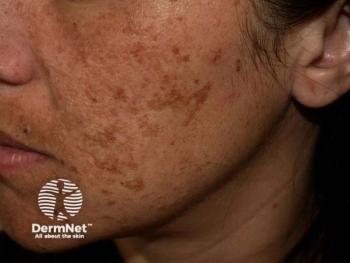
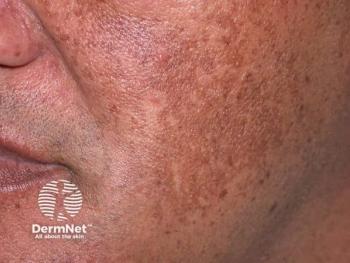
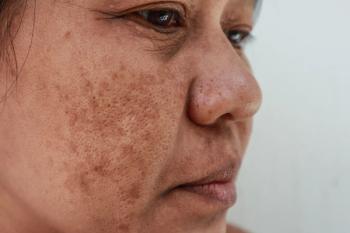
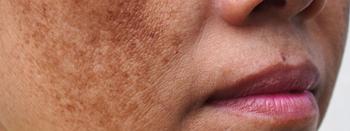
Sunscreen demonstrates strong therapeutic properties in patients with pigmentary disorders
The importance of blocking visible light in the treatment of pigmentary disorders is becoming clearer. One expert says photoprotection in patients with pigmentary conditions is a therapeutic cornerstone.
Dermatologists have long recommended sunscreens to prevent worsening of pigmentary disorders. But there’s mounting evidence that suggests sunscreen also has a therapeutic role in the treatment of melasma, post-inflammatory hyperpigmentation and chronic UV-induced hyperpigmentation, according to Susan C. Taylor, M.D., FAAD, who presented on the topic during the American Academy of Dermatology VMX 2020.1
The evidence
The role that sunscreen plays in melasma treatment isn’t new. Dr. Taylor referred to a study published in Cutis in 1983 in which researchers studied 53 melasma patients.2 All patients in the double-blind study received 4% hydroquinone, the gold standard melasma treatment, according to Dr. Taylor.
“One group received a broad-spectrum sunscreen and the other placebo. And we can see a significant difference in improvement of the melasma. We find that in the group that used the 4% hydroquinone as well as the broad-spectrum sunscreen, 96% improved, and this is in comparison to 80% who were in the placebo group who did not use sunscreen but only 4% hydroquinone. This confirms the positive role of sun protection in the treatment of melasma,” she says.
A more recent paper, published in 2019 in the Indian Journal of Dermatology, Venereology and Leprology looked at the impact of sunscreen on post-inflammatory hyperpigmentation and lentigines in 230 subjects.3
“The design of this particular trial is rather interesting in that all of the subjects were required to have sun exposure for two to four hours a day during the highest intensity of sunlight between 12 p.m. and 3 p.m.,” Dr. Taylor says. “Both groups used sunscreen twice a day for a 12-week period of time. But here’s the difference: Group A used an SPF 50 sunscreen with UVA protection and group B used SPF 19 again with equivalent UVA protection. They found there was equal improvement in the density of the pigmented spots and radiance of the skin in both groups.”
The study demonstrates the value of UVA radiation protection and suggests UVB protection isn’t as critical for improving post-inflammatory hyperpigmentation and lentigines, according to Dr. Taylor.
Authors of another study published in 2016 in Dermatologic Surgery of 32 subjects with photoaging who applied an SPF 30 sunscreen for a year found improvements in mottled and discrete pigmentation, as well as evenness in skin tone.4
Beyond UVA protection, the importance of blocking visible light in the treatment of pigmentary disorders is becoming clearer, according to Dr. Taylor. In a study of 10 subjects with skin types IV, V and VI whose backs were irradiated with either visible light alone or a combination of visible light and UVA1, researchers found the pigmentation induced by visible light was darker and more sustained than in the UVA1 group.5
“We’ve learned that it’s the shorter wavelengths of visible light—in the blue-violet range, that’s about 415 nm that induces significantly more hyperpigmentation as compared to the longer visible light wavelengths in the red-light spectrum, which is about 630 nm,” Dr. Taylor says.
Another lesson learned: visible blue light stimulates opsin-3, according to research published 2017 in the Journal of Investigative Dermatology.6
“This activates melanogenesis-associated transcription factor and other melanogenic enzymes, specifically tyrosinase and dopachrome, which form a protein complex primarily in the melanocytes of individuals with darker skin, which produces quite significant amounts of melanin. So, we need to start to think about our photoprotection encompassing visible light,” she says.
What blocks visible light? Iron oxide, made up of inorganic pigments that produce optically opaque sunscreen formulations, absorbs visible light and some ultraviolet wavelengths.
Dr. Taylor cited a study that demonstrates sunscreens that protect the skin from visible light in addition to UVA and UVB showed better effectiveness in melasma treatment and relapse compared to sunscreens that only protect against UVA and UVB.7 In that study of 61 melasma subjects, all received treatment with 4% hydroquinone and applied a broad-spectrum SPF 50 sunscreen.
“But here’s the difference. One arm of the study received the sunscreen that contained the visible light blocker iron oxide included and the other had no visible light blocker,” Dr. Taylor says. “What was demonstrated was that in eight weeks, the group with the visible light blocker had 77% improvement in the [Melasma Activity and Severity Index] MASI score compared to only 61% improvement in the group that did not have a visible light blocker (the UV-only blocker). I think this is pretty compelling.”
Researchers have found that a concentration of 2% iron oxide in sunscreens or foundations is needed to block the pigment enhancing effects of high-energy visible light.
Antioxidants, commonly added to sunscreens, also help to treat pigmentary disorders. In a study of 44 subjects who applied sunscreen containing spirulina and dimethylmethoxy chromanol twice a day for three months, researchers found the antioxidant supplementation significantly improved sun-induced skin damage.8
“There’s another antioxidant … Licochalcone A. It’s extracted from the root of the Glycyrrhiza inflate plant. It has been demonstrated to help block visible light and hence the generation of increased pigmentation and the mechanism has been worked out for Licochalcone A.9 So, this is another ingredient and antioxidant combined with sunscreen that can be effective for melasma, as well as for post-inflammatory hyperpigmentation,” Dr. Taylor says.
A logical next question among dermatologists is whether infrared radiation might also impact pigmentation and pigmentary disorders. Dr. Taylor doesn’t believe it does but pointed to the development of a new polymer coating that has been applied to zinc oxide and titanium dioxide particles.
“This polymer coating in a series of in vitro and ex vivo studies demonstrated the ability of mineral-based product formulations with the coating to provide protections against UV in the 290 to 440 nm range, as well as visible light, infrared radiation and environmental pollution, 10” Dr. Taylor says. “So, it’s something to keep in mind.”
Dr. Taylor concluded that photoprotection in patients with pigmentary conditions is a therapeutic cornerstone. For their patients with pigmentary disorders, dermatologists should consider recommending not only sunscreens that protect against UVA and UVB, but also visible light.
Disclosures:
Dr. Taylor is an advisory board member and speaker for Beiersdorf, Johnson and Johnson, as well as is an or investigator for Aclaris, Allergan, Amirall, Avon, Cann Tec, Croma Pharma, Galderma, Eli Lilly, L’Oreal, Ortho Dermatologic, Pfizer, Walgreens Boots.
References:
1 Taylor S. The Future of Photoprotection for Pigmentary Disorders. Presented at: American Academy of Dermatology VMX 2020, June 12-14, 2020.
2 Vázquez M, Sánchez JL.
3 Sarkar R, Garg VK, Jain A, et al.
4 Randhawa M, Wang S, Leyden JJ, Cula GO, Pagnoni A, Southall MD.
5 Kohli I, Chaowattanapanit S, Mohammad TF, et al.
6 Regazzetti C, Sormani L, Debayle D, et al.
7 Castanedo-cazares JP, Hernandez-blanco D, Carlos-ortega B, Fuentes-ahumada C, Torres-Álvarez B.
8 Souza C, Campos PMBGM.
9 Mann T, Eggers K, Rippke F, et al.
10 Bernstein EF, Sarkas HW, Boland P, Bouche D.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.