LCV/RNF-alpha-blocking agents link?
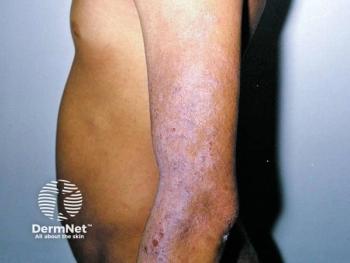
National report — Patients who take TNF-alpha-blocking agents may be at risk for developing leukocytoclastic vasculitis (LCV), according to a new study.
National report - Patients who take TNF-alpha-blocking agents may be at risk for developing leukocytoclastic vasculitis (LCV), according to a new study.
A researcher from the Avera Research Institute, Sioux Falls, S.D., and the Food and Drug Administration (FDA) reports that most study-patients' skin lesions improved once they discontinued taking either etanercept or infliximab.
"There were a couple of case reports of LCV that were reported in association with TNF-alpha blockers in rheumatology journals that interested me in finding out if any more had been reported to the FDA, since this was not seen or reported during the initial studies with the drugs," says lead author Niveditha Mohan, M.D., assistant professor, department of internal medicine, University of South Dakota School of Medicine and a rheumatologist at the Avera Research Institute.
She identified 35 LCV cases - 20 linked to etanercept and 14 that occurred with taking infliximab.
Twenty-two of the total patient population in the study, or 62.8 percent, experienced a complete or marked improvement of the LCV when they stopped taking the TNF-alpha blockers. The skin lesions on three of the etanercept patients continued despite stopping the medication, and one of these patients improved when the researchers switched the patient to infliximab. The LCV recurred in six patients when they restarted the therapy, while three patients experienced a negative rechallenge phenomenon, according to the study.
The author also notes that LCV lesions improved in patients despite continuing to take concomitant medications that have been associated with LCV.
"The purpose of this study is to make physicians aware that TNF blockers can cause LCV as a possible adverse event and that this should be considered in the differential diagnosis when patients on these agents develop LCV," Dr. Mohan says.
While the problem is unusual, it might be underreported, according to Dr. Mohan.
"It is a rare problem, especially when considering that that the reported cumulative incidence of LCV in rheumatoid arthritis over 30 years is about 5 percent," she says. "However, the AERS database is limited by underreporting and, hence, there may potentially be more patients who develop this than those that have been reported. The cases that we reported for the most part had mild disease and for the most part had disease resolution after discontinuing the drug. If they do not have any good alternatives to taking TNF agents, it is worth trying to keep them on the drug to see if the problems improve."
Dr. Mohan tells Dermatology Times that the theories behind the skin reaction with TNF-alpha-blockers include an antigen-antibody reaction or possible induction of an autoimmune diathesis resulting in vasculitic changes. However, there is no definitive information available today, since it is so rare and relatively recently described.
According to Dr. Mohan, dermatologists who see LCV in rheumatoid arthritis patients taking these therapies should first rule out other more common causes of LCV including infection and other drugs, such as cryoglobulinemia or malignancy.
Michael Parks, Centocor spokesperson, says that Remicade (Centocor) has on its label the potential adverse reaction of LCV, but says LCV also occurs in the general population of rheumatoid arthritis patients.
The risk should not dissuade patients from using and doctors from prescribing the medication, Mr. Parks says.
"The risk, even if the event occurs, is so mild that seldom does it lead to discontinuation of therapy, and, when the symptoms of the skin condition occur, they are reversible when the medication is discontinued."
Dr. Mohan agrees that there are well-documented reports of LCV occurring in the rheumatoid arthritis population. But she questions whether this might still be related to medication use because a significant number of patients improved upon discontinuing the drugs, despite continuing on other agents which have been described to cause LCV.
"More importantly, a number of them developed the reaction again (positive re-challenge phenomenon) when they were exposed to the drug a second time," Dr. Mohan says.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.