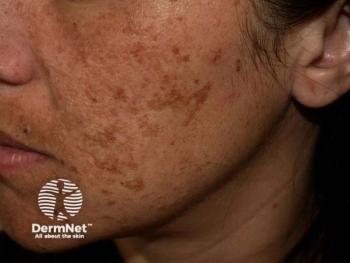
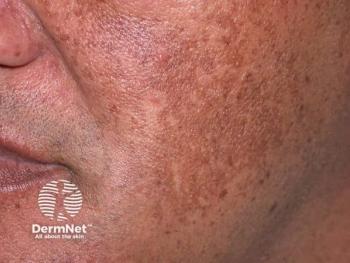
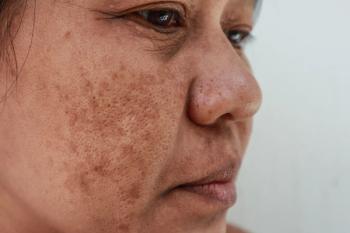
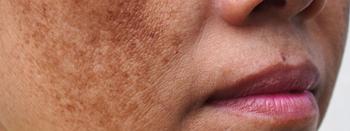
A melasma treatment ladder
A literature review on clinical evidence for melasma treatments suggests an evidence-based treatment ladder.
There’s strong evidence supporting the use of hydroquinone as a first-line treatment for melasma.
The science suggests tranexamic acid is a very promising melasma treatment.
The low-fluence Q-switched laser remains one of the best laser and light options for treating melasma, especially in darker types.
And overall studies suggest that chemical peels do not have better melasma treatment outcomes than topical therapy.
That’s according to a
Author Natalia M. K. Spierings, B.Sc., M.B.B.S., M.R.C.P.(UK), M.R.C.P (Derm), M.B.A., M.Sc., a consultant dermatologist at Queen Mary University of London, UK, conducted a literature search in July 2019, looking for English-language studies published on melasma treatments in the last decade. She found four clinical trials focused on topical hydroquinone as a first-line option; 12 papers on tranexamic acid use; 19 looking at various novel melasma therapies; 42 investigating laser and light treatments; and 11 analyzing outcomes of peels for melasma.
Based on her findings, Dr. Spierings suggests a melasma treatment ladder starting with topical hydroquinone and retinoid-based products as first line for the first three months, at least. If there are no contraindications she recommends also adding oral tranexamic acid 250 mg daily to the first-line treatment. Her second-line melasma treatment recommendation is to use lasers, including low-fluence Q-switched Nd:YAG, picosecond laser and pulsed dye lasers for lighter skin types. Dermatologists and other providers might consider peels as a third-line therapy, with glycolic acid or trichloroacetic acid (TCA) peels showing the greatest efficacy in outcomes for melasma, according to the paper.
A Closer Look
Topical treatments rank high among commonly used melasma therapies. These include photoprotection, since UV light and visible light can worsen pigmentation in all skin types. Dr. Spierings notes that physical, not chemical sunscreens, are recommended for melasma since titanium dioxide and zinc oxide protect against not only UV light but also visible light damage.
Hydroquinone works by inhibiting the tyrosinase enzyme in melanin’s production. Researchers have also found triple combination creams effectively treat melasma. The most recent such FDA-approved cream being Tri-Luma (Galderma), which is hydroquinone 4%, tretinoin 0.05% and 0.1% fluocinolone acetonide.
The author adds the FDA approved nonablative fractional 1550/1540 nm laser for melasma treatment in 2005, and in 2012 approved Lutronic’s Spectra laser, a Q-switched laser for melasma.
“In theory, lasers and light should be effective at treatment melasma, as melanin has a broad absorption spectrum (630-1100 nm) making it amendable potentially to a variety of laser and light sources,” she writes. “It is understood that longer wavelengths can penetrate deeper to reach dermal pigment but melanin absorption is better at shorter wavelengths.”
Among the four studies in the hydroquinone category was a level 1 evidence paper, meaning the study was a properly powered and conducted randomized clinical trial. In that study https://link.springer.com/article/10.1007%2Fs40261-015-0292-8, Gong Z, et al., conducted an 8-week trial of 233 Chinese patients, in which they compared placebo to fluocinolone acetonide, hydroquinone and tretinoin cream for the treatment of moderate and severe facial melasma. They found a statistically significant improvement with study cream.
Collectively, the four studies add to the evidence that hydroquinone 4% works and is safe in the treatment of melasma, she writes.
Tranexamic Acid
Among the 12 trials examining oral, topical and injectable tranexamic acid for melasma treatment, several were high-quality studies supporting tranexamic acid’s use as a monotherapy or in combination with other melasma treatments. None of the trials reported any adverse events, suggesting the therapy is safe. The risk of relapse is high when tranexamic acid is discontinued, so providers might consider it as a long-term therapy option, the author writes.
Novel Options
Nearly 20 of the clinical trials in the review represented novel therapies, including the topical Lumixyl (Envy Medical), an oligopeptide that inhibits tyrosinase; cysteamine, an amino acid thought to inhibit melanogenesis; as well as 75% mulberry extract oil and others. The studies, however, are for the most part small and fail to draw definitive conclusions. So, more research is needed on these novel treatments, according to the paper.
Laser and Light Therapies
Dr. Spierings identified 23 clinical trials analyzing Q-switched Nd:YAG laser treatment for melasma. While the evidence supporting use of the laser is hampered by small sample sizes and no trials that compare the Q-switched Nd:YAG to other melasma therapies, low-fluence Q-switched lasers appear to be the best laser and light option for melasma currently. Q-switched Nd:YAG treatment seems most effective when combined with others, such as intense pulsed light (IPL), glycolic peels and oral treatments, such as tranexamic acid, she reports.
Clinical trials looking at IPL treatment for melasma show only minimal improvement and any positive effects from the IPL need to be maintained with topical therapy.
Studies in the last decade suggest that nonablative fractional lasers in melasma result in mild to moderate improvement at best, with patients relapsing in the months following treatment. The laser to avoid is the 1550 nm, which clinical trials suggest is neither efficacious nor safe for melasma treatment, according to the paper.
There isn’t enough evidence to recommend fractional CO2 lasers for melasma treatment.
But there is promise with picosecond lasers, which have been shown in studies, including level 1 evidence, to significantly improve melasma when combined with topical hydroquinone. Some studies looking at picosecond treatment alone suggest it’s faster and even better than the Nd:YAG but the sample sizes are small and they lack long-term follow up, according to the author.
Peels
Finally, when researchers have compared use of peels for melasma with topical therapy, peels were not superior, resulted in acute side effects and had greater risk for post-inflammatory hyperpigmentation.
References:
Spierings, NMK. Melasma: A critical analysis of clinical trials investigating treatment modalities published in the past 10 years. J Cosmet Dermatol. 2019;00:1– 6.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.