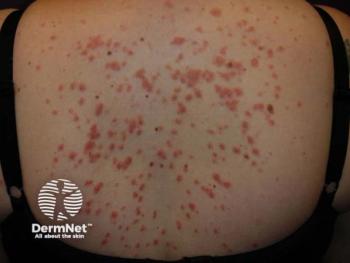
The connection between multiple sclerosis and psoriasis
Key Takeaways
- Patients with multiple sclerosis show increased incidence and prevalence of psoriasis, suggesting shared autoimmune mechanisms involving T helper cells and pro-inflammatory cytokines.
- The gut microbiome, genetic polymorphisms, and environmental factors like vitamin D deficiency and smoking may contribute to the pathogenesis of both conditions.
A meta-analysis of 43,643 patients with multiple sclerosis shows that these patients have an increased incidence and prevalence of psoriasis.
A meta-analysis of 43,643 patients with multiple sclerosis shows that these patients have an increased incidence and prevalence of psoriasis. The publication appeared online October 25 in the
The review highlights the challenges of managing multiple sclerosis in the context of its comorbidities and complications, specifically psoriasis, according to lead author Ching-Chi Chi, M.D., Chang Gung Memorial Hospital, Taiwan. "Medical specialists should be aware of the risk of developing psoriasis in patients with multiple sclerosis. Because both disorders are attributed to autoimmune mechanisms, we suggest that dermatology specialists may need not only neurology, but also rheumatology consultations. Further laboratory or imaging studies may be necessary for psoriatic patients in whom neurological symptoms appear," Chi and colleagues wrote.
Although the precise pathway leading to the concurrence of psoriasis and multiple sclerosis remains unclear, previous studies have focused on the immune system, environmental factors and genomics. The association between the two diseases may stem from the shared immune pathogenesis involving activation of T helper 1 (Th1) and Th17 cells, which lead to production of pro-inflammatory cytokines.
For multiple sclerosis, the proposed immunopathogenesis involves interferon-Æ´ and TNF factors, along with IL-17, -21, -22 and -26, which are produced by Th17 cells. All of these cytokines are crucial in the pathogenesis of psoriasis.
The gut microbiome has been implicated in the pathogenesis of both multiple sclerosis and psoriasis, as have genetic polymorphisms in HLA-DRB1 and IL-12B. Both pathways warrant additional exploration, the authors wrote.
Confirmed environmental triggers for multiple sclerosis include ultraviolet radiation exposure, Epstein-Barr virus, cigarette smoke and vitamin deficiency, but no evidence suggests that the foregoing environmental factors are also the predisposing factor for psoriasis. However, wrote Chi et al., they are related to psoriasis pathogenesis to some degree. "For instance, vitamin D deficiency can affect the proliferation of cells and immune response regulation. This might explain the increasing prevalence of multiple sclerosis with latitude."
Additionally, some reports state that vitamin D likely plays a key role in psoriasis pathogenesis. Although the real mechanism remains unclear, and it is tough to tell whether the relationship is direct or indirect, authors said, the shared vitamin D deficiency may partly explain the possible association between psoriasis and multiple sclerosis.
Previous studies have established strong evidence that Epstein-Barr virus is related to multiple sclerosis, although few studies have investigated the connection between Epstein-Barr virus and psoriasis. Investigators hypothesized that Epstein-Barr virus might induce cutaneous manifestations, as herpes simplex virus does, and these manifestations could result in the immunopathogenesis of psoriasis.
Cigarette smoke contains numerous toxic chemicals that induce inflammatory responses. "Smoking can produce free radicals and oxidative stress that damage the signal transduction pathway related to pathogenesis of psoriasis." Meanwhile, nicotine spurs production of proinflammatory cytokines such as IL-12 and TNF.
Meta-analysis of five case-control and four cross-sectional studies yielded a pooled odds ratio of 1.29 for prevalent psoriasis in patients with multiple sclerosis. From two cohort studies, investigators calculated that patients with multiple sclerosis had a pooled hazard ratio of 1.92 for psoriasis.
Two previous reviews investigating the link between multiple sclerosis and psoriasis showed inconsistent results. One, published in the July 2010
"By contrast," Chi et al. wrote, "we included more recent studies and separately analyzed data further according to different types of study design, thus providing robust evidence on the association of multiple sclerosis with psoriasis."
The fact that the meta-analysis included only two cohort studies made it difficult to explore the causal relationship between multiple sclerosis and psoriasis. Likewise, a lack of non-Caucasian studies may limit the generalizability of the study's findings. The analysis also excluded psoriasis subtypes and the impact of age, gender and disease severity.
Dermatologists in clinical practice may have to take pre-existing multiple sclerosis into account when managing psoriasis. "Nowadays, the commonly used medications for psoriasis include topical corticosteroids, keratolytic agents and immunomodulators." Few studies examine the effects of drugs on the association between the two diseases, the author wrote. "The hazard may therefore be underestimated. We recommend that clinicians be aware of this possibility. Furthermore, patients with psoriasis and a family history of multiple sclerosis should be referred to neurologists for multiple sclerosis screening, and vice versa."
REFERENCE
Chia-Yu Liu, Tao-Hsin Tung PhD, Chin-Yu Lee, Kuo-Hsuan Chang MD, PhD, Shu-Hui Wang MD, MS, Ching-Chi Chi MD, DPhil. "Association of Multiple Sclerosis with Psoriasis: a Systematic Review and Meta-Analysis of Observational Studies,"
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.