- Dermatology Times, April 2022 (Vol. 43. No. 4)
- Volume 43
- Issue 4
- Pages: 50
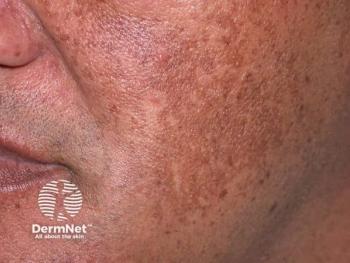
Identifying Diagnostic Bias in Skin of Color
Investigator Loren Krueger, MD, urges dermatologists to recognize and correct disparities in clinical decision-making, particularly regarding skin cancer.
Disparities in treating patients of color for dermatologic disorders extend beyond macro concerns such as accessibility and awareness to medical issues such as bias in clinical decision-making, according to research results presented at the 18th Annual Skin of Color Society Scientific Symposium held March 24, 2022, in Boston, Massachusetts.
In an exclusive interview with Dermatology Times®, lead abstract author Loren Krueger (LK), MD, assistant professor in the Department of Dermatology, associate program director, residency program, Emory University School of Medicine, Atlanta, Georgia, expanded on findings showcased in the abstract “Clinical Decision-Making Bias in Darker Skin Types: A Prospective Survey Study Identifying Diagnostic Bias in Decision to Biopsy.” The abstract catalogues disparities patients of color face in dermatologic care, especially regarding skin cancer and inflammatory disease diagnoses.
Krueger discussed these issues, including unmet needs among patients of color, and initiatives to increase physician diversity in the specialty in her conversation with Dermatology Times®.
What was the impetus for your research?
LK: We know that there are disparities in care for SOC [skin of color] populations, including those relating to skin cancers. Skin cancers may be diagnosed at later stages, and there is increased morbidity for SOC populations. We frequently attribute this to limitations in access to dermatologic care and a lack of awareness of risk. However, we must also understand that bias exists in medicine, and therefore we should know [and identify] any contributions we as dermatologists make to this disparity.
How did you design the study to investigate possible bias in clinical decision-making?
LK: There was no perfect way to design this study, but we wanted to know if background skin color plays a role in decision-making. We found images of dermatologic conditions in lighter skin and darker skin and asked dermatologists whether they would biopsy, as well as what they suspected the diagnosis would be. This study design allowed us to compare differences in dermatologists’ decision-making—to explain what those differences were.
What impact do these unneeded procedures have on patients and the health care system?
LK: Biopsies are relatively easy to perform in office and can be very helpful. Of course, we use biopsy when deemed necessary because there is an associated health care cost and a small scar that will develop. Unnecessary biopsies are burdensome to our health care system and our patients.
In your presentation, you noted that skin cancer is a special area of concern in terms of disparities in decisions such as whether to biopsy. What should dermatologists look for in presentation on skin of color to make a more accurate diagnosis?
LK: Early detection is key in skin cancer. Often, skin cancer presents differently in SOC patients—for example, in chronic ulcers or discoid lupus. As dermatologists, it is our duty to ensure an appropriate level of suspicion in these cases, even though they are not the typical presentation.
For SOC patients, it is important to note that squamous cell carcinoma [SCC] and basal cell carcinoma [BCC] may present as pigmented. Additionally, SCC is the most common type of skin cancer in Black patients and tends not to occur in sun-exposed areas. Chronic inflammatory or scarring processes have been estimated to account for 20% to 40% of SCC in this population. There is also a markedly higher metastatic potential in the setting of SCC secondary to chronic inflammatory or scarring. Asian patients also have a higher risk of SCCs due to chronic inflammation or scarring.
How can dermatologists raise awareness in SOC communities to help people recognize the early warning signs of skin cancer?
LK: You bring up a great point. SOC communities need more resources and education on warning signs. For example, there has been some effort to promote melanoma screening by hairdressers and nail technicians. Community engagement is key.
What did your research reveal about decision-making bias in inflammatory conditions such as atopic dermatitis (AD) and psoriasis?
LK: Our findings showed that participants were more likely to biopsy inflammatory skin conditions in SOC patients. Extrapolating, this may suggest that participants were less comfortable making a clinical diagnosis in background darker skin types and were therefore more likely to biopsy. This finding demonstrates our need for adequate training in all patient populations and phototypes.
Your presentation noted that “Black patients had 26% lower odds of receiving isotretinoin for acne and 42% lower odds of dupilumab [Dupixent; Sanofi and Regeneron Pharmaceuticals] for AD.” How much of that is the result of bias, and how much is a reflection of the drugs’ cost and availability, patients’ lack of awareness on when to consult a dermatologist, and dermatologists’ knowledge gap in diagnosing and treating these challenging conditions in patients of color?
LK: The [data cited] are key as evidence that disparities exist. The disparities are likely multifactorial. These findings demonstrate that there may be biases in decision-making regarding treatment for SOC patients.
Is telehealth an answer?
LK: Telehealth certainly has the potential to expand access in both rural and urban settings. Telehealth as a platform does not allow us to eliminate our biases, however. This study used photos, which are commonly the medium in telehealth, and clearly identified our biases.
How can the specialty start to bridge this gap in care? Does it start with medical school training?
LK: Absolutely! I have faith that our specialty is on the way to bridging the gaps, but first they must be identified. There are 2 aspects to address. First, we must make sure that our specialty is diverse and can address the unique needs of every community. This starts even earlier than medical school. We should increase youth interest in STEM [science, technology, engineering, and mathematics] and ensure that our pipeline to dermatology is as inclusive and as equitable as possible. Secondly, all dermatologists, regardless of race or ethnicity, should deliver quality care with cultural humility. Our medical school and residency curricula should reflect this aim.
How can practicing dermatologists learn to better recognize the different presentations of skin diseases on darker phototypes?
LK: Dermatology is such a visual specialty. Images and photos used for teaching should be diverse. Early exposure and training with dermatologists specializing in caring for minority populations and diseases that disproportionately affect minority populations should be available for all trainees. Ultimately, exposure is crucial.
Historically, medical school textbooks and photographic indices have failed to focus on providing diagnosis and manifestation examples for non-White skin. Is this improving?
LK: [It’s] definitely improving, but [there is] still work to be done. A great example of this was the dermatologic manifestations of COVID-19. Despite our field’s recognition that photographic representation of SOC is so important, when the literature on skin findings in COVID-19 was first published, there was a dramatic lack of images in SOC. This was despite the fact that COVID-19 disproportionately affected Black communities.
What other resources are available for physicians and medical students seeking to understand the presentation of skin cancer on people of color?
LK: These resources certainly exist, thankfully. For example, VisualDx [an online learning platform] is intentional about including images in SOC. Additionally,
Do you want to highlight any key points of the study for our readers?
LK: We all have personal and professional biases; that is simply fact. It is our duty to investigate, acknowledge, and attempt to mitigate our biases to provide the best care to our patients.
What should future studies investigate to improve this situation?
LK: We need more studies on bias as it relates to our diagnostic and therapeutic patterns. Our field should reflect on these to guide our training and future practice. Ultimately, to achieve health equity, we have to ensure that we as dermatologists are doing our part.
Disclosure:
Krueger disclosed no relevant conflicts.
Reference:
Krueger L. Clinical decision-making bias in darker skin types: a prospective survey study identifying diagnostic bias in decision to biopsy. Abstract presented at: 18th Skin of Color Society Scientific Symposium; March 24, 2022; Boston, MA.
Articles in this issue
almost 4 years ago
Microneedling Misconceptionsalmost 4 years ago
2022: Meeting the Challenges of Advanced BCCalmost 4 years ago
Cost of Copies Prompts a Lawsuitalmost 4 years ago
Diverse Perspectives in Medical Aesthetics Matter More Than Everalmost 4 years ago
Cellular Grafting in Vitiligoalmost 4 years ago
Polish Skills to Treat Nail Disordersalmost 4 years ago
Machine Learning to Identify Biomarkers in ADalmost 4 years ago
Effect of Joint Pain on Analgesic Use in Patients with Psoriasisalmost 4 years ago
Linking Psoriasis and Cardiometabolic DiseaseNewsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.