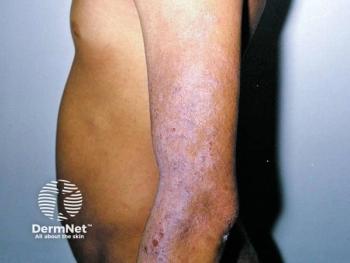
Pediatric scar treatments
EAST POINT, Georgia – According to the literature, new treatments for keloids and hypertrophic scars include intralesional interferon, 5-FU, doxorubicin, bleomycin, verapamil, retinoic acid, imiquimod 5 percent cream, tacrolimus, tamoxifen, botulinum toxin, TGF-beta3 and rhIL-10. Unfortunately, none of these treatments have been proven to be safe in the pediatric population. A growing body of evidence suggests, however, that imiquimod 5 percent cream is an effective and appropriate treatment for hypertrophic scars and keloids after surgery or trauma in pediatric patients.
Key Points
East Point, Ga. - A growing body of anecdotal evidence suggests that imiquimod 5 percent cream is an effective and appropriate treatment for hypertrophic scars and keloids after surgery or trauma in pediatric patients.
Atlanta dermatologist Terry L. Sharpe, M.D., takes the use of this versatile immune response modifier a step further in her pediatric patients, with preventative application in those who are prone to hypertrophic scar and keloid formation.
"In children with strong family histories of keloids, or in children who are having procedures in keloid-prone areas such as the chest or ears, I recommend using Aldara (imiquimod, Graceway) prophylactically," Dr. Sharpe says.
Topical therapies, such as imiquimod, have become increasingly popular for hypertrophic scar and keloid treatment and prevention because of their ease of use, noninvasive nature and relatively low cost in comparison to other options.
In one recent study, 13 keloids (in adult patients) were treated with excision in combination with nightly applications of imiquimod 5 percent cream for eight weeks. Ten patients with 11 keloids completed the six-month study, and no keloids recurred after six months.
Patients experienced mild irritation with the application of imiquimod, and some needed a break from the medication. More than half of the patients experienced hyperpigmentation.
"I often treat children with imiquimod after a procedure or injury," Dr. Sharpe says. "My regimen is three times a week for eight weeks, and this regimen does seem to prevent keloid formation."
The downside, however, is that imiquimod can be irritating in some patients, causing redness, scaling and pruritis.
Conventional treatments on which Dr. Sharpe continues to rely for scars and keloids in her pediatric patients include Cordran tape (flurandrenolide, USP), silicone gel, intralesional Kenalog (triamcinolone, Bristol-Myers Squibb), liquid nitrogen and pressure earrings.
"I often treat with Cordran tape, which is applied to the affected area at bedtime," Dr. Sharpe says. "The children sleep in it, and it usually leads to softening of the keloid. It can also be used for prevention after a surgical procedure, and it tends to reduce the incidence and extent of pruritis."
Dr. Sharpe stresses that when treating children, the least painful option possible is the best choice. Silicone gel fits the bill, she says.
"There are some reports that the silicon makes the hypertrophic scars and keloids more pliable; however, I do not see a complete flattening with silicon, unless the lesion is very new and thin - but it is painless," she says.
Another painless option is pressure earrings, which are particularly effective for preventing keloids after surgery on the ear.
"This is painless and can be combined with Cordran tape, intralesional injections or Aldara," Dr. Sharpe says.
In older, "motivated" children, Dr. Sharpe sometimes opts for intralesional Kenalog of between 6 mg and 40 mg, depending on the thickness and location of the keloid. She avoids this treatment completely in younger children, and uses the lower strength in darkly pigmented children, because, she says, higher doses can result in unsightly hypopigmentation.
She sometimes uses Intron A (interferon alfa-2b, Schering) injections as well, but much less frequently than in years past, she says, because of the expense associated with them.
If the patient is fairer in complexion, Dr. Sharpe says liquid nitrogen is a viable treatment option.
"This is probably more acceptable now that there are over-the-counter wart treatments based on this premise," she says.
Adult patients who have keloids may be treated with radiation therapy. Dr. Sharpe says she does not opt for radiation treatment for scars or keloids in pediatric patients because of the potential long-term side effects.
"There is a theoretical concern for the development of squamous cell cancers in the area of previous radiation therapy," she says.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.