novel tazarotene 0.045% lotion and tazarotene 0.1% cream in the treatment of moderate-to-severe acne vulgaris. J Drugs Dermatol. 2019;18(6):542.
3. Hebert A, Thiboutot D, Stein Gold L, et al. Efficacy and Safety of Topical Clascoterone Cream, 1%, for Treatment in Patients With Facial Acne: Two Phase 3 Randomized Clinical Trials. JAMA Dermatol. 2020;156(6):621- 630. doi:10.10 01/jamadermatol.2020.0465
4. Zhanel G, Critchley I, Lin LY, Alvandi N. Micro-biological profile of sarecycline, a novel targeted spectrum tetracycline for the treatment of acne vulgaris. Antimicrob Agents Chemther. 2019;63(1):e01297-18. doi:10.1128/A AC.01297-18
5. Plovanich M, Weng QY, Mostaghimi A. Low usefulness of potassium monitoring among healthy young women taking spironolactone for acne. JAMA Dermatology. 2015;151(9):941-944. doi:10.1001/jamadermatol.2015.34
6. Wei C, Bovonratwet P, Gu A, Moawad G, Silver-berg JI, Friedman AJ. Spironolactone use does not increase the risk of female breast cancer recurrence: a retrospective analysis. J Am Acad Dermatol. 2020;83(4):1021-1027. doi:10.1016/ j.jaad.2020.05.081
7. Garg V, Choi JK, James WD, Barbieri JS. Long-term use of spironolactone for acne in women: a case series of 403 patients. J Am Acad Dermatol. 2021;84(5):1348-1355. doi:10.1016/j.jaad.2020.12.071
8. Tan J, Knezevic S, Boyal S, Waterman B, Janik T. Evaluation of evidence for acne remission with oral isotretinoin cumulative dosing of 120-150 mg/kg. J Cutan Med Surg. 2016;20(1):13-20. doi:10.1177/1203475415595776
9. Strauss JS, Rapini RP, Shalita AR, et al. Isotretinoin therapy for acne: results of a multicenter dose-response study. J Am Acad Dermatol. 1984;10(3):490 -496. doi:10.1016/s0190 -9622(84)80100 - 0
10. Layton AM, Knaggs H, Taylor J, Cunliffe WJ. Isotretinoin for acne vulgaris--10 years later: a safe and successful treatment. Br J Dermatol. 1993;129(3):292-296. d o i :10 .1111/ j .13 6 5 - 213 3 .19 9 3 . t b118 4 9. x
11. Zane LT, Leyden WA, Marqueling AL, Manos MM. A population-based analysis of laboratory abnormalities during isotretinoin therapy for acne vulgaris. Arch Dermatol. 20 06;142(8):1016 -1022. doi:10.10 01/a r c h d e r m .142.8.1016
12. Huang YC, Cheng YC. Isotretinoin treatment for acne and risk of depression: a systematic review and meta-analysis. J Am Acad Dermatol. 2017;76(6):1068 -1076.e9. doi:10.1016/ j.jaad.2016.12.028
13. Hekmatjah J, Chat VS, Sierro TJ, Read C, Kassardjian AA, Armstrong AW. Differences in depression and distress between acne patients on isotretinoin vs oral antibiotics. J Drugs Dermatol. 2021;20(2):172-177. doi:10.36849/JDD.5559
14. J. Harper, H. Baldwin, D. Eichenfield. Acne and Rosacea Update 2022. Presented at Maui Derm NP+PA Summer 2022; June 23-25, 2022; Colorado Springs, Colorado.
Articles in this issue
over 3 years ago
Diagnostic Approaches for Melasma and Vitiligoover 3 years ago
When to Progress to Systemic Therapyover 3 years ago
Focusing on Feetover 3 years ago
He Is my Covering Physician. Why Am I Being Sued?over 3 years ago
Mouse Model May Shed Light on APC mutations in brain metastasesover 3 years ago
FDA Approves Roflumilast Cream 0.3% for Plaque Psoriasisover 3 years ago
How to Tackle Challenging Cases in DermatologyNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.