Laser Therapy for Scars and Keloids
Jill Waibel, MD, discusses her recommendations on how to treat keloids and scaring using lasers in her presentation at the Skin of Color Update 2021.
Jill Waibel, MD, presented at the Skin of Color Update, held virtual September 10-12 on lasers and their uses for both scar and keloid treatment.1 Waibel is medical director and owner, Miami Dermatology and Laser Institute, subsection chief of dermatology, Baptist Hospital, medical director, Multidisciplinary Skin Cancer Clinic, Miami Cancer Institute, all in Miami Florida and Dermatology Times® editorial board member.
She explained that scar formation is affected by the level of wound trauma, personal genetics, and location of scar. Keloids tend to form in the same location multiple times due to tension; however, Waibel said that the issue could be deeper than what it seems.
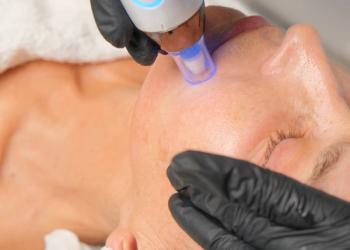
Although it is usually used for wrinkles, ablative fraction laser (AFL), according to Waibel, was the laser that changed the treatment world for scars. She says combination treatment is needed when choosing an approach, but the scar type determines the different combination therapies to use.
“The one thing that I almost always do with every scar patient I treat and every keloid patient I treat is laser assisted drug delivery,” Waibel said. She expanded on this, noting that when using a fractional ablative laser, columns open on the skin and these holes are open for about 48 hours. She said, most research suggests a physicians can inject FDA approved medication into a scar. Previously when she treated triplets, Waibel injected 1 of the triplets, resulting in the 1 patient healing 60% better than her other 2 sisters.
When treating hyperpigmentation, Waibel uses 1927 nm laser and AFL for treatment. For hypopigmentation, which she said is tough to treat, she said she can use a multitude of solutions, like a nonAFL (NAFL), AFL, AFL and bimatoprost, and CelluTome (KCI). When she uses bimatoprost, which is FDA approved to treat glaucoma, she injects immediately after the laser treatment then twice a day for a week, which repigments the skin.
For atrophic scars, the dermal depressions occur after a loss of dermal collagen and can represent a reconstruction challenge. Waibel’s solution is AFL with an after topical treatment of poly-L-lactic acid (PLLA) for both deep atrophic and thin skin atrophic scars. She reminds her patients that it does take 3 to 6 months for collagen remodeling.
For post inflammatory erythema (PIE) and post inflammatory hyperpigmentation (PIH), which she stated comes from acne which must be treated first. She treated a patient with a pulse dye laser, and while some inflammation remained, it stopped the spread.
When it comes to excessive scaring such as those created after surgery, the etiologies include location, hormones, genetics, chronic inflammation (acne), tension wound borders, and delayed epithelization. Waibel believes if a scar is less than 6 months old, it can be prevented, and they have to be treated gently and she tends to only use NAFL, and it works on all skin types.
For keloids, as the knowledge is still growing on how to treat them, Waibel explained that she never tells a patient it won’t come back after treatment. When treating keloids, she shaves off the keloid and then uses a laser, but never sutures as, in her experience, it makes the keloid come back worse than before. She uses is fractional laser and if the patient has not had surgery in that area before, she applies triamcinolone acetonide 10 mg. Waibel does not use a higher dose as it runs a risk of hyperpigmentation.
For burn and trauma scars, she can use multiple lasers. For a burn patient Waibel had, she used a 1550 nm laser and a 1927 nm NAFL and within 2 sessions the scarring looked more even. When doing these treatments, she works closely with reconstructive surgeons as they can work together to create the best treatment for the patient.
Not only cosmetic improvement can be made, but motion improvement can also be made according to Waibel and to keep in mind symptoms are sometimes what brings a patient in. She also learned that scars may be deeper than expected and have different depths are different levels.
“We have seen that the sooner you treat scars, and this is all scars, they melt away,” Waibel said. She stated laser treatments have a major role in trauma rehabilitation and give the physician power to heal patients and help alleviate suffering.
Disclosures:
Jill Waibel, MD, has done clinical trials for AbbVie, ArgenX, Cytrellis, Eli Lilly and Company, Lumenis, Lutronics, Michelson Diagnostics, Novartis, Pfizer, RegenX, Sciton, Syneron/Candela, and UCB. She has been on advisory boards for Cytrellis, Dominion Aesthetic Technologies, Sciton. A speaker for Eli Lilly and Company, Loreal, Novartis, and Syneron/Candela. Equipment from Michelson Diagnostics. She also discusses FDA off label uses.
Reference:
1. Waibel. J. Lasers As First Line of Therapy for Keloids and Other Scars - Pearls from the Expert. Presented at the: Skin of Color Update; September 10, 2021; Virtual.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.