Getting a handle on epidermolytic hyperkeratosis
In the long term, understanding and addressing the origin of this skin disease - down to its genetic mutation - will prove more beneficial to patients and physicians.
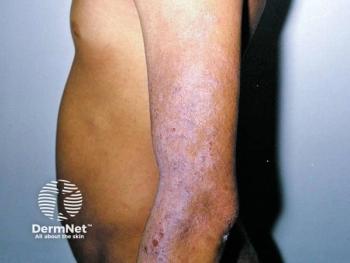
National report - Epidermolytic hyperkeratosis, also called bullous congenital ichthyosiform erythroderma, is a rare autosomal dominant ichthyosis and presents at birth or shortly thereafter as erythema, blistering and/or peeling.
A better understanding of the mutations in keratin production and the molecular mechanisms that cause structural instability in keratinocytes, leading to easy blistering, hyperproliferation and hyperkeratosis, may be the key to finding therapeutic strategies based on gene therapy and may open doors to possible options for a permanent corrective therapy for epidermolytic hyperkeratosis.
In the United States and worldwide, epidermolytic hyperkeratosis is a life-long condition without a gender or race predilection, and affects one in 200,000 to 300,000 persons.
Morbidity includes recurrent infection, sepsis and electrolyte imbalance, which are possible during the neonatal period, and mortality is possible if the sepsis and electrolyte imbalance are not treated properly. The differential diagnoses for epidermolytic hyperkeratosis include epidermolysis bullosa, lamellar and X-linked ichthyoses and staphylococcal scalded skin syndrome (SSSS) as well as Stevens-Johnson syndrome and toxic epidermal necrolysis.
A definitive diagnosis, however, is of paramount importance. This can be achieved through keratin gene defect studies, clinical presentation and careful history-taking, biopsies (diagnostic in de novo cases) and prenatal diagnosis made through analysis of chorionic villus sampling, amniotic cells and fetal skin biopsies. Histologic studies are distinctive but not unique.
According to Dr. Chen, the current treatment modalities are limited to relieving the symptoms of this dominant monogenetic disease. Woundcare for the blistering and aggressive moisturization/emollients are important. Some improvement has been noted with high-dose beta-carotene, systemic retinoids, topical retinoids, 10 percent glycerine, lactic acid, alpha hydroxy acid, calcipotriol, antibacterial soap and urea. However, in the long term, understanding and addressing the origin of this skin disease - down to its genetic mutation - will prove more beneficial to patients and physicians, as well as to healthcare systems worldwide.
Of mice and men
Dr. Chen tells Dermatology Times, "Epidermolytic hyperkeratosis is caused by mutations in either the keratin K1 or K10 genes.
"These mutations lead to defective suprabasal keratinocytes, resulting in blisters and hyperkeratosis. Gene therapy may be the answer in successfully treating this ichthyosis at the molecular level. Our laboratory previously developed an inducible mouse model for epidermolysis hyperkeratosis which is viable, due to the fact that the expression of a mutant K10 allele can be restricted to a focal area of the skin.
"Once the mutant K10 allele is activated in epidermal stem cells by topical application of an inducer, these stem cells continuously give rise to defective progeny that form hyperkeratotic lesions which persist for the life of the mouse. This mouse model also revealed that partial suppression of the mutant K10 allele may be sufficient to eliminate the clinical phenotype."
To test this novel therapeutic strategy, Dr. Chen and his team of researchers developed siRNAs that specifically target mutant K10 transcripts for degradation, without affecting wild type K10 transcripts. He introduced these siRNAs into lentiviral vectors, and subsequently used them to transduce cells expressing both wild type and mutant K10 constructs.
Dr. Chen observed that under these conditions, an efficient knock-down of mutant, but not wild type, K10 transcripts could be achieved. He claims that these results may prove to be a very vital step forward in forging a novel gene therapy and possible permanent corrective therapy for this debilitating skin disease. Dr. Chen and colleagues at the Center for Cutaneous Molecular Biology are currently using this lentiviral vector to transduce keratinocytes isolated from his epidermolytic hyperkeratosis mouse model. They also are testing whether the correction of the epidermolytic hyperkeratosis phenotype can be achieved in vivo when these cells are introduced into a graft on nude mice.
Newsletter
Like what you’re reading? Subscribe to Dermatology Times for weekly updates on therapies, innovations, and real-world practice tips.