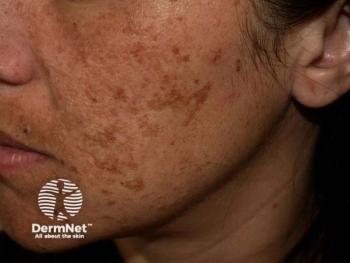
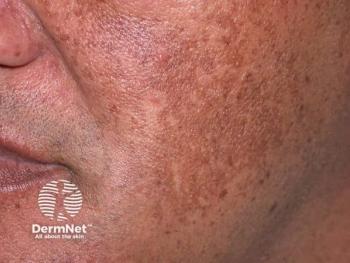
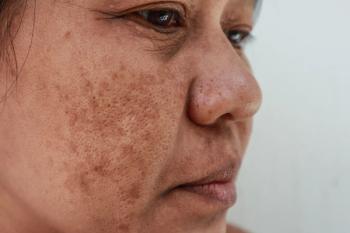
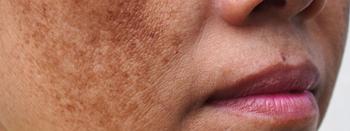
A review of lasers for hyperpigmentation
Researchers recently discussed laser and IPLS options for a variety of pigmentary conditions, and provided their recommendations for each one in this review published in European Academy of Dermatology and Venerelogy.
Conventionally, lasers and intense pulsed light sources (IPLS) are considered go-to treatments for various pigmentary disorders. But not every laser therapy works for every condition.
In a
“A complete review of the existing data and a consensus statement by experts in the field was highly needed to help physicians to provide optimal care of these lesions,” said Thierry Passeron, M.D., Ph.D., dermatology professor at the University of Nice Sophia Antipolis.
Initiated by the European Society for Laser in Dermatology, the statement outlines laser recommendations and efficacy for these conditions.
Overall, researchers discussed treatment options for 16 pigmentary disorders. These are their recommendations.
Actinic lentigos: Use ultrashort Q-switched nanosecond/picosecond laser treatment to treat a small number of actinic lentigos lesions. One or two sessions can completely remove the benign, flat lesions caused by acute, prolonged, unprotected sun exposure.
Lentil simplex and lentiginosis: Treat lentigos simplex with QS lasers, such as QSNY, QSAL, and QS ruby, to target melanin with nanosecond pulses. Results are favorable, and recurrence is low, investigators said. If numerous lesions are present, rule out a syndromic association before treating.
Ephelides: A 532nm QS laser can treat ephelides’ high pheomelanin content, but recurrence is inevitable. Laser treatment isn’t highly indicated. Recommend regular sunscreen use instead.
Café au lait spots: Laser treatment isn’t recommended. Recurrence within a few months is high, and hypopigmentation is a common side-effect.
Linear and whorled hypermelanosis: Few treatments exist, but QS lasers appear effective after only one or two sessions, researchers said. Caution patients recurrences are possible, requiring additional treatments.
Naevus spilus (NS): Use QS lasers to treat macules or papules accompanying these lesions. Macular NS responds better to treatment than papular, but recurrences aren’t infrequent.
Becker’s naevus (BN): Management is highly variable, and removal carries scarring and dyspigmentation risks. Long-pulsed laser effectively removed BN-associated hair, but its less efficacious in hyperpigmentation treatment. Investigators suggest advising against treatment because results aren’t predictable and recurrence is high.
Dermal hypermelanocytosis, Ota, Ito naevus: The 1064nm QS laser is the gold standard for Ota and Ito naevus therapy. Pain, swelling, and pinpoint bleeding are possible. Consequently, researchers recommend at least two months between sessions to minimize scarring risk.
Acquired dermal melanocyotsis, including ABNOM: Use the 1064nm QS laser for treatment. Verify the diagnosis, however, because this condition doesn’t respond to blanching agents or peelings.
Congenital nevomelanocytic nevi (CNN): QS and LP pigment-specific lasers and fractional lasers can improve a patient’s cosmetic appearance, but they don’t eliminate the malignancy risk associated with bigger, more numerous CNNs. Therefore, discuss laser options among other therapeutic options.
Postinflammatory hyperpigmentation: This acquired condition can negatively impact patients’ lives, but, eventually, laser treatment can provide improvement. However, as it can induce or worsen the condition, test small areas before treating the entire lesion.
Melasma: Kligman’s formula is the gold standard treatment for this highly complex hyperpigmentary disorder, but lasers can effectively target melasma’s vascular component, investigators said. Still, consider it only if topical depigmenting agents and peelings fail because relapses and worsening can occur.
Drug-induced non-melanin pigment: QS lasers are preferred for clearing these hyperpigmentations caused by drugs or metallic salts. Advise patients to stop using these agents when possible.
Exogenous ochronosis: These discolorations are difficult to treat. Use multiple QS laser and/or fractional ablative laser treatments, coupled with high SPF sunscreen protection, to provide improvement.
Siderosis and hemosiderosis: Little data is available on treating these iron deposits, but evidence shows fewer than three sessions with a 532nm QS laser appears to be effective.
Pigmented seborrhoeic keratosis and dermatosis papulosa: Good efficacy and safety results indicate a 1064nm LP Nd-YAG laser and ablative erbium laser can be added to the cadre of treatments for dermatosis papulosa nigra.
Overall, Passeron said, clinicians must remember not all devices and therapeutic approaches are effective or appropriate for all conditions. They must be careful to identify the correct diagnosis before prescribing treatment.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.