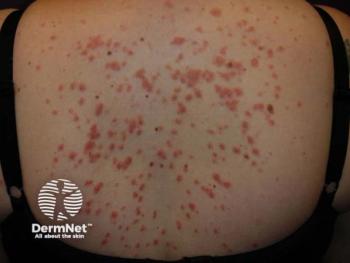
Topical guidelines will provide real-world guidance
Key Takeaways
- New guidelines emphasize real-world decision-making, patient preferences, and the chronic nature of psoriasis, highlighting the need for maintenance therapy.
- Distinctions between clinical and research severity scales are made, with subjective measures complementing clinical assessments for a comprehensive view of disease severity.
The latest set of guidelines for psoriasis being developed by the American Academy of Dermatology and the National Psoriasis Foundation will stress patient education and the need to align treatment strategies with patient lifestyles.
Pending joint guidelines from the American Academy of Dermatology (AAD) and the National Psoriasis Foundation (NPF) examine topical therapies for psoriasis from a practical perspective, addressing severity scales and alternative therapies along the way.
“This is not going to be exactly like the previous AAD topical guideline. In fact, it’s not going to cover just topical therapies,” says guidelines co-author Dario Kivelevitch, M.D. He is a dermatologist at Baylor University Medical Center in Dallas. Few new topical treatments for psoriasis have emerged since the 2009 publication of previous AAD topical psoriasis guidelines,1 he says. The main difference in the updated guidelines is their focus on real-world decisions.
Patient preferences
A patient preferences section stresses the need to align therapeutic strategies with patients’ likes and lifestyles. Vehicle selection also depends on the treatment area, says Dr. Kivelevitch.
“If you give someone an ointment to put on the face or hair-bearing areas, that person may not use it because it’s going to be uncomfortable or not cosmetically acceptable,” he says. Conversely, many patients prefer foams or solutions for the scalp.
“But it depends. It has to do with the physician’s communication with the patient and his or her preferences. I have seen patients who like greasy treatments on their scalp,” Dr. Kivelevitch says.
The new guidelines also emphasize the importance of educating patients about the chronic nature of psoriasis and the need for maintenance after flares subside.
RELATED:
“Many patients come back after using a topical treatment saying the treatment doesn’t work because they flared as soon as they stopped it,” he says.
This disconnect highlights a patient education problem - “physicians not explaining that this is a chronic disease, and if you stop treatment, it will come back,” Dr. Kivelevitch says.
Additionally, the guidelines address the role of steroid-sparing agents to minimize the risk of adverse effects due to topical steroid overuse.
“For the most part, patients fail to maintain long-term topical treatments,” he adds.
Severity scales
The new guidelines draw distinctions between tools for clinical use versus research settings. For example, body surface area (BSA) is a simple, straightforward measurement tool that is widely accepted in clinical practice. Conversely, more complex scales such as the Psoriasis Area and Severity Index are used in clinical trials but are generally too cumbersome for daily practice, he says.
More subjective calculations can help guide treatment decisions in situations where patients may not meet objective severity criteria.
“Patients may not fit in the classic classification of severe psoriasis - more than 10% BSA affected, yet they may have 3% or 4% BSA affecting the genitals, face and feet with a huge impact in their quality of life. In such cases topical treatments may not be enough,” Dr. Kivelevitch says. “Quality of life and other subjective severity measures can complement the clinical assessment tools to provide a better picture of the real severity of the disease.”
Alternative medicines
Acknowledging the popularity of and public interest in alternative treatments such as Chinese medicine, acupuncture and naturopathic ingredients, the guidelines emphasize that such treatments may complement but not replace traditional therapies.
“The guidelines do not recommend any alternative medicine in lieu of mainstream medicines. The idea is to provide information as to which treatments have been tested and have shown some evidence of possible benefit,” he says.
Guideline authors took care not to recommend any particular alternative treatments, he says, because such treatments generally lack evidence and/or show conflicting results. And some alternative therapies could be harmful. Examples include excessive vitamin D supplementation or St. John’s wort, which may be a photosensitizer.
Dr. Kivelevitch adds that although the new guidelines are virtually complete in draft form, they may undergo additional changes. At press time, the guidelines were under review by AAD and NPF officials. Once approved at this level, the document will be submitted for AAD member comments.
“I hope in the next couple of months, the guidelines should be published or ready to be published,” he says.
Disclosures:
Dr. Kivelevitch is an investigator for Arcutis and a speaker for Eli Lilly.
References:
1 Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 3. Guidelines of care for the management and treatment of psoriasis with topical therapies. J Am Acad Dermatol. 2009;60(4):643-59.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.