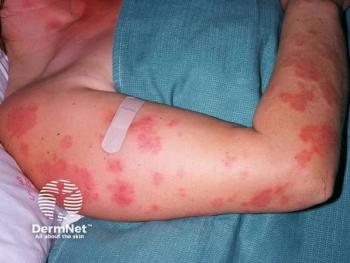
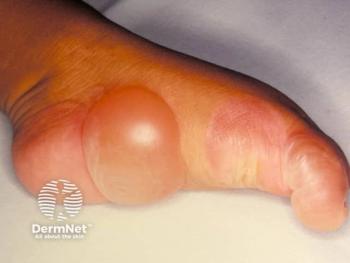
Stefan Weiss, MD, Discusses OM1’s New HS Dataset and Expanded Dermatology Network
The addition of an HS dataset adds approximately 26,000 new patient records.
According to OM1’s announcement, clinicians will now have access to treatment utilization and machine learning-generated Hurley Stage estimations through OM1’s augmented, automated, and manual note abstraction capabilities and clinical dataset. Clinicians can use the insights from OM1 to more accurately diagnose and stage HS progression. The new HS dataset includes natural history of disease and patient journeys, treatment effectiveness, phenotypic subtyping, and more. Additionally, the HS dataset breaks down electronic medical record demographical data including geography, comorbidities, treatments, and provider specialty, and enhances it with unstructured data from medical claims and physician notes of disease stage, anatomic location, and disease manifestation.
To further discuss the significance of OM1’s new HS dataset, Dermatology Times spoke with
Dermatology Times: Can you explain in more detail how OM1's expanded Dermatology Network, now including almost 26,000 hidradenitis suppurativa patient records, utilizes automated AI extraction to assist health care providers in diagnosing conditions earlier and staging disease progression for more targeted treatment plans?
Weiss: By creating disease severity estimations, AI modeling can leverage the data on the 26,000 patients to track improvement or progression longitudinally. This added insight is critical because if patients’ disease activity cannot be observed, we can’t know if their treatments are effective, their condition is worsening, or how disease activity correlates with other events in their medical history. Providers benefit from ‘filling in gaps’ in the record and richer visibility into what’s happening with their patients than would otherwise be available.
Dermatology Times: Could you elaborate on the ways in which OM1's expanded network aims to provide a clearer understanding of the patient journey from diagnosis onwards, specifically addressing the impact of skin diseases on a patient's mental health?
Weiss: The patient does not exist in a vacuum. The various organ systems are highly interrelated. Data that transcend a single disease state or organ system offers exponentially more valuable insights on the patient experience. The association between skin disease and mental health is extensively documented. In fact, nearly 20 years ago the first study identified the impact of psoriasis on social functioning to be greater than any other disease. Skin disorders, visible to the patient, and a reminder every time one looks in the mirror eventually take a toll on a person's mental well-being. Understanding this toll with a quantitative metric, like the PHQ9 is highly valuable. Dermatologists are not going to record that measure. However, linking patients across a dermatology and mental health data set can be insightful in illustrating these correlations.
Dermatology Times: What are some of the potential benefits and applications of the data collected through OM1's Dermatology Network in terms of improving patient care and mitigating the mental health implications associated with skin diseases?
Weiss: Unfortunately, most dermatologic diseases are viewed by policymakers as cosmetic. Their impact on mental health is neglected. Already a tragedy in this country, we need to do more to aid those suffering from mental illness. When that mental illness is triggered by a treatable skin condition, we have an opportunity to intercede early and successfully. However, insurance companies often refuse to pay for advanced therapeutics for those with skin disease. Documenting the impact of the disease on mental health and the improvement in mental functioning after treatment can be a powerful force for good in changing the patient journey.
Dermatology Times: What is the importance of gathering insights, including treatment effectiveness across different demographics and providers, and how this data can be used to accelerate research and improve clinical decision-making in the field of dermatology?
Weiss: Understanding the impact of a treatment on a disease across different populations allows physicians to personalize treatments. If we find across big data sets that certain patient populations respond better to certain drugs or therapeutic mechanisms it allows us to achieve the ultimate objective of getting the right drug to the right person at the right time.
Dermatology Times: Do you have any examples where OM1's datasets have revealed previously unknown trends or insights that have had a significant impact on patient care or dermatological research?
Weiss: One area of insight has been that the care of dermatologists meets the standards of health equity. Now, the health care system remains broken in that some groups have a disproportionately poor access to care. However, should access be obtained, the care received does not differ across sub-populations.
Reference
- OM1 launches hidradenitis suppurativa dataset to expand real-world evidence in dermatology. BusinessWire. News release. September 21, 2023. Accessed October 3, 2023.
https://www.businesswire.com/news/home/20230921621716/en/OM1-Launches-Hidradenitis-Suppurativa-Dataset-to-Expand-Real-World-Evidence-in-Dermatology
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.