Researchers Explore WIHN in Mice and Humans
Researchers assessed the function of skin bacteria in wound healing and wound-induced hair follicle neogenesis (WIHN), a rare adult organogenesis model.
Researchers at Johns Hopkins School of Medicine have been studying a phenomenon in mice involving wounds, where at the center of a wound they make a new hair follicle as they did when they were embryos—but that normally doesn’t happen as adults.
That led to a study, “Bacteria induce skin regeneration via IL-1b signaling,”1 where researchers assessed the function of skin bacteria in wound healing and wound-induced hair follicle neogenesis (WIHN), a rare adult organogenesis model.
“That process is really exciting and we were really curious about what induces that and what controls that,” says Luis Garza, MD, PhD, professor at the department of dermatology at Johns Hopkins School of Medicine, who served as lead author of the study. “This could teach us how to deal with burn scars or maybe even eventually growing a limb, because limbs and hair follicles have a lot of overlapping biologies.”
Therefore, studying WHIN is something that could make a big difference in the future of wound care.
Garza explains that WIHN levels and stem cell markers correlate with bacterial counts, being lowest in germ-free, intermediate in conventional specific pathogen-free, and at its highest in wildtype mice, even those infected with pathogenic Staphylococcus aureus.
“When we looked at gene signatures of what genes are being turned off and on, in multiple contexts, we saw mice that had good regeneration had a genetic signature that overlapped that when you have a staff aureus infection,” he says. “We thought that was kind of weird, so we sought out to test what could be the role of bacteria in wound healing and regeneration.”
Today, environmental factors that enhance regeneration are largely unknown. The immune system and microbiome are attributed roles in repairing and regenerating structure, but their precise interplay has always been unclear.
During the study, decreasing skin microbiota via cage changes or topical antibiotics lowered WIHN. Therefore, inflammatory cytokine IL-1b and keratinocyte-dependent IL-1R-MyD88 signaling are necessary and sufficient for bacteria to promote regeneration.
“We tested a bunch of different conditions—comparing standard laboratory mice in our medical school to germ-free mice grown in a bubble,” Garza says. “We did wounds on them and compared how well they regenerated. We found the standard mice regenerated much better than the ones that weren’t exposed to any bacteria at all.”
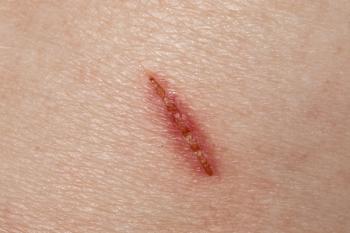
That led to a small trial on humans, where a topical broad-spectrum antibiotic slowed skin wound healing in adult volunteers, demonstrating a role for IL-1b to control morphogenesis and support the need to reconsider routine applications of topical prophylactic antibiotics as well.
“We did identical punch wounds on the back of people’s legs and for one group, we told them to use Vaseline, and the other, we told to use Neosporin, and the one that got Neosporin, healed slower,” Garza says. “We saw wound healing speed changes in the mice also, so bacteria not only helped regeneration in the mice, but also helped regeneration speed in people.”
The researchers concluded that people should not use Neosporin for wounds when healthy; that by understanding how these bacteria are acting, it may lead to the development of new and better therapies; and that they could more safely identify specific elements that are being turned on by bacteria and given those instead.
Reference:
1. Wang G, Sweren E, Liu H, et al. Bacteria induce skin regeneration via IL-1β signaling. Cell Host Microbe. 2021;29(5):777-791.e6. doi:10.1016/j.chom.2021.03.003
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.