Case Report: Efficacy of Dupilumab for Acquired Reactive Perforating Collagenosis Associated with Atopic Dermatitis
A new report delves into the case of a 35-year-old man with ARPC and why dupilumab was utilized for treatment.
Acquired reactive perforating collagenosis (ARPC) is a rare dermatological condition characterized by the transepidermal elimination of abnormal connective tissue, such as collagen and elastin. Typically manifesting in adults, ARPC is commonly associated with systemic diseases where pruritus is a prevalent symptom, such as diabetes mellitus and chronic kidney disease. Less frequently, ARPC has been linked to chronic inflammatory skin disorders like eczema and psoriasis. The itch-scratch cycle plays a critical role in the pathogenesis of ARPC lesions, emphasizing the importance of anti-pruritic therapies in managing this condition. A new case study published in
Case Presentation
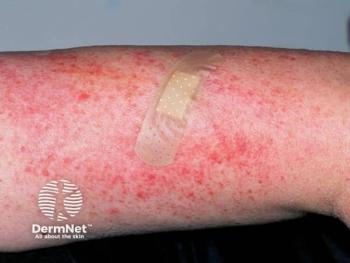
Investigators highlighted the case of a 35-year-old man who presented with a 12-month history of pruritic, chronic-relapsing skin lesions on the trunk and limbs. The patient’s medical history included an arteriovenous malformation involving the meninges and glaucoma, with a noted history of childhood food allergies. Physical examination revealed numerous erythematous-scaling patches with eczematous features and excoriations, intermingled with multiple papules and nodules characterized by central keratotic plugs symmetrically distributed on the trunk and lower extremities.
Blood tests, including eosinophil count and total IgE levels, were within normal limits, and patch tests were negative. Histopathologic examination of a skin biopsy confirmed chronic eczema, while a nodule biopsy showed epidermal necrosis with extruded collagen and elastic fibers. This led to a diagnosis of ARPC associated with severe atopic dermatitis (AD).
Initial systemic treatment with cyclosporine provided clinical improvement but had to be discontinued due to adverse effects, including dyslipidemia, altered liver enzyme levels, and hypertension. Subsequently, the patient was treated with dupilumab at the approved dose for AD. Notably, the patient reported “marked relief from itching,” with an itch numeric rating scale score decreasing from 9 to 2 after one month of treatment. Significant clearance of lesions was achieved after twelve weeks, although some postinflammatory hyperpigmented macules and erythematous patches persisted.
Discussion
Management of ARPC primarily focuses on alleviating pruritus and addressing associated comorbidities. In mild cases, topical steroids, antihistamines, and moisturizers are commonly used. Severe cases may require systemic treatments such as steroids, retinoids, tetracyclines, phototherapy, dapsone, methotrexate, and allopurinol.2-3
In this case, the severe itch related to AD likely contributed to the development of ARPC lesions, which appear to be a reactive response to chronic scratching and repetitive trauma. Chronic pruritus in AD is predominantly driven by Th2 cytokines, particularly interleukin (IL)-4 and IL-13, which act on itch sensory neurons and enhance neural hypersensitivity to various pruritogens.4
Dupilumab, a monoclonal antibody inhibiting IL-4 and IL-13 signaling, has proven effective in treating moderate to severe AD and other pruritic skin disorders, including prurigo nodularis, bullous pemphigoid, lichen planus, and pruritus sine materia. Recent reports have also highlighted dupilumab's efficacy in treating ARPC, both associated with and independent of AD. One study emphasizes that "chronic pruritus in atopic dermatitis is known to be driven by type 2 cytokines, including IL-4 and IL-13, and dupilumab... has been shown to be effective in the treatment of moderate to severe atopic dermatitis as well as other type 2-driven pruritic dermatological conditions."5
Given dupilumab's safety profile, even in patients with multiple comorbidities, investigators wrote that it represents a promising treatment option for severe ARPC-associated itching. This case supports the potential use of dupilumab for ARPC, expanding its therapeutic indications and providing relief for patients suffering from this challenging condition. As noted in the study, "this case supports the potential use of dupilumab for the treatment of reactive perforating dermatosis," highlighting its potential in managing ARPC associated with severe AD.1
Further research and clinical trials are warranted to establish dupilumab as a standard treatment for ARPC and other pruritic dermatoses. Investigators concluded, “Considering the safety profile of dupilumab also demonstrated in frail patients affected by multiple comorbidities, including diabetic and kidney failure, it could be a valuable potential treatment option for severe ARPC-associated itching.”1
References
- Gori N, De Luca E, Chiricozzi A, Sfregola S, Di Stefani A, Peris K. Successful Use of Dupilumab in the Treatment of Acquired Perforating Dermatosis Associated with Atopic Dermatitis. Case Rep Dermatol Med. 2024;2024:6265608. Published 2024 Jun 19. doi:10.1155/2024/6265608
- Garrido PM, Queirós C, Borges-Costa J, Soares-Almeida L, Filipe P. Acquired perforating dermatosis: clinicopathologic study of a 10-year period at a tertiary teaching hospital. Int J Dermatol. 2020;59(4):445-450. doi:10.1111/ijd.14760
- Gori N, Di Stefani A, De Luca EV, Peris K. A case of disseminated perforating necrobiosis lipoidica. Clin Case Rep. 2020;8(5):808-810. Published 2020 Mar 27. doi:10.1002/ccr3.2766
- Erickson S, Heul AV, Kim BS. New and emerging treatments for inflammatory itch. Ann Allergy Asthma Immunol. 2021;126(1):13-20. doi:10.1016/j.anai.2020.05.028
- Napolitano M, Di Guida A, Nocerino M, Fabbrocini G, Patruno C. The emerging role of dupilumab in dermatological indications. Expert Opin Biol Ther. 2021;21(11):1461-1471. doi:10.1080/14712598.2021.1907341