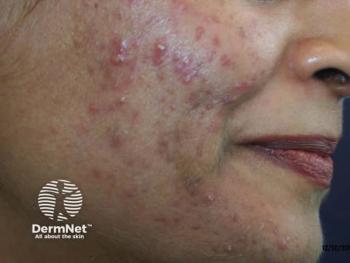
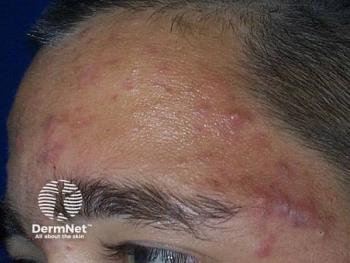
Acne research goals should focus on inflammation
The psychological distress caused by scarring and PIH following long-term acne disease can be devastating, begging the need for more effective therapeutic options.
Jersey City, N.J. - Scarring and
As such, dermatologic research should not only focus on the pathogenesis of acne, its treatment and management, but also investigate more effective treatment options for those patients with subsequent scarring and PIH from this condition, according to an expert.
“The amount of psychological harm that scarring and PIH inflicts on acne sufferers can even be greater than the condition itself however, there is a dearth of research and innovation regarding these long-term consequences of acne disease,” says Paul Mouser, Ph.D., principal scientist, Ashland Specialty Ingredients, a commercial unit of Ashland, Bridgewater, N.J. “Therefore, I believe that the goals of research in this field should also encompass more
Several converging lines of evidence indicate that inflammation may be present throughout the development of acne lesions, Dr. Mouser says, both during the latter stages where inflammatory papules, pustules and nodules are present and during the early stages of lesion development, in microcomedones and comedones. When the inflammation resolves, PIH and/or scarring often appears on the skin where the acne lesions once were. Here, atrophic scars are the most common type of acne scar seen, which include icepick-type scars, followed by boxcar and rolling scars.
Assessing inflammation
Not all acne patients are created equal, however, as the likelihood of
Other research has shown that T cells that are isolated from acne lesions are P. acnes reactive (Mouser PE, Baker BS, Seaton ED, Chu AC. J Invest Dermatol. 2003;121(5):1226-1228). According to Dr. Mouser, those patients who have a specific response to Propionibacterium acnes will have worse acne and possibly worse scarring due to the exaggerated immune response they have to P. acnes.
“The immune infiltrate in scarrers compared to non-scarrers can be very different and depending how the patient’s immune system will react to Propionibacterium acnes, the subsequent potential scarring can be equally diverse,” Dr. Mouser says.
Extracellular matrix remodeling (ECM) also plays a pivotal role in the development of scars in acne patients. Histologically, atrophic scars will exhibit a thinning of the skin, loss of elastin and dermal fat as well as defects in collagen production resulting in a downward pull of the dermis.
Role of MMPs
According to Dr. Mouser,
While Jalian et al found that MMP-1 and MMP-9 are present in acne lesions and that P. acnes is capable of significantly upregulating their mRNA expression in monocytes (Jalian HR, Liu PT, Kanchanapoomi M, et al. J Invest Dermatol. 2008;128(12):2777-2782), and Trivedi et al found increased expression of MMP-1 and MMP-3 in acne lesions (Trivedi NR, Gilliland KL, Zhao We, et al. J Invest Dermatol. 2006;126(5):1071-1079), Lee et al found that keratinocytes are an important source of MMPs in acne and that MMP-1, MMP-2, MMP-3, and MMP-9 were significantly upregulated in acne lesions by immunohistochemistry (Lee SE, Kim J-M, Jeong SK, et al. Arch Dermatol Res. 2010;302(10):745-756). All of these studies indicate and underscore the intricate and important role of MMPs in the development of scars in acne skin.
Similar to scarring acne, Dr. Mouser says PIH can also be a great source of psychological distress and can cause significant anxiety and lowered self-esteem in affected individuals. More frequently seen in patients with darker Fitzpatrick skin types, PIH develops in the same area as the preceding inflammation and although it can spontaneously remit, it often fades away very slowly and can sometimes persist for years.
Studies have demonstrated the melanocyte-stimulating properties of leukotrienes such as LT-C4 and LT-D4, prostaglandins E2 and D2, and thromboxane (TX)-2 (Morelli JG, Norris DA. J Invest Dermatol. 1993(100):191S-195S; and Tomita Y, Maeda K, Tagami H. Pigment Cell Melanoma Res. 1992;5(5):357-361), indicating the association of PIH with inflammation.
Many therapeutic modalities have been tried to improve PIH, including hydroquinone and a plethora of other topical agents that are aimed at interfering with the melanogenesis pathway, as well as chemical peels and energy-based modalities, all of which can achieve variable aesthetic outcomes in PIH.
“The goal is to understand better and find out why the inflammatory infiltrate is occurring in acne lesions. The data from the studies performed to date all appear to indicate that Propionibacterium acnes is a major player; however, if we could find the antigen, we could help prevent scarring from ever occurring,” Dr. Mouser says. “I believe that we currently have all of the tools in place to research this area and looking forward, this is where future studies should be focused.”
Disclosures: Dr. Mouser reports no relevant financial interests.
More on the psychological burden of acne