- General Dermatology
- Eczema
- Chronic Hand Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
- Prurigo Nodularis
Article
Systemic Oxidative Stress Plays Role in Etiopathogenesis of Melasma
Author(s):
Researchers noted that serum levels of malondialdehyde and vitamin C are indicators of the impairment caused by systemic oxidative stress.
According to researchers, systemic oxidative stress plays a significant role in the etiopathogenesis of melasma.
toa555/AdobeStock
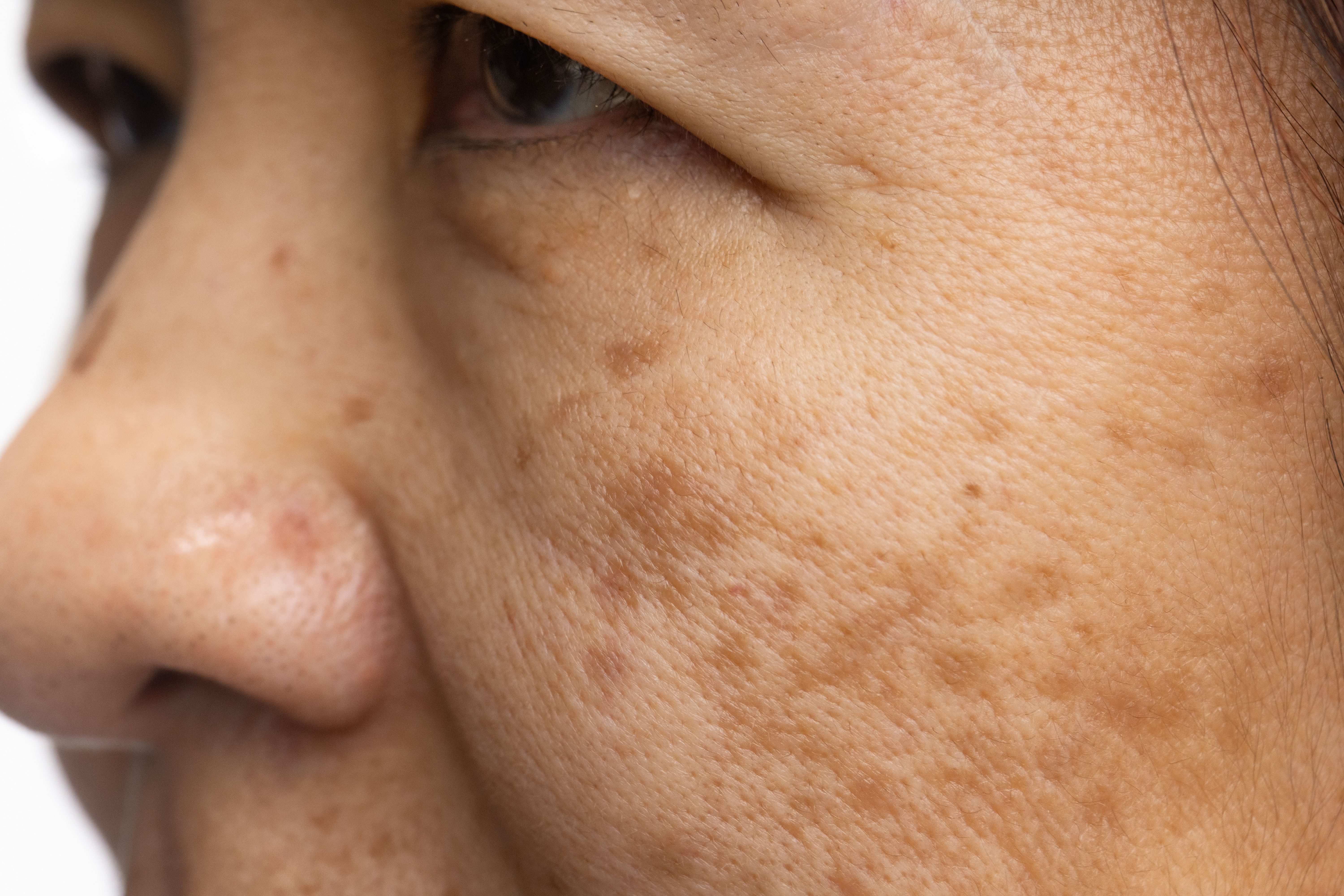
In a recent case-control study,1 researchers sought to determine the relationship between melasma and systemic oxidative stress, including its role in the etiopathogenesis of the condition and correlations between severity and extensiveness of disease. They cited prior research evaluating the significance of oxidative stress in several cutaneous disorders, such as: alopecia areata, atopic dermatitis, chronic wound progression, eczema, lichen planus, pemphigus vulgaris, psoriasis, rosacea, and vitiligo.
While there is not much research related to oxidative stress in the literature, Rahimi et al note that the relationship between melasma and antioxidants may suggest involvement of oxidative stress in the pathogenesis of melasma.
A total of 50 patients from a singular outpatient department were considered for study participation. All patients had received a melasma diagnosis and become members of the study’s case group. If patients in this cohort had previously been treated for melasma, they were required to undergo a 6-month washout period prior to participating. Researchers then recruited 50 healthy volunteers without melasma to become members of the control group; these volunteers were age, sex, and skin type- matched with members of the case group.
Patients were required to be non-smokers and have a minimum 3-month period wherein they did not consume alcohol, antioxidants, or oral contraceptives leading up to the start of the study. Patients who had been pregnant within a year leading up to the study or who had a history of other skin disorders, chronic diseases, or an immunocompromised status, were excluded from participation.
At inclusion, a dermatologist evaluated all participants and collected demographic and disease-specific data, including percentage of total face area affected by melasma and severity of disease, which was measured by the Melasma Area and Severity Index (MASI).
Blood samples were collected from all participants, and serum levels of several parameters were evaluated, including: catalase (CAT), glutathione peroxidase (GPX), malondialdehyde (MDA), protein carbonyl (PC), selenium (Se), superoxide dismutase (SOD), vitamin C, and vitamin E.
When comparing blood samples of patients in the case and control groups, researchers found that the average serum MDA level in members of the case group was 3.08 U/mL, while the average level among members of the control group was 2.35 U/mL. Furthermore, serum MDA levels had a significant and positive correlation with both MASI score and extension of disease.
Additionally, the average serum vitamin C score of patients in the case group was 2.16 μg/mL, while members of the control group had an average of 2.57 μg/mL. According to Rahimi et al, these differences between the control and case group were significant in nature.
“MDA was the most significant indicator of systemic OS (oxidative stress) in melasma and was correlated with both the severity and extension of the disease. Despite the controversial results of different studies, disrupted oxidant–antioxidant balance in melasma is the common finding in all previous reports as well as study,” according to Rahimi et al. “On the whole, the investigation into the relationship between systemic oxidative stress and melasma can provide new insights into the etiopathogenesis and, consequently, the treatment of this disease. Therefore, further studies are recommended on the indicators of OS in both the sera and skin lesions of the patients to reach a definitive conclusion. Moreover, future clinical trials focusing on the improvement of MASI by antioxidant supplementation to increase MDA would be necessary to confirm the association.”
Reference
- Rahimi H, Mirnezami M, Yazdabadi A, Hajihashemi A. Evaluation of systemic oxidative stress in patients with Melasma. J Cos Dermatol. Published online July 18, 2023. doi:10.1111/jocd.15924