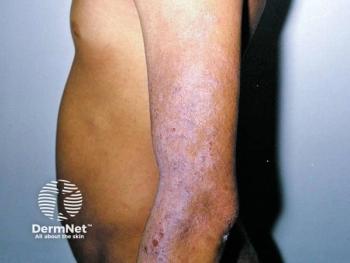
Port wine stain strategies
Vascular laser surgery for port wine stains has led the way in pediatric dermatology surgery and can significantly improve the condition. The period from six to 18 months offers a good window for treatment.
"I really believe that when you look at specialty pediatric dermatology, it was vascular lasers that moved the field into dermatologic surgery, setting up a great number of patients who are undergoing a large set of procedures, many of which are performed under general anesthesia or sedation," Dr. Eichenfield says.
While the laser procedure is good at reducing the coloration of port wine stain, most patients will see residual coloration.
Standard still subpar
The pulsed dye laser is considered to be the standard of treatment, with initial lasers generating a wavelength of 585 nanometers and newer equipment at 585 to 595 nanometers.
Larger-diameter vasculature tends to respond better to the higher wavelength. There is some variability among patients in response to both wavelengths and no good predictor as to which will be better for an individual patient.
Pulse durations generally range from 450 to 1,500 microseconds.
Dr. Eichenfield tells Dermatology Times that after six to eight treatments, many physicians "start to change the parameters to see if they can get any more lightening in the area."
It appears that 30 percent to 50 percent of all children who undergo treatment for port wine stains have either a recurrence or darkening of the site over time. However, there are limited studies on this phenomenon.
Options in treating stubborn port wine stains include increasing the wavelength, higher fluences, higher fluences with cryogen cooling - as a way to minimize epidermal damage - overlap of treatment areas and increased central venous pressure as a way to increase blood flow to the skin to generate more of a vascular target.
Managing recalcitrant stains
Refractory port wine stains and hypertrophic port wine stains remain problematic for practitioners.
The 1,064 Nd:YAG laser has been used on some patients with good results, but its utilization in pediatric patients is still quite limited.
Dr. Eichenfield prefers to defer treatment during the first few months of life. He generally initiates treatment at about 4 to 6 months, with the goal of completing six to eight treatments by 18 to 24 months of age.
"The safety of anesthesia is equivalent at any age beyond a few months of life, and the treatments and postoperative purpura do not disrupt a young child's life very much, unlike treating an older child or adolescent. The first two years of life may be a window of opportunity where the parents are conscious of the intervention, but the children may not be," which can be an attractive reason to address the situation early, Dr. Eichenfield notes.
He says lasers are not considered to be the primary tool in treating hemangiomas, though they can be effective in treating remnant hemangioma and ulcerated hemangiomas.
"But only consider laser with trepidation for rapidly proliferating and extrasuperficial or deep lesions," he warns.
The skinny on sedation
The trend is to use general anesthesia or unconscious sedation for elective pediatric surgery that cannot be accomplished with the patient awake, with or without topical and local injection anesthetics.
The Food and Drug Administration (FDA) recently ordered five companies to stop compounding topical anesthetic creams because the agents were linked to seizures, irregular heartbeats and two deaths, Dr. Eichenfield notes.
He speculates, "It is probably the mixture of agents - lidocaine, petracaine, benzocaine and primacaine - and this risk is clearly greater in small children."
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.