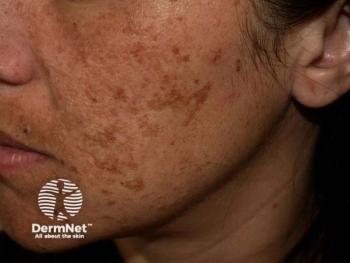
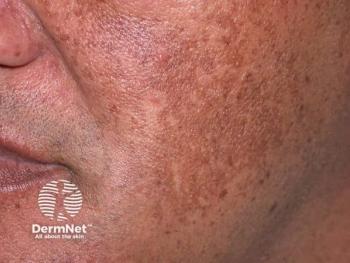
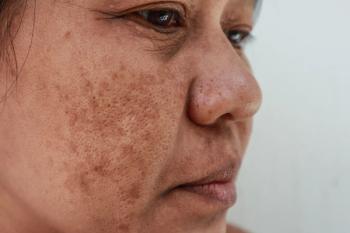
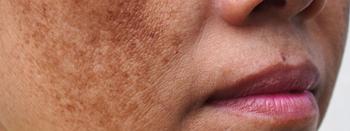
Antioxidant drug promising for melasma
Silymarin, derived from milk thistle, could offer the same level of treatment efficacy for melasma with more benefits for patients than the most widely-used therapy, hydroquinone.
Silymarin, an antioxidant drug, could offer the same level of treatment efficacy for melasma with more benefits for patients than the most widely-used therapy, hydroquinone.
A
This study is the first to directly compare the efficacy and impact of both medications.
Clinically,
Consequently, according to investigators, there’s a need to identify other treatment options that offer patients improvement without deleterious effects.
“We hope these results would encourage the wide use of silymarin in the treatment of melasma and, consequently, allow a new important substitute for those who complained from this psychologically distressing disorder,” said lead author Ahmad Nofal, M.D., a dermatologist on the faculty of medicine at Zagazig University in Egypt.
Derived from milk thistle, silymarin’s main component is the antioxidant silibinin, but its exact mode-of-action hasn’t yet been identified. It has been shown to decrease the dangerous effects of solar ultraviolet radiation, including oxidative stress, inflammation, edema, erythema, DNA damage and immune responses. Additionally, in a dose-dependent way, it can prevent melanin production without impacting cell viability.
In contrast, the more widely-used hydroquinone inhibits melanogensis by stymieing the tyrosianse enzyme. It affects how melanomas form, melanize and degrade, and it modulates melanocytes’ membranous structures, leading to whole melanocyte necrosis.
To test how silymarin compared as a possible treatment option, investigators divided 42 female participants into three groups. Each group contained 14 patients. Group 1 received a twice-daily 0.7% silymarin cream regimen. Group 2 was treated with twice-daily 1.4% silymarin cream, and Group 3 was treated with once-daily 4% hydroquinone cream. The study lasted three months, and patients were instructed to avoid excessive sun exposure and apply sunscreen of at least SPF 50.
According to study results, all patients experience roughly the same level of melasma improvement. Group 1 began with mean MASI scores of 18.56 +/- 5.58. Throughout treatment, the scores steadily fell: 13.94 +/- 4.92 at one month, 12.62 +/- 4.76 at two months, and 10.96 +/- at three months. Overall patients saw a melasma reduction of 39.21 percent +/- 20.65. Group 2, with a beginning mean MASI of 21.75 +/- 8.47, saw a drop to 17.39 +/- 8.07 at one month, 15.6 +/- 7.92 at two months, and 14.88 +/- 7.79 at three months. The final percent reduction was 33.84 +/- 15.61.
Results were statistically similar for Group 3. Participants began with a mean MASI score of 16.64 +/- 9.0. After one month, it fell to 12.25 +/- 6.94, and it dropped to 10.82 +/- 7.10 at two months. By month three, their MASI scores reduced to 8.81 +/- 5.68, totaling a 46.75 percent reduction +/- 22.83.
The difference between the medications emerged when investigators examined the occurrence of side effects. They found hydroquinone caused frequent, significant side effects. In this current study, researchers reported, 71.4 percent of hydroquinone recipients (10 individuals) experienced erythema. Burning and scaling also each occurred in the same number of patients.
Conversely, according to data analysis, participants treated with silymarin experienced no negative side effects.
“The absence of adverse effects in the patients treated with silymarin represents an important advantage of silymarin over the conventional hydroquinone that is commonly associated with adverse effects,” the authors wrote. “This indicates that silymarin might serve as an effective and safe modality for the treatment of melasma.”
Additionally, the relapse rate between the two treatments was different. Only one patient (7.14 percent) in both silymarin groups (Groups 1 and 2) experienced a relapse after six months. However, three patients (21.4 percent) in the hydroquinone group relapsed during the same follow-up period.
Based on these results, the authors recommended further research, but they concluded topical silymarin could be a good option for patients who encounter unwanted side effects with hydroquinone.
Reference:
Gamal N, Ibrahim A, Nofal A, Nofal E, Osman S, Topical silymarin versus hydroquinone in the treatment of melasma: A comparative study, Journal of Cosmetic Dermatology (2018); doi: 10.1111/jocd.12769