- General Dermatology
- Eczema
- Alopecia
- Aesthetics
- Vitiligo
- COVID-19
- Actinic Keratosis
- Precision Medicine and Biologics
- Rare Disease
- Wound Care
- Rosacea
- Psoriasis
- Psoriatic Arthritis
- Atopic Dermatitis
- Melasma
- NP and PA
- Skin Cancer
- Hidradenitis Suppurativa
- Drug Watch
- Pigmentary Disorders
- Acne
- Pediatric Dermatology
- Practice Management
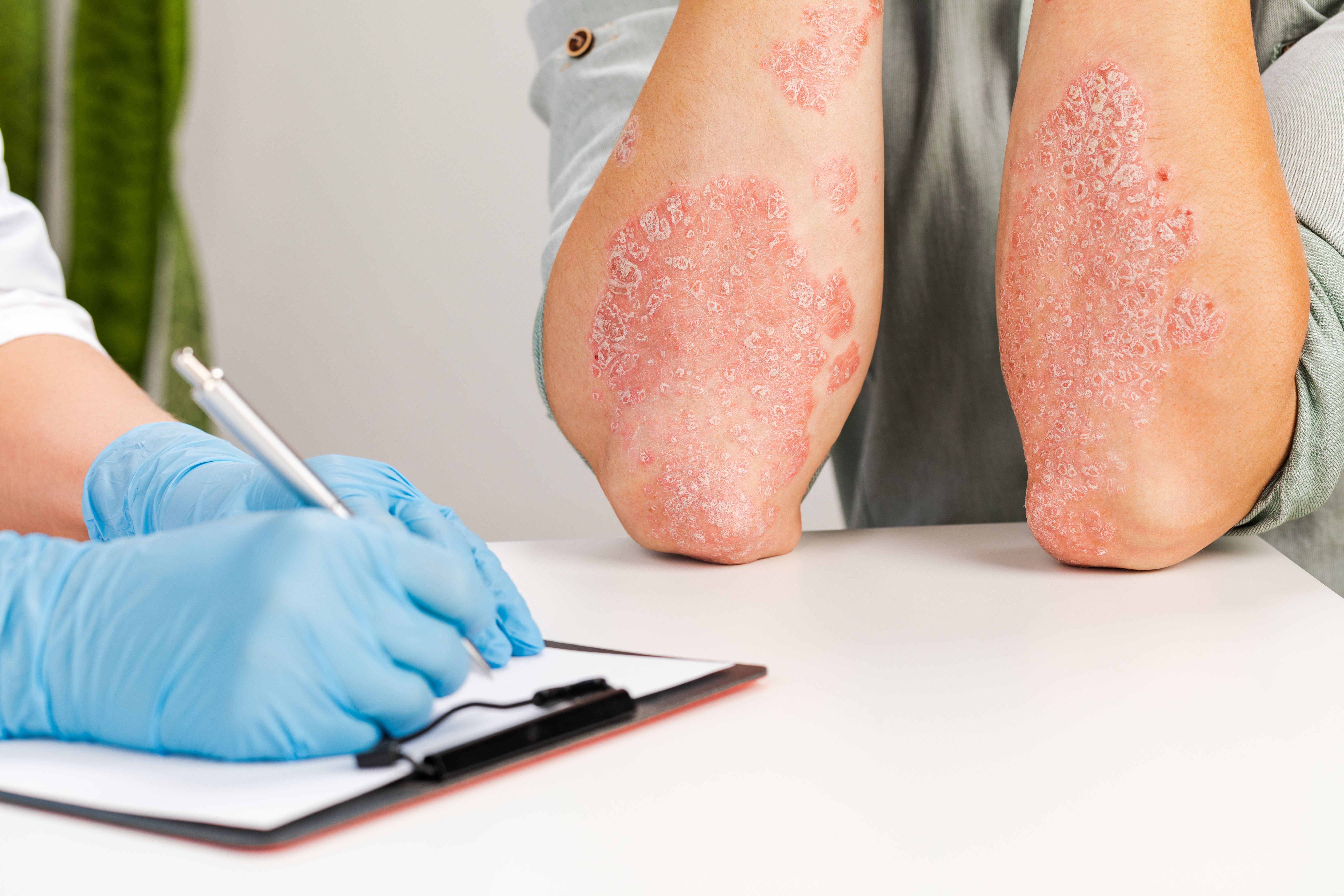
Half of Patients With Psoriasis Receiving Placebo In Clinical Trials Report Adverse Events
A recent review and meta-analysis says this statistic may be due in part to nocebo effects.
Half of patients enrolled in clinical trials of systemic psoriasis therapies who received inert placebo reported adverse events (AEs), according to one study. These findings could potentially be explained by nocebo effects and are important to consider when counseling patients and designing future studies.
This systemic review and meta-analysis is published in Frontiers in Medicine.
“This high baseline rate of AEs may be partially explained by nocebo effects and has important implications for RCT [randomized controlled trial] design and for evaluating side effects in clinical care,” the researchers wrote.
While novel therapeutic agents, such as biologics, have become the gold standard of care, allowing patients to reach near-total or total skin clearance, they may also be associated with negative side effects that impact patient adherence and persistence.
In this study, the researchers aimed to estimate the proportion of patients randomized to placebo who experienced AEs that resulted in treatment discontinuation, infections, and injection- or infusion-related AEs, as well as measure the risk differences (RDs) between patients who received treatment vs placebo.
"The nocebo effect is a well-established phenomenon defined as the occurrence of undesirable side effects secondary to negative patient expectations as opposed to the pharmacologic activity of an intervention," the authors explained.
Studies included in the analysis were placebo-controlled phase 2, 3, or 4 induction or maintenance clinical trials of patients aged 18 years and older with moderate-to-severe plaque psoriasis who received conventional systemic anti-psoriatic agents or placebo. Additionally, these studies reported the frequency and nature of AEs experienced by patients in both treatment and placebo groups.
The analysis included a total of 103 randomized controlled trials (RCTs) of 92 biologic therapies and 38 non-biologic treatments vs placebo. A total of 30,249 patients were randomized to systemic therapy, with 25,067 (82.9%) receiving biologic treatment and 12,940 receiving placebo.
Of these trials, 96 had initial placebo-controlled periods of 16 weeks or shorter. However, 4 clinical trials were excluded due to inability to locate and confirm primary outcomes.
AEs were reported in 96 comparisons (86 biologic and 10 non-biologic), serious AEs (SAEs) in 110 comparisons (91 biologic and 19 non-biologic), and infectious AEs in 101 comparisons (89 biologic and 12 non-biologic).
The overall pooled AE rate in patients who received systemic therapy was 57.1% (95% CI, 54.7-59.5) compared with patients who received placebo (49.8%; 95% CI, 47.1-52.4). The RD was 6.7% (95% CI, 4.6-8.9; P < .00001).
Both biologic and non-biologic groups experienced a higher proportion of infectious AEs compared with placebo groups, while no statistically significant RD in SAEs or AEs leading to discontinuation was identified between systemic therapy and placebo groups.
However, the researchers acknowledged some limitations to the study. First, they noted that there may be other explanations for the high rate of AEs observed in the placebo group, including the accumulation of psoriatic complications and potential misattribution of symptoms from related psoriatic conditions, such as psoriatic arthritis. Second, there was significant heterogeneity between studies when assessing for any AEs that were not fully explained in the metaregression analysis.
Despite these limitations, the researchers believe the study adds to the importance of considering nocebo effects to account for the observed AEs in patients who received placebo.
“We did not identify any significant overall RD in either serious AE or AE leading to discontinuation of therapy between systemic therapy and placebo,” wrote the researchers. “These outcomes inform the interpretation of RCT data and influence clinician-patient communication.”
Reference
Ma B, Park Y-J, Barber K, et al. Nocebo effects in systemic therapies for adult plaque psoriasis: A systematic review and meta-analysis. Front Med. 2024;11. doi:10.3389/fmed.2024.1373520
[This article was originally published by our sister publication, American Journal of Managed Care.]