Seeing is believing
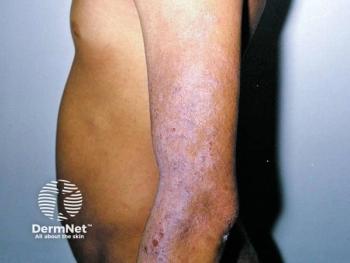
The severe hyperpigmentation began at 2 weeks of age and continued until 8 years of age, when the pigment began to disappear leaving behind a light-brown colored skin and numerous lentigines.
Mexico City, Mexico - Even though most dermatologists would agree that the majority of dermatologic cases seen in private practice or in clinic are clear cut and straight forward, in terms of diagnosis, every now and then they are highly challenged and confronted with extremely peculiar cases - patients presenting with a constellation of symptoms not seen in literature and less spoken of in academic circles.
Ramon Ruiz-Maldonado, M.D., professor of the department of dermatology and pediatric dermatology at the University of Mexico and National Institute of Pediatrics in Mexico City, Mexico, discusses six such unusual cases.
Case 1: Universal acquired melanosis
The severe hyperpigmentation began at 2 weeks of age and continued until 8 years of age, when the pigment began to disappear leaving behind a light-brown colored skin and numerous lentigines. Family members had a light brown skin color and Caucasoid anthropomorphic features.
Dr. Ruiz-Maldonado says that excessive amounts of melanin were seen in all epidermal layers on skin biopsy and electron microscopic examination showed normal melanocytes with increased numbers of melanosomes two, three and four. The patient died at age 26 of a colonic adenocarcinoma.
Case 2: Multiple scalp whorl syndrome and associated anomalies
According to Dr. Ruiz-Maldonado, this previously unreported syndrome involved a 13-month-old male infant with no less than 14 hair whorls in the scalp.
The patient had sparse frontal hair, a wide forehead, ectropion, abnormal implantation of the eyelashes, peculiar hair, as well as a depigmentation of the nipples.
"Over 90 percent of individuals have just one whorl, less than 5 percent have two whorls, and to have three whorls is regarded as exceptional. The association of multiple hair whorl formation, brain development and other unusual anomalies, begs the question of further studies and developmental explanations," he says.
Case 3: Edematous scarring vasculitic panniculitis (ESVP)
"Classic" hydroa vacciniform is characterized by seasonal light-induced vesicles that evolve into crusts and leave behind varicelliform scars.
Patients are in a good general health and spontaneous resolution of lesions in adolescence to early adulthood is the norm.
"Our clinic described 14 pediatric cases of a severe condition characterized by marked facial and hand edema, as well as large vesicles and crusts that leave behind varioliform scars and tissue loss. Patients suffer from wasting, failure to thrive, hepatosplenomegaly, insect bite hypersensitivity, frequent development of Epstein-Barr virus associated malignant NK/T cell lymphoma, as well as lobar and septal panniculitis, vasculitis and perineuritis," Dr. Ruiz-Maldonado tells Dermatology Times.
He says that this multisystemic disease with malignant potential has significant differences from the classic hydroa and suggested that the severe disease form be considered a separate disease entity.
Case 4 : Intrauterine epidermal necrosis
Dr. Ruiz-Maldonado described the clinical picture of three premature, female newborns suffering from congenital, excessive skin necrosis, sparing only the scalp, face, hands, feet, elbows and knees, with normal mucous membranes.
Two of the infants were dizygotic twins and all three patients died 72 hours postpartum. He says that the histopathology of the epidermis adjacent to the denuded dermis suggested an apoptotic process.
"This condition may be genetically determined in an autosomal recessive form. The differential diagnoses can include extensive aplasia cutis congenita, Herlitz type epidermolysis bullosa, toxic epidermal necrolysis, acute graft-versus host reaction and congenital erosive and vesicular dermatosis," Dr. Ruiz-Maldonado says.
Case 5: Desmoplastic hairless, hypopigmented nevus
Dr. Ruiz-Maldonado reports this variant of giant congenital melanocytic nevus (GCMN) in four of 143 pediatric cases of 143 GCMN.
Patients presented with hard, progressively hypopigmented and alopecic giant congenital melanocytic nevi, with severe, refractory pruritus seen in two patients.
All four patients showed intense dermal fibrosis, scarce nevus cells and hypotrophic or absent hair follicles on section. Dr. Ruiz-Maldonado notes that there was no evidence of malignant transformation and that the fibrosis could have been due to an immune reaction to the nevus cells.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.