Improve Outcomes for Impetigo
Literature update highlights the treatment methods, clinical pearls, and enhancement of outcomes for the disease
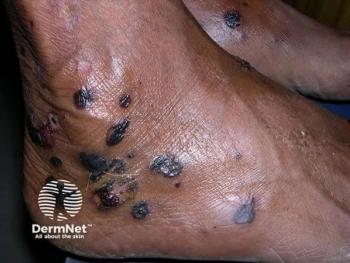
Impetigo is highly contagious and most caused by gram-positive bacteria, presenting as erythematous plaques with a yellow crust. This condition may be painful or itchy. An article posted in the
When treating impetigo, topical antibiotics by themselves or as a combination treatment with systemic antibiotics are used. These antibiotics should combat both Staphylococcus aureus (S aureus) and Streptococcus pyogenes (S pyogenes) to help quicken recovery and lessen the spread of the infection. These treatments are help decreased the chance of complications with the kidneys, joints, bones, and lungs as well as acute rhematic fever, according to the study.2,3,4
For localized, uncomplicated, non-bullous impetigo, topical therapy aloe is the treatment of choice. In cases of bullous impetigo and cases of non-bullous impetigo with more than 5 lesions, deep tissue involvement, systemic signs of infection, lymphadenopathy, or lesions in the oral cavity, systemic antibiotics should be used according to the researchers.
“In areas of high prevalence of methicillin-resistant Staphylococcus aureus (MRSA) or if cultures are positive for MRSA, clindamycin or doxycycline are the preferred treatments,” the authors wrote. “Trimethoprim-sulfamethoxazole is effective against MRSA but should only be used if group A streptococci are not the causative agent, or in addition to an anti-streptococcal antibiotic.”
Pediatric impetigo patients are advised to maintain good personal hygiene and avoid other children during the active outbreak. It is noted that washing hands, linens, clothes, and affected areas that may have encounter infected fluids is recommend and sores can be covered with a bandage to help prevent spread by contact. If impetigo is recurrent, evaluation for carriage of the causative bacteria should be performed.
It was found that 5% of patients with impetigo will develop associated glomerulonephritis, the authors explained, and there is inconclusive evidence whether antibiotics can help reduce the incidence of these events. It usually occurs 1 or 2 weeks after infection and patients may experience fever, hypertension, edema, and hematuria.
Keeping these treatments in mind, will help treatment outcomes, the authors concluded.
Reference:
- Nardi NM, Schaefer TJ. Impetigo. In: StatPearls. StatPearls Publishing; 2021. Accessed October 27, 2021.
http://www.ncbi.nlm.nih.gov/books/NBK430974/ - Loadsman MEN, Verheij TJM, van der Velden AW. Impetigo incidence and treatment: a retrospective study of Dutch routine primary care data. Fam Pract. 2019;36(4):410-416. doi:10.1093/fampra/cmy104
- Smith DRM, Dolk FCK, Pouwels KB, Christie M, Robotham JV, Smieszek T. Defining the appropriateness and inappropriateness of antibiotic prescribing in primary care. J Antimicrob Chemother. 2018;73(suppl_2):ii11-ii18. doi:10.1093/jac/dkx503
- Rush J, Dinulos JG. Childhood skin and soft tissue infections: new discoveries and guidelines regarding the management of bacterial soft tissue infections, molluscum contagiosum, and warts. Curr Opin Pediatr. 2016;28(2):250-257. doi:10.1097/MOP.0000000000000334














