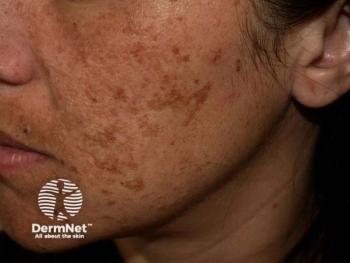
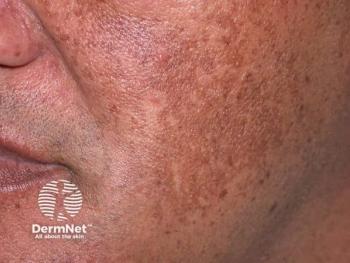
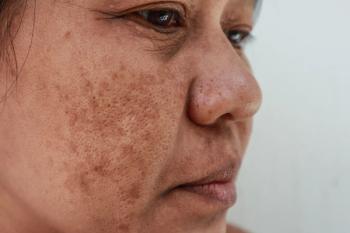
Melasma treatment possibilities expand thanks to new research
New research has shed light on how hyperpigmentation occurs. Experts break down what you need to know in this article.
Historically, melasma has been a difficult-to-treat condition, confounded by hard-to-avoid sun exposure and characterized by flare rebounds. Recent research, though, is shedding light on how the hyperpigmentation occurs, clueing dermatologists into potential new treatment avenues.
Having a better understanding of what might cause the condition and being able to recognize it can help providers give patients the highest level of care possible, meeting their physical and mental needs.
“We know melasma is a therapeutically challenging condition because when you cease to treat it - or even during treatment - there can almost be a universal relapse with the current tools we have in our toolbox,” says Pearl Grimes, M.D., director of the Vitiligo and Pigmentation Institute of Southern California. “Ideally, we’d love to find something we can use to clear up the patient and get them in a sustained state of remission, but we’re not there yet.”
Still, she says, new data surrounding melasma is launching dermatology in the right direction.
THE PATHOGENESIS OF MELASMA
Sunlight is known to be a major player in melasma with ultraviolet light being a significant trigger, she says. But, new data also points to a role for visible light, particularly low-spectrum blue light. By activating the exon 3 pathway on melanocytes, visible light triggers the dopachrome complex responsible for the sustained hyperpigmentation of melasma.
But, there’s more at play than sunlight exposure, says Seemal Desai, M.D., president of the Skin of Color Society.
“There is a good amount of data now that talks about melasma as almost an inflammatory skin condition,” Dr. Desai says, who is also the president and medical director for Innovative Dermatology in Plano, Texas. “It’s one of those things where we also want to mention to patients who have melasma that there is a vascular component to the disease.”
This increased vascularity causes blood vessel dilation. Different from what is usually associated with rosacea, he says, this vascularity appears to be mediated by mast cells. They degranulate chemokines, such as histamines and other proteins. Over time, that degranulation causes damage to the epidermal-dermal basement membrane junction, the area of tissues connecting the epidermal and dermal skin layers.
Other blood vessel markers, such as vascular endothelial growth factor, are found in higher levels in melasma-affected skin versus unaffected skin, Dr. Grimes says.
“When you look at these changes that have been identified, it suggests melasma probably represents a phenotype of photodamage,” she says. “It creates a paradigm shift in how we treat it.”
In addition to sunlight and vascular involvement, recent research also points to pollution as being a potential factor in melasma development, says Arianne Kourosh, M.D., MPH, a pigmentary disorder specialist at Massachusetts General Hospital.
“In urban settings, pollution could also damage the skin and give rise to hyperpigmentation,” she says. “This is important because it’s an external factor that might give rise to melasma or worsen it.”
Research published in the Journal of Drugs in Dermatology revealed airborne particulate matter and polycyclic aromatic hydrocarbons can enter the skin and create quinones that produce reactive oxygen species that lead to skin pigmentation.1 The results also highlight increased rates of melasma among patients with skin types III-VI in areas with documented high pollution levels, including India and South East Asia.
RECOGNIZING MELASMA
Overall, dermatologists can recognize and diagnose melasma by one clinical feature - symmetry.
“Melasma tends to be a predominantly symmetrical hypermelanosis. It affects both sides of the face,” Dr. Desai says. “And, if it’s going to be extrafacial, such as on the forearms, it’s important to note that symmetry before making a diagnosis.”
Mostly, melasma appears only on certain parts of the face. It is generally centrally located, covering areas laterally across the cheeks and in front of the ear. Overall, he says, it is respectful of facial bony contours, rarely impacting any spots above the cheek bone or in the periorbital area.
These characteristics can help dermatologists avoid a misdiagnosis. For example, while patients with acanthosis nigricans experience lateral hyperpigmentation, it is concentrated in the hollows of the cheeks. And, hyperpigmentation found on the lateral parts of the temple or the forehead is most frequently associated with either drug-induced hyperpigmentation or lichens planus pigmentosus.
THE PSYCHOSOCIAL IMPACT
Alongside addressing the physical nature of melasma, it’s also vital for dermatologists to hone in on how the hyperpigmentation affects a patient’s mental state. For many patients, these skin changes can be distressing, pushing them to wear heavy make-up or avoid going out in public, Dr. Desai says.
“This isn’t the way we should encourage our patients to deal with hyperpigmentation,” he says. “We want them to feel comfortable in their own skin, and sometimes that requires counseling.” Dr. Grimes agrees. But, although she readily brings in a counselor to talk with patients who struggle with melasma’s emotional and psychosocial impact, she says her first strategy to help patients develop a healthy perspective about their condition is education. Explaining the chronic nature of the condition, as well as the potential treatment options, is critical to helping them both learn how to manage the condition and feel more comfortable with it.
“We, as caregivers, should never be cavalier and tell patients, ‘It’s just melasma, you’ll be fine,’” she says. “You need to have empathy and compassion for the patient while doing your best to off er them eff ective treatment.”
For some patients, though, the psychosocial angst associated with melasma doesn’t come from within. Providers should also be aware melasma can present a cultural component, says Dr. Kourosh.
“Dermatologists need to be culturally sensitive. In certain cultures, there is significant pressure on patients to have light skin,” she says. “For that reason, having hyperpigmentation can be additionally distressing. That’s why it’s important from the outset to establish healthy goals for treatment - specifically the goal is to have a healthy, even skin tone, not to have light skin.”
Regardless of the reasons behind why a patient experiences distress when learning they have melasma, Dr. Grimes says, dermatologists shouldn’t be timid when utilizing the resources necessary to deliver the highest level of care while helping patients process their diagnosis.Â
References:
1. Roberts WE. Pollution as a risk factor for the development of melasma and other skin disorders of facial hyperpigmentation - is there a case to be made?. J Drugs Dermatol. 2015;14(4):337-41.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.