Latex allergy concerns spur steps to protect healthcare workers
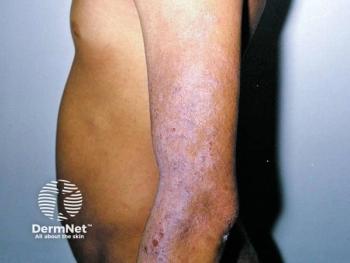
Mild reactions to latex may involve skin redness, rash, hives or itching; more severe reactions can include wheezing and difficulty in breathing.
The use of latex gloves by healthcare employees has grown substantially since the mid-1980s, with the AIDS epidemic largely responsible for the Centers for Disease Control issuing recommendations that gloves be worn as protection against blood-borne pathogens. That recommendation became mandatory in 1991 under the Blood Borne Pathogen Standard established by the Occupational Safety and Health Administration. Today, millions of latex gloves are used by healthcare employees.
But along with the increase in latex glove use, there has been growing concern over the increase in cases of latex allergy reactions, not only among healthcare workers, but among patients who are similarly susceptible.
Latex itself is a nature-based product manufactured from a milky fluid produced by the rubber tree. Latex allergy is a reaction to certain proteins that exist in latex rubber. The majority of healthcare workers will not have an allergic reaction to latex, but it's estimated that nearly 20 percent of them will, after regular exposure from wearing latex gloves, develop an allergy and suffer some degree of complication. Mild reactions to latex may involve skin redness, rash, hives or itching; more severe reactions can include wheezing and difficulty in breathing. In its most severe state, latex allergy can result in death. According to U.S. Food and Drug Administration statistics, latex allergy has been identified as the cause of death in at least 17 healthcare workers since 1989.
"Hand dermatitis, unfortunately, is often trivialized - and it shouldn't be because it serves as a marker that there could be more severe reaction ahead," he says.
Because there is no cure for latex reaction, Dr. Lang says the most effective means by which to deal with latex allergy among healthcare workers is, most obviously, for them to stop wearing latex gloves and opt for those made with synthetic latex that doesn't carry the proteins that set off the allergy. Also, workers identified as having latex allergy should avoid areas where latex is present.
"In recent years, powdered latex gloves have become popular, especially among surgeons who find them more comfortable and feel they allow them a more real touch and firmer grip," Dr. Lang says. "But that powder, which is made from a cornstarch base, can act as a carrier of latex particles. It gets into the air and can be inhaled by workers who are allergic."
Because of this, many hospitals have stopped using powdered latex gloves altogether. In fact, some hospitals have banned latex gloves altogether, powdered or not, and switched to gloves made from synthetic latex. According to Dr. Lang, though the Cleveland Clinic has not issued a ban on latex gloves, usage of the powdered type has dropped dramatically.
Dr. Lang also points out that gloves aren't the only culprit causing problems for latex-allergic employees. Latex is omnipresent in most healthcare facilities because so many items are made of it: stethoscope tubing, blood pressure cuffs, face masks, catheters, bed-railing protectors, even crutch tips - all of these and more can contain latex.
Since these products likely won't be banished any time soon, Dr. Lang suggests screening and testing of workers - now a routine procedure - to determine, among other things, their susceptibility to latex allergy. And, he adds, patients shouldn't be overlooked in screening procedures. The Clinic includes latex-allergy testing for patients as well as employees, both through blood and skin tests. Dr. Lane says it's important to note that blood tests are less sensitive to latex-allergy detection than skin tests. In cases where there's uncertainty, skin tests - which can detect the allergy even when blood tests turn up negative - should be administered to confirm or overrule the allergy's presence.
As an additional step, Dr. Lang suggests that healthcare workers or patients identified as being latex-allergic should wear medical-alert bracelets stating their allergy.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.