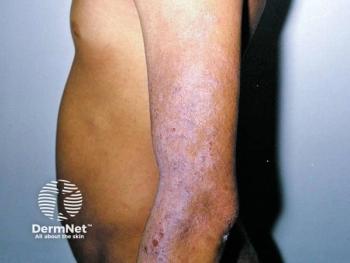
Skin cancer and the immunosuppressed patient
National report — The threats of skin cancer and bad outcomes from the disease are significantly higher for those who are immunosuppressed than they are in the general population.
National report - The threats of skin cancer and bad outcomes from the disease are significantly higher for those who are immunosuppressed than they are in the general population.
The increase in skin cancer risk for immunosuppressed patients varies depending on the population. It can range from a small increase with the administration of systemic steroids to a dramatic increase - up to 64-fold - with transplant-associated immunosuppression, according to Clark C. Otley, M.D., a dermatologist and associate professor of dermatology at the Mayo Clinic, Rochester, Minn.
Dermatologists play an important role in taking extra precautions with these patients, who include transplant and HIV patients. Among dermatologists' options, Dr. Otley says, are to aggressively pursue traditional preventive and treatment options, as well as work closely with the specialists treating these patients to modify drug regimens and enhance immunity.
Skin cancer is the most prominent of cancers among transplant patients.
"About 50 percent of the cancers that develop in our transplant patients are skin cancers, which outnumbers all the other cancers combined," Dr. Otley says. "That is because our immunity probably fights cancer development; we also know that some of the immunosuppressant medications may contribute to cancer formation."
Researchers who have injected cyclosporin into a particular kind of mouse, called a SCID, and exposed these mice to ultraviolet radiation have found the mice develop cancer at an increased rate. That is, even though they do not have an intact immune system, suggesting that there might be a carcinogenic effect, according to Dr. Otley.
One way to help transplant patients avoid skin cancer is to modify their use of medicines that could cause the cancer.
"There are about eight lines of evidence suggesting that reduction of immunosuppression may be an effective adjuvant modality that could reduce the risk of skin cancer in the transplant patients. However, a randomized prospective trial for this specific indication is yet to be done," Dr. Otley says.
It is likely that many transplant patients on immunosuppressant therapy are on higher doses of medication than they need to be to optimize their kidney, heart or liver function, according to Dr. Otley.
Dantal J. et al conducted a randomized trial where patients received either high-dose or low-dose cyclosporin one year after kidney transplantation and found that while there was increased risk of rejection, it was manageable rejection. At the trial's end, patients did not have any permanent detrimental effects on their organs and developed fewer cancers, including fewer skin cancers, according to Dr. Otley.
Another strategy is to consider switching patients to a relatively new immunosuppressant called sirolimus, or rapamycin.
"There is early epidemiologic data that suggests that rapamycin might be associated with a lower risk of skin cancer," he says. "It is important to emphasize, however, that modifying immunosuppressant therapy is not something that dermatologists do. This is something that we talk with the transplant physicians and ask them to consider. We, however, know how bad the skin cancer is and it is the dermatologist's job to identify the risk of skin cancer, think about how risky it will be in the future and then talk to the transplant physician when we feel like it is warranted to reduce the immunosuppression."
In addition to consulting with patients' physicians about modifying their drug regimens, dermatologists would recommend that patients use vigorous sun protection, with sunscreen and protective clothing. Dermatologists, according to Dr. Otley, should treat any skin cancers aggressively and consider using a variety of chemotherapy and preventive cream treatments.
HIV-related challenges
Since the development of highly active antiretroviral therapy (HAART), HIV patients have enjoyed longer lives. The resulting immunosuppression, however, has been associated with elevated risks for a variety of cancers, including skin cancers, lymphomas, anal cancers, head and neck cancers, myelomas, germ cell tumors, lung cancers and leukemia, according to Dr. Otley.
"In one study, researchers discovered that if you have HIV-associated Kaposi's sarcoma, you respond better to HAART plus a pegylated liposomal form of doxorubicin, which is chemotherapy, than you do just with the administration of the highly active antiretroviral therapy," he says.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.